Lucian M. Predescu1, M. Tirlea1, Radu Ciudin1,2, Dan Deleanu1
1 „Prof. Dr. C. C. Iliescu” Emergency Institute for Cadiovascular Diseases, Bucharest, Romania
2 „Carol Davila” University of Medicine and Pharmacy, Bucharest, Romania
Abstract: Determining the best percutaneous coronary intervention (PCI) strategy in complex and multiple lesions is very diffi cult based only on angiographic characteristics. There are invasive modalities to determine the hemodynamic sig-nificance of a coronary stenosis and its impact on coronary blood flow, like fractional fl ow reserve (FFR) and instantaneous wave-free ratio (iFR). Atheromatous plaque characterization by intravascular ultrasound (IVUS) is very useful to predict the hemodynamic impact of a coronary stenosis, to determine the exact severity of the stenosis and to characterize the components of the plaque using virtual histology. These invasive hemodynamic and imagistic modalities can guide the PCI strategy in order to obtain the best possible outcome for the patient.
Keywords: PCI, instantaneous wave-free ratio, fractional flow reserve, intravascular ultrasound, invasive coronary he-modynamic evaluation, invasive imagistic evaluation.
INTRODUCTION
Determining the best PCI strategy in complex and multiple lesions is very difficult based only on angio-graphic characteristics. There are invasive modalities to determine the hemodynamic significance of a coro-nary stenosis and its impact on coronary blood flow, like FFR and iFR. Atheromatous plaque characteriza-tion by IVUS is very useful to predict the hemodyna-mic impact of a coronary stenosis, to determine the exact severity of the stenosis and to characterize the components of the plaque using virtual histology. The-se invasive hemodynamic and imagistic modalities can guide the PCI strategy in order to obtain the best pos-sible outcome for the patient.
CASE REPORT
We report the case of a 60-year-old male patient ad-mitted to our clinic with aggravated angina. The past medical history of the patient was unremarkable. His cardiovascular risk factors were stage III hypertension and dyslipidemia.
Clinical examination revealed a controlled blood pressure under antihypertensive therapy without any abnormalities.
The electrocardiogram showed sinus rhythm, heart rate = 75 bpmin, negative and symmetric T waves in the precordial leads. Transthoracic echocardiography revealed a left ventricular ejection fraction of 40%, hypokinesia of anterior and antero-lateral wall and mild mitral and tricuspid valve regurgitation.
Because the patient presented with unstable angina and he had a depressed left ventricular ejection frac-tion we proceeded directly to invasive evaluation wi-thout further non-invasive tests. Coronary angiogram showed a 50% distal left main stenosis (Figure 1), a long lesion on proximal left anterior descending artery (LAD) starting from the ostium to the first diagonal branch, with 70% stenosis (Figure 2) and atheromato-us plaques on left circumflex artery and right coronary artery. Syntax Score was 21, Syntax Score II for PCI was 35.1 (PCI 4-year mortality = 10.3%), Syntax Score for coronary artery bypass grafting (CABG) was 30.7 (CABG 4-year mortality = 7.2%) and EuroSCORE II was 1.02%.
Heart Team analyzed the case and based on Syntax Score and Syntax Score II results decided that the patient was a good candidate for both PCI and CABG with a low surgical risk. The informed decision of the patient was in favor of PCI. There were some questi-ons about the best modality to revascularize the pati-ent by PCI: we need to treat the distal left main lesion that can potentially complicate the procedure, or we can treat the proximal LAD lesion only?
In order to guide our PCI decision, we investigated the hemodynamic significance of left main and LAD lesions using iFR and iFR pull-back. iFR result in the distal segment of LAD was 0.79 showing that the com-bined left main and LAD lesions had a signifi cant im-pact on coronary flow (Figure 3). This measurement demonstrated the presence of ischemia in the myo-cardial territory supplied by LAD. In order to see the individual contribution of left main lesion and LAD le-sion to the ischemia we performed iFR pull-back. iFR result, distal to the left main lesion but proximal to the LAD lesion, was 0.93 showing that the left main lesion had a non-significant impact on coronary flow (Figure 4). According to iFR evaluation of the combined lesi-ons, if we treat by PCI the LAD lesion only, the iFR measurement after PCI must be 0.93 that is negative for ischemia.
To treat only the LAD lesion, we had to characteri-ze the left main and LAD plaque distribution, to decide if we can stent only up to the ostium of the LAD, to choose the right size for the stent in order not to dissect the left main. For those purposes we perfor-med IVUS in the left main and LAD. IVUS showed that the atheromatous plaque started in distal left main and affected the entire proximal LAD to the first diago-nal branch. According to IVUS minimum lumen area (MLA) on proximal LAD was 2.8 mm2 with a 72.6% stenosis (Figure 5), MLA at the ostium of LAD was 6.2 mm2 with a 53.9% stenosis (Figure 6) and MLA on distal left main was 10.2 mm2 with a 52.5% stenosis (Figure 7). IVUS confirmed the severity of stenosis on proximal LAD and it showed a large MLA at the os-tium of LAD and in distal left main.
Although the distal left main lesion was hemodyna-mically non-significant based on iFR and IVUS mea-surements we further characterized the lesion using virtual histology. IVUS using virtual histology showed that the distal left main lesion was a stable lesion with mostly fibrous and fatty-fi brous tissue and a small ne-crotic core located far from the intima (Figure 8).
After predilatation, we implanted a 3.0×26 drug eluting stent on proximal LAD from the ostium to the first diagonal branch without touching the left main
lesion. The final angiographic result was good (Figure 9, 10). IVUS confirmed the optimal result after PCI and it excluded any left main dissections. iFR result in the distal LAD after PCI was 0,94 that is negative for ischemia (Figure 11).
The evolution of the patient was good without any procedural related complications. He was treated with a beta blocker, dual antiplatelet therapy with aspirin and clopidogrel, an angiotensin-converting enzyme in-hibitor and a calcium channel blocker for hypertension and a statin. The patient was discharged the following day without angina.
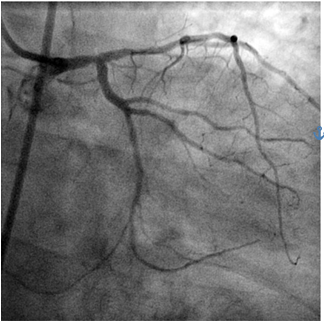
Figure 1. Coronary angiogram – left coronary artery (caudal projection): 50% distal left main stenosis.
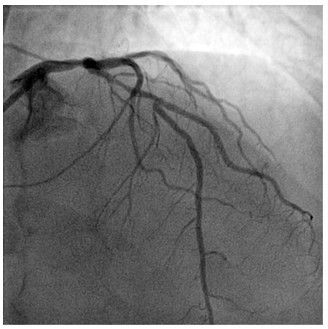
Figure 2. Coronary angiogram – left coronary artery (cranial projection): a long lesion on proximal left anterior descending artery starting from the ostium to the first diagonal branch, with 70% stenosis.
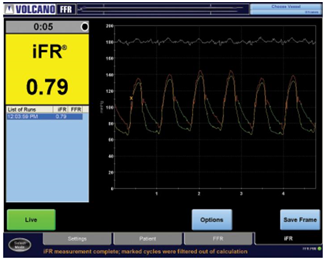
Figure 3. iFR result in the distal left anterior descending artery before PCI.
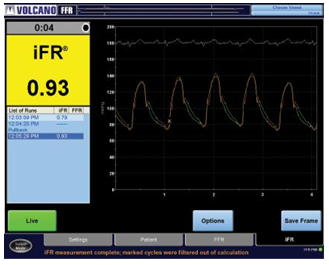
Figure 4. iFR result distal to the left main lesion before PCI.
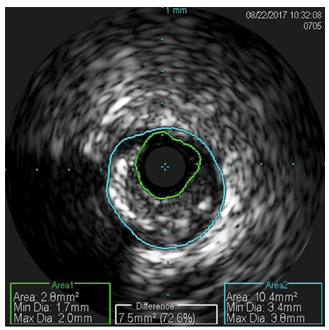
Figure 5. Intravascular ultrasound – minimum lumen area on proximal left anterior descending artery was 2.8 mm2 with a 72.6% stenosis.
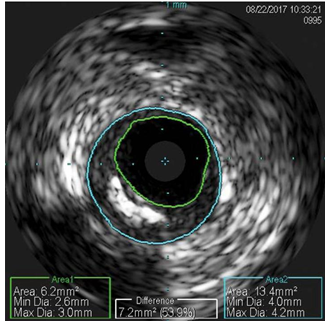
Figure 6. Intravascular ultrasound – minimum lumen area at the ostium of left anterior descending artery was 6.2 mm2 with a 53.9% stenosis.
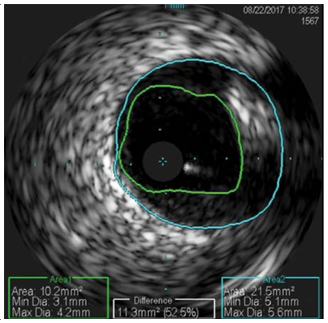
Figure 7. Intravascular ultrasound – minimum lumen area on distal left main was 10.2 mm2 with a 52.5% stenosis.
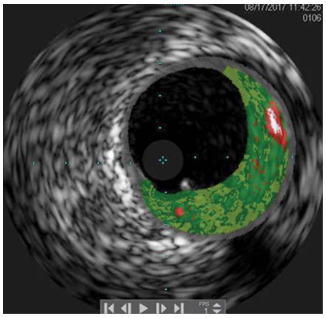
Figure 8. Intravascular ultrasound with virtual histology on distal left main showed a stable lesion with mostly fibrous (dark green) and fatty-fibrous (light green) tissue and a small necrotic core (red) located far from the intima.
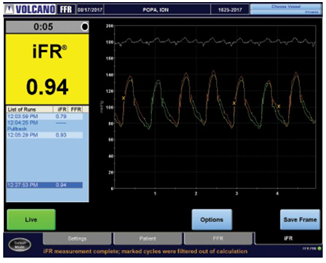
Figure 9. iFR result in the distal left anterior descending artery after PCI.
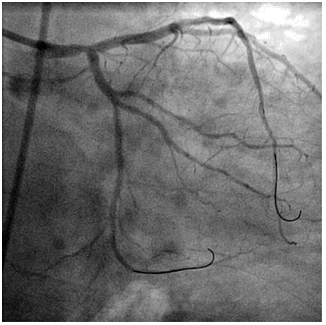
Figure 10. Coronary angiogram – left coronary artery (caudal projection) – final angiographic result after PCI.
DISCUSSIONS
This presentation highlights the case of unstable angina in a patient with moderate distal left main stenosis and a severe proximal LAD stenosis, that was suitable for revascularization by either PCI or CABG. In order to choose the best PCI strategy, we needed to characterize the coronary lesions from the anatomical and hemodynamic point of view.
FFR is the gold standard in predicting the hemodynamic severity of coronary stenosis1,2. FFR is the ratio of mean distal coronary pressure to mean aortic pressure during maximum hyperemia, usually induced by adenosine infusion, and represents the percentage of normal fl ow across a coronary stenosis. The ische-mic threshold for FFR was established to be ≤0.80 in FAME 1 and FAME 2 trials 3. This is now the recom-mended ischemic reference standard for the invasive assessment of myocardial ischemia. DEFER (Percutane-ous Coronary Intervention of Functionally Non-significant Stenosis) trial showed that it is safe to defer PCI of nonsignificant stenosis determined by FFR. At 5-year follow-up, the deferred group had a rate of death or myocardial infarction that was lower than the rate in the PCI group 4.
A newer physiological index used to assess the se-verity of stenosis is iFR. The iFR is calculated by mea-suring the resting pressure gradient across a coronary lesion during the portion of diastole when microvas-cular resistance is low and stable. Benefits of iFR inclu-de the ability to obtain an instantaneous hemodynamic lesion assessment without the need to administer a hyperemic agent, such as adenosine, removing the risk for adverse events induced by adenosine. Recently, iFR-SWEDEHEART (The Instantaneous Wave-free Ra-tio versus Fractional Flow Reserve in Patients with Stable Angina Pectoris or Acute Coronary Syndrome) and DEFI-NE-FLAIR (Functional Lesion Assessment of Intermediate Stenosis to Guide Revascularization) trials showed that coronary revascularization guided by iFR was nonin-ferior to revascularization guided by FFR with respect to the risk of major adverse cardiac events at 1 year5,6. However, there are limited data about the utility of iFR in the assessment of intermediate left main steno-sis. The iFR measurement had a grey zone between 0.86 and 0.93 when it was recommended to perform additional measurements, like FFR. An iFR ≤0.85 was considered positive for ischemia and an iFR ≥0.94 was considered negative for ischemia. Recently, the ische-mic threshold for iFR was changed to 0.89, and the grey zone was abandoned. So, an iFR ≤0.89 is now considered positive for ischemia7.
In this case, we chose to use iFR measurement to assess the hemodynamic significance of left main and proximal LAD lesions because iFR is a little safer procedure than FFR with the same good results. The iFR value distal to the LAD stenosis was 0.79 that is positive for ischemia and determine the need for re-vascularization. This value measured the combined effect on coronary flow of the left main stenosis and the proximal LAD stenosis. In order to determine the exact contribution of each coronary stenosis to the impairment of coronary flow we performed iFR pull-back. During iFR pull-back we saw that the iFR value between the left main lesion and LAD lesion was 0.93. This value is negative for ischemia. The conclusion was that the left main stenosis had a non-significant impact on coronary flow and the LAD lesion was the main obstacle that was responsible for ischemia in our pati-ent. Based on these results we decided that it is enou-gh to treat the LAD lesion only in order to relieve the myocardial ischemia. To treat only the LAD lesion, we had to characterize the left main and LAD plaque dis-tribution by IVUS and to choose the right size of the stent in order to avoid stent edge dissection in the left main if we stent the LAD up to the ostium.
IVUS is a catheter-based imaging modality that pro-vides high-resolution cross-sectional images of the co-ronary artery, enabling measurements of luminal and vessel areas1. Using IVUS we can accurately measure the minimum lumen area, the size of the vessel, the amount of plaque and the severity of the stenosis. IVUS can predict the hemodynamic signifi cance of a coronary stenosis by measuring the MLA. In non-left main lesions, a MLA <3 mm2 had the best sensitivity and specificity for correlating with FFR <0.80 1. In our case the MLA of proximal LAD lesion was 2.8 mm2 predicting a hemodynamically significant lesion. In left main lesions, a MLA <6.0 mm2 predict an FFR <0.758,9. There are data showing that it is safe to defer the left main revascularization if the MLA is >6.0 mm2 10. In our case the MLA of left main stenosis was 10.2 mm2 that is another reason besides iFR value to treat only the LAD lesion.
IVUS can assess using virtual histology the plaque morphology. Based on the amplitude and frequency of reflected ultrasound signals IVUS can detect the fibrous tissue, the fatty-fibrous tissue, the calcium and the necrotic core. It can estimate de percentage of each type of tissue in the atheromatous plaque 1. In our case the left main lesion had a small necrotic core, that was far from the intima, and a lot of fi brous and fatty-fi brous tissue. These morphologic elements cha-racterize a stable atheromatous plaque that has a small likelihood for adverse events.
Based on the invasive hemodynamic and imagistic evaluation we decide to treat only the LAD lesion, in order to keep it simple and to avoid a complicated left main PCI that would have been unnecessary to relieve the patient ischemia. The iFR value on distal LAD after PCI was 0.94, as we predicted before PCI, showing that the myocardial ischemia was treated. The evolu-tion of the patient was good with this individualized strategy.
CONCLUSIONS AND IMPLICATIONS FOR CLINICAL PRACTICE
Coronary angiogram offers limited information in or-der to plan the PCI strategy based on anatomical cha-racteristics only, mostly in patients with complex and multiple coronary lesions. An important goal of PCI in a symptomatic patient is to relieve the myocardial ischemia. Treating all coronary lesions seen on coro-nary angiogram without certifying the hemodynamic significance of these lesions can complicate the proce
dure and jeopardize the clinical outcomes of the pati-ent. There are a lot of data showing that guiding the PCI by FFR, iFR and IVUS evaluation improves the out-comes of the patient. There are clear cut-offs for all these invasive assessments that can guide us to choose the best PCI strategy for each patient.
Conflict of interest: none declared.
References
1. Lotfi, A., et al., Expert consensus statement on the use of fraction- al flow reserve, intravascular ultrasound, and optical coherence tomography: a consensus statement of the Society of Cardiovascular Angiography and Interventions. Catheter Cardiovasc Interv, 2014. 83(4): p. 509-18.
2. Yong, A.S., et al., Fractional flow reserve assessment of left main stenosis in the presence of downstream coronary stenoses. Circ Cardiovasc Interv, 2013. 6(2): p. 161-5.
3. Melikian, N., et al., Fractional flow reserve and myocardial perfusion imaging in patients with angiographic multivessel coronary artery disease. JACC Cardiovasc Interv, 2010. 3(3): p. 307-14.
4. Zhang, D., et al., Fractional flow reserve versus angiography for guiding percutaneous coronary intervention: a meta-analysis. Heart, 2015. 101(6): p. 455-62.
5. Gotberg, M., et al., Instantaneous Wave-free Ratio versus Fractional Flow Reserve to Guide PCI. N Engl J Med, 2017. 376(19): p. 1813-1823.
6. Davies, J.E., et al., Use of the Instantaneous Wave-free Ratio or Fractional Flow Reserve in PCI. N Engl J Med, 2017. 376(19): p. 1824-1834.
7. Ding, W.Y., S. Nair, and C. Appleby, Diagnostic accuracy of instantaneous wave free-ratio in clinical practice. J Interv Cardiol, 2017. 30(6): p. 564-569.
8. de la Torre Hernandez, J.M., et al., Prospective application of pre-defined intravascular ultrasound criteria for assessment of interme-diate left main coronary artery lesions results from the multicenter LITRO study. J Am Coll Cardiol, 2011. 58(4): p. 351-8.
9. Predescu L.M, Zarma L, Platon P, Postu M, Bucsa A, Croitoru M, De-leanu D, Ginghina C, Current treatment of left main coronary artery disease. Cor et Vasa 58 (2016) e328-e339.
10. McDaniel, M.C., et al., Contemporary clinical applications of coro-nary intravascular ultrasound. JACC Cardiovasc Interv, 2011. 4(11): p. 1155-67.
 This work is licensed under a
This work is licensed under a