Download PDF
https://doi.org/10.47803/rjc.2020.30.2.222
Mihaela Bolog1, Mihaela Dumitrescu1, Florentina Romanoschi1, Elena Pacuraru1, Alina Rapa1
1 „Prof. Dr. Agrippa Ionescu” Emergency Clinical Hospital, Bucharest, Romania
Abstract: Objective – To examine the utility of global longitudinal strain imaging diastolic index (SI-DI) in the assessment of patients with suspected obstructive coronary artery disease (CAD). Methods – We performed rest 2 D standard echocardiography and strain imaging in 30 healthy subjects and in 148 patients with normal or mildly reduced ejection fraction and indication for coronarography for suspected obstructive CAD. Standard echocardiographic and strain parameters were analysed. Results – Global SI-DI was signifi cantly lower in the selected vs control group (p <0.001). After coronarography patients were divided in three subgroups: 74 patients with more than 50% obstruction in any major artery, 26 patients with previous revascularisation but no significant obstructive lesions at present and 48 patients without obstructive artery disease. Average global SI- DI was significantly lower in the subgroup with obstructive CAD vs the other two subgroups (p<0.05).Global SI-DI lower than 0.5 had a good sensitivity (84%) and a reasonable positive predictive value (52%) for detection of obstructive CAD. Conclusions – Global SI-DI is significantly lower in patients with obstructive CAD and normal or mildly reduced ejection fraction compared with normal subjects. A cut off value lower than 0.5 selects patients with a higher probability of obstructive CAD.
Keywords: strain imaging, coronary artery disease.
Rezumat: Obiectivul studiului – Este de a examina utilitatea indicelui diastolic global longitudinal(SI-DI ) evaluat prin ecocardiografie 2D metoda speckle tracking în evaluarea pacienţilor cu risc de boală coronariană obstructivă (CAD). Meto-da – 30 de subiecţi sănătoşi şi 148 de pacienţi cu suspiciunea de CAD cu indicaţie pentru coronarografie au fost examinaţi ecocardiografi c bidimensional standard şi speckle tracking. Rezultat – SI-DI global a fost semnifi cativ mai mic la pacienţii cu suspiciunea de CAD vs grup de control (p < 0.001). După coronarografie pacienţii au fost împărţiţi în trei subgrupe: 74 de pacienţi cu mai mult de 50% obstrucţie coronariană, 26 de pacienţi cu revascularizare anterioară, dar fără leziuni obstructive semnificative în prezent şi 48 pacienţi fără leziuni. Valoarea medie a SI-DI global a fost semnifi cativ mai mică în subgrupul pacienţilor cu leziuni obstructive vs celelalte două subgrupe (p < 0,05). SI-DI global mai mic de 0,5 a avut o sensibilitate de 84% şi o valoarea predictivă pozitivă de 52% pentru detectare CAD. Concluzii – SI-DI global este semnifi cativ mai mic la pacienţii cu leziuni coronariene obstructive şi fracţia de ejecţie normală sau uşor redusă în comparaţie cu subiecţii normali. O valoare mică decât 0,5 selectează pacienţii cu o probabilitate mai mare de CAD. Cuvinte cheie: imagistica de strain, boală coronariană obstructivă.
INTRODUCTION
Strain is a measurement of dimensional change or de-formation. Imaging techniques have been developed to quantify myocardial strain in clinical practice1. The most widely used is speckle tracking echocardiography whi-ch has been proved to have an important role in evalu-ation of subtle left ventricular systolic disfunction in various clinical conditions (assessment of cardiotoxicity, valvular disease, left ventricular hypertrophy, ischemic heart disease). Different strain patterns could orient the diagnostic (amyloidosis, pathologic hypertrophy, regional disfunction). The role of systolic and/or diastolic strain analysis in regional wall motion abnormali-ties in ischemic heart disease was validated in previous studies2-5. Post-systolic shortening by speckle tracking echocardiography is an independent predictor of cardiovascular events6 and post-systolic strain index, a quantitative measurement of post systolic shortening, is a parameter that can identify ischemic segments7. There have been proposed several mechanisms for ischemia- related diastolic abnormalities: reduced systolic contraction followed by decreased elastic recoil and subsequently decreased early diastolic untwisting and ventricular suction, reduced chamber compliance by fibrotic changes, delayed active contraction or late passive myocardial contraction (post-systolic thickening)8,9. Diastole is also an active process, energy – de-pendent directly affected by hypoxemia. Ischemia – induced delay in regional relaxation (stunned regional diastolic dysfunction) in the perfusion territory of the involved coronary artery was demonstrated in previous studies. Ishii10 demonstrated that impaired diastolic function with delayed outward wall motion persisted beyond recovery after ischemia. Quantitative analysis of regional diastolic dysfunction can be obtained by several echocardiographic methods like color kinesis, tissue doppler imaging and by speckle tracking strain imaging. Several studies demonstrated previously that analysis of diastolic images by color kinesis offers a quantitative evaluation of global diastolic function. Harada11 defined a color kinesis diastolic index (CK-DI) as the degree of left ventricular segmental expansion during the first 30% of diastole and proved that it co-relates with standard diastolic parameters. The idea of using one third of diastole comes from a previous study which reported that peak filling rate during the first third of diastole were significantly lower at rest in patients with coronary artery disease than in normal patients, despite similar heart rates12.Validated tissue doppler imaging (TDI) parameters of left ventricular filling pressure (E/E´) are indirect measures of ventricular filling method is angle dependent, influenced by preload and has a relatively broad “grey zone”. Strain imaging is less influenced by these factors and offers both regional and global characterisation of myocardial deformation. Strain imaging diastolic index was re-ported to be a sensitive marker to detect LV regional delayed relaxation during early diastole in myocardial ischemia induced by exercise8 and it proved to be associated with severe coronary artery stenosis13.Rest global longitudinal SI-DI was shown to correlate with left ventricular (LV) filling pressures in suspected coronary artery disease14 and with NTproBNP in hypertensive patients15. However, usefulness of global SI-DI in the assessment of patients with suspected CAD must be established.
METHODS
We performed 2 D standard echocardiography and strain imaging in 30 healthy subjects and in 148 patients with suspected obstructive CAD, normal or borderline ejection fraction (EF) and indication for coronarography. Criteria for referral to coronary arteriography are presented in Table 1. Patients with severe or rest symptoms, severe valvulopathy, arrythmia and/ or EF less than 45% were excluded. Standard echocardiographic parameters left ventricular global longitudinal strain (LVGLS) and global SI-DI were analysed. The patients subsequently underwent coronary angiographic examination.
After coronarography patients were divided in three subgroups: 74 patients (50%) had more that 50% coronary obstruction in any major artery, 26 patients (17.5%) had previous revascularisation but no significant obstructive lesions at present and 48 patients (32.5%) were without obstructive artery disease. General and echocardiographic characteristics in controls and selected patients before and after coronary angiographic examination are presented in Table 2 and 3.
Standard two-dimensional echocardiography Transthoracic echocardiography was performed using bidimensional, M-mode, pulse wave Doppler, color-flow Doppler, tissue doppler and speckle tracking imaging with an ultrasound system Philipps Epiq 7G. Images were acquired and analyzed according to current recomandations16. Atrial and ventricular dimensions were measured, ejection fraction was calculated with Simpson method, diastolic dysfunction indices accor-ding to recommendations17. The left ventricular mass was calculated with Devereux formula. Atrial volume has been indexed to the body surface area. Pulsed-wave Doppler imaging was used to measure mitral valve inflow velocity peak at early (E) and late diastole (A) in a standard manner.

Tissue Doppler imaging of the left ventricular longitudinal function was used to determine mitral annular velocities in early (e´) diastole at both septal (e´ septal) and lateral (e´ lateral) annulus. For each examination E/e´ and average e´ (e´ septal + e´ lateral /2) were calculated.
Speckle tracking two-dimensional echocardiography
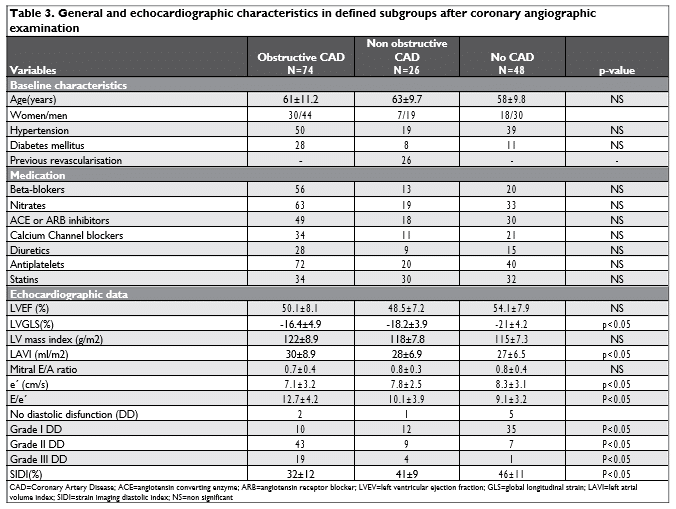
Echocardiographic images for speckle tracking analysis were acquired in 2-,3-, and 4- chamber views at a high frame rate (60-80 frames/s). Images were obtained during a transient breath hold and stored for offline analysis. Left ventricular global longitudinal strain was measured using the commercial available software , on PC workstation (QLAB,7.0).End diastole was defined as the time of R-wave peak and end systole as time of aortic closure, which was defined automatically on 2-D echography. After initialization of strain measurement, the computer automatically defined the region of interest (ROI), which was manual adjusted, when necessary. There were recorded 1-3 stable consecutive cardiac cycles for each view. Atrial and ventricular premature beats were excluded. Strain was measured automatically in each segment for each view and subsequently accepted by the person who performed the analysis. Peak strain was defined as the highest strain value that was acquired in the longitudinal direction through the cardiac cycle. Global longitudinal strain and peak strain for each segment were displayed in “bull’s eye” view. Strain curves were displayed for each segment in all cardiac cycle. Average end -systolic strain for each view was measured at the closure of aortic valve, displayed on strain curves graphic (Figure 1). Global SI-DI was determined as end-systolic strain minus strain at 1/3 of diastole (b) (measured on strain curves graphic using the linear markers), repor-ted on end-systolic strain (a). The formula used for global SI-DI calculation was (a-b)/a. Global longitudinal SI-DI was calculated as the average of global SI-DI obtained from the 3 apical views9-11.
Statistical analysis
The obtained data were expressed as mean values standard deviations. The relationship between the continuous variables was calculated using Pearson´ s correlation coefficient. Comparison between means of two groups with continuous variables was performed using Student’s t-test and for categorical variables using 2 and between several groups using ANOVA analysis. Univariable and multivariable Cox proportional hazards models were used to calculate hazard ratios (HR). Analysis was performed using SPSS version 17 for Windows. A p value < 0.5 was considered significant.
RESULTS
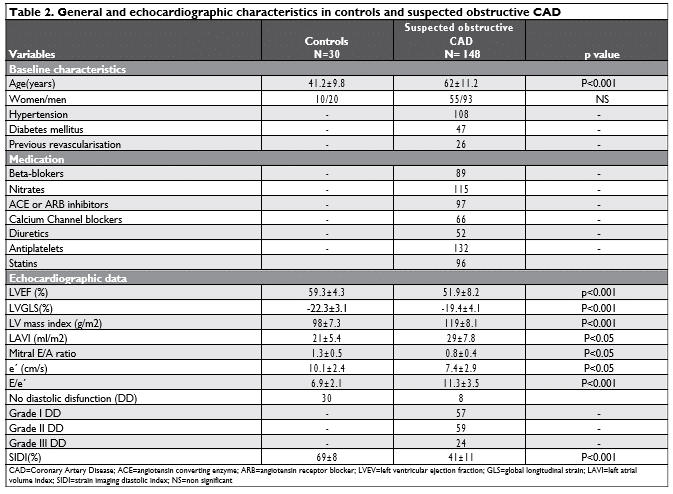
General and echocardiographic data are presented in Table 2. Of the 148 patients selected 55 were women, mean age was 62 ± 11 years old, 108 were hypertensive, 47 had diabetes mellitus and 26 were previously revascularized. Selected patients had cardiovascular risk factors and at least one episode of angina or angina equivalent in their medical history (not in the last month). All patients were under treatment, class of medication being mentioned in Table 2. At the enrolment patients had mild or no symptoms. Healthy subjects were significantly younger (41.2± 9.8 years old) and had normal echocardiographic examination. Mean EF in studied group, although in normal range was significantly lower than in control group (51% vs 59% respectively, p<0.001).
Coronary angiography data
Elective coronarography was performed in all selected patients. Indications for coronarography are presented in Table 1. After coronarography patients were divided in three subgroups: 74 patients (50%) had more that 50% coronary obstruction in any major artery, 26 patients (17.5%) had previous revascularisation but no significant obstructive lesions at present and 48 patients (32.5%) were without obstructive artery disease (Table 3). Class of medication did not differ in the three subgroups (p<0.05). Standard echocardi-ographic data showed no significant difference in the ejection fraction, left ventricular mass index and mitral E/A ratio, in the defined subgroups. Mean LVEF was different in subgroups but with no statistical significance (50 % in obstructive CHD vs 48 % in non-obstructive CHD vs 54 % in no CHD, p= 0.089). Left atrial volume index, e´ and E/e´ were significantly different in obstructive CHD than in non-obstructive CHD or no CHD (p<0.05).
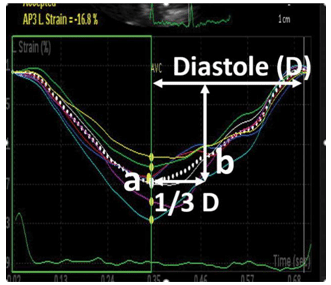
Figure 1. Calculation of Global Longitudinal Strain Imaging Diastolic In-dex (GLSI-DI) explained on strain curves. GLSI-DI was calculated with the formula: GLSI-DI=a-b/a where a=average longitudinal strain at the closure of aortic valve and b=longitudinal strain at 1/3 of diastole, in 2-,3- 1nd 4 chambers views.
Strain analysis
Mean left ventricle global longitudinal strain (LVGLS) was significantly lower (in absolute value) in angina vs control group (-19.4% vs -22%, p<0.001). In specified subgroups GLS was lower in absolute value in obstructive CHD than in non-obstructive CHD and no CHD (-16% vs -18 % vs -21%, p<0.05). Global SI-DI was significantly lower in angina pectoris vs control group (0.41 vs 0.69, p <0.001). Average global SI-DI was significantly lower in the subgroup with obstructive coronary disease vs the other two subgroups (0.32 vs 0.41 and 0.46 respectively, p<0.05) (Figure 2 and 3).
In univariate analysis lower global SI-DI was associated with a higher risk of coronary artery disease (Hazard Ratio 1.39, 95% Confidence Interval 1.09-1.49; p<0.05 per 0.1% decrease).There was significant correlation between reduced global SI-DI and the presence of coronary artery disease (r=-0,54, P<0.05), hypertension (r=- 0.61, p<0.05), left ventricular hypertrophy (r=-0.68, p<0.05), diastolic dis-function (r=-0.69, p<0.05). Although LVGLS was also significantly different between subgroups (p<0.05), we found a week correlation between global SI-DI and LVGLS (-0.39, p=0.063). Global SI-DI lower than 0.5 had a good sensitivity (84%) and negative predictive value (71%) and a lower specificity (40%) and positive predictive value (52%) for detection of obstructive CAD.
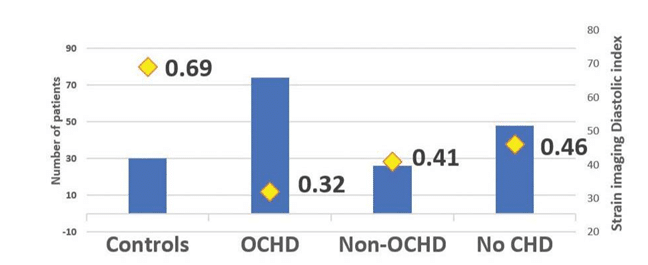
Figure 2. Mean value of longitudinal global strain imaging diastolic index (GLSI-DI) in healthy controls and subgroups of angina pectoris patients. (OCHD=obstructive coronary heart disease). GLSI-DI is significantly lower in OCHD vs healthy subjects (0.32 vs 0.69), subgroup with non obstructive CHD (0.32 vs 0.41) and vs subgroup without CHD (0.32 vs 0.46).
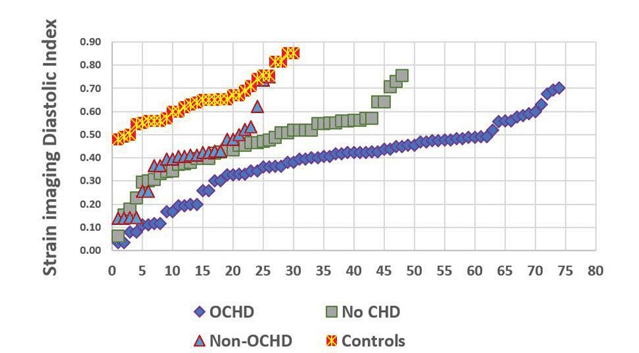
Figure 3. Graphic representation of the values of longitudinal strain imaging diastolic index (GLSI-DI) in each individual patient in healthy subjects (controls) and in specified subgroups defined after coronarography (OCHD=obstructive coronary heart disease subgroup, non-obstructive CHD subgroup=Non-OCHD and without CHD subgroup=no CHD).
DISCUSSION
In the current study we demonstrated the usefulness of a new parameter global SI-DI, assessed by 2D speckle tracking, in the diagnostic evaluation for obstructive coronary heart disease. The selected patients had a high probability of coronary artery disease18 or have been previously revascularized. Systolic left ven-tricular function was normal or mildly reduced (EF ≥ 45%). Global SI-DI was significantly lower in selected group vs a healthy controls (0.41 vs 0.69, p <0.001). After coronarography we further divided the selec-ted group in three subgroups: with more that 50% coronary obstruction in any major artery (50%), with previous revascularisation but no significant obstructive lesions at present (17.5%) and without obstructive artery disease. (32.5%). Global SI-DI was significantly lower in each subgroup vs healthy patients (p<0.001) and in the subgroup with obstructive coronary disease vs the other two subgroups (0.32 vs 0.41 and 0.46 respectively, p<0.05). Ejection fraction did not differ significantly between subgroups but LVGLS was lower (in absolute value) in obstructive CAD and in non-obstructive CAD vs no CAD (p<0.05). We found a significant correlation between lower values of global SI-DI and the presence of diastolic disfunction. Grade II and III diastolic disfunction, evaluated according to 2016 ASE/EACVI recommendations17 had a higher incidence in obstructive CAD group vs non obstructive CAD and no CAD (83% vs 50% vs 16% respectively) indicating that global SI-DI is also a parameter for assessing diastolic disfunction with high filling pressure. The weak correlation between global SI-DI and LVGLS could be explain by the fact that we used end systolic strain not peak systolic strain in the calculation formula and all our patients were a high cardiovascular risk group with other factors that could contribute to a modified LVGLS. Univariate analysis showed that lower global SI-DI was associated with a higher risk of coronary artery disease. The cut off value of 0.5, selected in previous studies13-15, had in our study a good sensitivity (84%) and negative predictive value (71%) thus it can be used to rule out significant coronary artery stenosis in rest echocardiography. The results of our study were not strong enough to demonstrate that rest global SI-DI is an independent parameter for prediction of obstructive CAD. This could be explained by the fact that global SI-DI evaluates alterations in early diastole that can appear in left ventricular hypertrophy, infiltrative myocardial disease or myocardial fibrosis. The positive predictive value at the cut off 0.5 was relatively low (52%) but as shown in univariate analysis the lower the value the higher the probability of having obstructive CAD especially when used in appropriate clinical context (angina pectoris, positive stress test).
Previous studies demonstrated that diastolic left ventricular abnormalities are early signs of myocardial ischemia and persists longer than transient systolic disfunction20-22. Ishii8 demonstrated in 2009 that evaluation by 2D strain imaging of exercised-induced post-is-chemic left ventricular relaxation or diastolic stunning is a reliable method for the detection of CAD. They proposed a new parameter, strain imaging segmental transverse diastolic index as a marker of regional acute ischemia (post-exercise) and proved that this parameter can improve diagnostic accuracy of stress echocardiography for the detection of significant CAD. Several studies showed that diastolic dysfunction persists longer, even 6 months after successful reperfusion in acute myocardial infarction23. Kimura13 showed that rest radial, longitudinal and transverse global SI-DI de-creased significantly in severe stenosis segments and identified a cut off value of 50% for transverse SI-DI for predicting segments with severe stenosis with a sensitivity of 0.79. Chiang14 demonstrated that global SI-DI corelated with NT-proBNP levels in asymptomatic hypertensive patients with preserved ejection fraction and concluded that global SI-DI might serve as a novel echocardiographic parameter for assessing diastolic function. Furthermore, global SI-DI may reflect elevated left ventricular filling pressure and its rapid change better than conventional diastolic parameters in patients with suspected CAD14.
2019 ESC guidelines of the diagnosis and management of chronic coronary syndromes recommends to use as initial test non-invasive functional imaging for myocardial ischemia or coronary CTA for the diagnosis of CAD in symptomatic patients in whom obstructive CAD cannot be excluded by clinical assessment19. In clinical practice exclusion of CAD by clinical evaluation is frequently difficult. We demonstrated that rest global SI-DI is an easy to measure parameter that could help in the assessment of obstructive coronary heart disease.
CONCLUSIONS
Global longitudinal strain diastolic index is significantly lower in patients with obstructive CAD and normal or mildly reduced ejection fraction compared with normal subjects. A cut off value lower than 0.5 selects patients with a higher probability of obstructive coro-nary heart disease.
Study limitations
This is a small study. The studied group of patients was selected regardless of the objective presence of ischemia and it was heterogenous group comprising patients with a high suspicion together with patients with already documented CAD. Another limitation was that we measured only longitudinal diastolic index and it is known that transverse and radial diastolic index are modified in CAD. The analysis was performed retrospectively so we had to exclude some segments with poor quality of image. The cut off point was not statistically demonstrated. Finally, we did not analyse SI-DI in relation with localisation and severity of coronary artery lesions.
Conflict of interest: none declared.
References
1. Patrick Collier, Dermot Phelan, Allan Klein. A test in Context: Myo-cardial Strain measured by Speckle Tracking Echocardiography. J Am Coll Cardiol. 2017; 69: 1043-56
2. Tanaka H, Kawai H, Tatsumi K, Kataoka T, Onishi T, Nose T, Mizo-guchi T, Yokoyama M. Relationship between regional and global left ventricular systolic and diastolic function in patients with coronary artery disease assessed by strain rate imaging. Circ J 2007; 71:517-23
3. Liang HY, Cauduro S, pellikka P, Wang J, Urheim S, Yang EH, Rihal C, Belohlavek M, Khandheria B, Miller FA, Abraham TP. Usefulness of two – dimensional speckle strain for evaluation of left ventricular diastolic deformation in patients with coronary artery disease. Am J Cardiol 2006: 98: 1581-6
4. Azvedo Cf, Amado LC, Kraitchman DL, Gerber BL, Osman NF, Rochitte CE, Edvardsen T, Lima JA. Persistent diastolic dysfunction despite complete systolic functional recovery after rperfused acute myocardial infarction demonstrated by tagged magnetic resonance imagimg. Eur Heart J 2004; 25 : 1419-27
5. Ishii K, Suyama T, Imai M, Maenaka M, Yamanaka A, Makino Y, Sei-no Y, Shimada K, Yoshikawa J. Abnormal regional left systolic and diastolic function in patients with coronary artery disease undergo-ing percutaneous coronary intervention: clinical significance of post-ischemic diastolic stunning. J AmColl cardiol. 2009; 54: 1589-97
6. Philip Brainin, Sofie Reumert Biering Sorensen, Rasmus Mogelvang, Peter Sogaard, jan Skov Jensen, Tor Biering- Sorensen. Postsystolic Shortening by Specckle Tracking Echocardiography Is an Indepen-dent Predictor of Cardiovascular Events and Mortality in the Gen-eral Population J AM Heart Assoc. 2018;7: e 008367. DOI: 101161/ JAHA.117008367
7. Koya Ozawa, Nobusada Funabashi, Takeshi Nishi, Masayuki Taka-hara, Hiroyuuki Takaoka, Yoshihide Fujimoto, Yoshio Kobayashi. Determination of quantitative post-systolic strain index threshold, assessed by two- dimensional speckle traking echocardiography for detection of myocardial ischemic segments confirmed on invasive fractional flow reserve. JACC2015; 65: A1214
8. Ishii Katsuhisa, Imai Makoto, SuyamaTamaki, Motoyoshi Maenaka, Takahiro Nagai, Masaki Kawanami, Yutaka Seino. Exercise- induced post-ischemic left ventricular delayed relaxation or diastolic stun-ning: is it a reliable marker in detecting coronary artery disease? J Am Coll Cardiol. 2009; 53: 698-705
9. Mads Ersbøll, Mads J Andersen, nana Valeur, Ulrik Mogensen, Yama Fahri, Jens Thune, Jacob E. Møller, Christian Hassager, Peter Søgaard, Lars Køber. Early diastolic strain rate in relation to systolic and dia-stolic function and prognosis in acute myocardial infarction study: a two-dimensional speckle tracking-study. European Heart Journal 2014;35:648-656
10. K. Ishii, K. Miwa, T. Sakurai. Motoyoshi Maenaka, MD,Takahiro Nagai, MD, Masaki Kawanami, Yutaka Seino. Detection of post-ischemic regional left ventricular delayed outward wall motion or diastolic stunning after exercise-induced ischemia in patients with stable ef-fort angina by using color kinesis J Am Soc Echocardiogr, 21 (2008), pp. 309-314
11. Masahiko Harada , Kyoko Hayashi , Yuichi Takarada , Hironori Hirai 2007 Mar;34(1):29-35. doi: 10.1007/s10396-006-0127-6
12. Lawrence A. Reduto, William J. Wickemeyer, James B Young, Leslie A. Del Ventura, John W. Reid, Donald H. Glaeser, Miguel A Qui-nones, Richard R. Miller. Left Ventricular Diastolic Performance At Rest and During Exercise in Patients With Coronary Artery Disease Assessment with First-pass Radionuclide Angiography. Circulation 63, No. 6, 1981.Downloaded from http://ahajournals.org by on June 1, 2020
13. Koichi Kimura, Katsu Takenada, XiaoFang Pan, Aya Ebihara, Kan-sei Uno, Nobuaki Fukuda, Takahide Kohro, Hiroyuki Morita, Yutaka Yatomi, Ryozo Nagai. Prediction of coronary artery stenosis using strain imaging diastolic index at rest in patients with preserved ejec-tion fraction. Journal of Cardiology (2011) 57, 311-315
14. Shuo-Ju Chiang, Masao Daimon, Katsuhisa Ishii, Takayuki Kawata, Sakiko Miyazaki, Kuniaki Hirose, Ryoko Ichikawa, Katsumi Miyauchi, Mei-Hsiu Yeh, Nen-Chung Chang, Hiroyuki Daida. Assesment of El-evation of and Rapid Change in left Ventricular Filing Pressure Using a Novel Global Strain Imaging Diastolic Index . Circulation Journal 2014;78 :419-427
15. Shuo-Ju Chiang, Masao Daimon, Katsuhisa Ishii, Sakiko Miyazaki, Yoko Koiso, Hiromasa Suzuki, Katsumi Miyauchi, Bei Yang, Mei-Hsiu Yeh, Betau Hwang, Hiroyuki Daida. A novel global strain diastolic in-dex correlates with plasma NT-proBNP levels in asymptomatic hy-pertensive patients with preserved ventricular ejection fraction. J. echocardiogr.(2009);DOI 10.1007/s12574-012-0122-4
16. Roberto M. Lang, Luigi P. Badano, Victor Mor-Avi, Jonathan Afilalo, Anderson Armstrong, Laura Ernande, Frank A. Flachskampf, Elyse Foster, Steven A. Goldstein, Tatiana Kuznetsova, Patrizio Lancellot-ti, Denisa Muraru, Michael H. Picard, Ernst R. Rietzschel, Lawrence Rudski, Kirk T. Spencer,Wendy Tsang, and Jens-Uwe Voigt. Recom-mendations for Cardiac Chamber Quantification by Echocardiography in Adults: An Update from the American Society of Echocar-diography and the European Association of Cardiovascular Imaging. European Heart Journal – Cardiovascular Imaging (2015) 16, 233–271 doi:10.1093/ehjci/jev014
17. Sherif F. Nagueh, Otto A. Smiseth, Christopher P. Appleton, Ben-jamin F. Byrd,Hisham Dokainish, Thor Edvardsen, Frank A. Flachs-kampf, Thierry C. Gillebert, Allan L. Klein, Patrizio Lancellotti, Paolo Marino, Jae K. Oh, Bogdan Alexandru Popescu, and Alan D. Wag-goner. Recommendations for the Evaluation of Left Ventricular Dia-stolic Function by Echocardiography : An Update from the American Society of Echocardiography and the European Association of Car-diovascular Imaging. European Heart Journal- Cardiovascular Imag-ing( 2016 ) 17, 1321-60
18. Voigt J, Pedrizzetti G, Marwick T et al; Definition for a common standard for 2 D speckle tracking echocardiography: consensus doc-ument of the EACVI /ASE/ Industry Task Force to standardize defor-mation imaging European Heart Journal (2015); 16, 1-11
19. Juhani Knuuti, William Wijns, Antti Saraste Davide Capodanno, Emanuele Barbato, Christian Funck-Brentano, Eva Prescott, Robert F. Storey, Christi Deaton, Thomas Cuisset, Stefan Agewall, Kenneth Dickstein, Thor Edvardsen, Javier Escaned, Bernard J. Gersh, Pavel Svitil, Martine Gilard, David Hasdai, Robert Hatala, Felix Mahfoud, Josep Masip, Claudio Muneretto, Marco Valgimigli, Stephan Achen-bach, Jeroen J. Bax . 2019 ESC Guidelines for the diagnosis and man-agement of chronic coronary syndromes. European Heart Journal (2019) 00, 171 doi:10.1093/eurheartj/ehz425
20. Bonow RO, Vitale DF, Bacharach SL, FrederickTM, Kent KM, Green MV. Adynchronous left ventricular regional function and impaired global diastolic filling in patients with coronary artery disease :rever-sal after coronary angioplasty. Circulation 1985;71:297-307
21. Wijns W, Serruys PW, Slager CJ. Effect of coronary occlusion during percutaneous transluminal angioplasty in humans on left ventricular chamber stiffness and regional diastolic pressure -radius relations. J Am Coll Cardiol1986; 7: 455-63
22. Mor-Avi V, Collins KA, Kocarz CE Shah M, Spencer KT, Lang RM. Detection of regional temporal abnormalities in left ventricular func-tion during acute myocardial ischemia. Am J PhysiolHeart Circ Physi-ol 2001;280: H1770-81
23. Neizel M, Korosoglou G, lossnitzer D, Kuhl H, Hoffmann R, Ock-lenburg C, Giannitsis E, Ossman NF, Katus HA, Steen H. Impact of systolic and diastolic deformation indexes assessed by strain -en-coded imaging to predict persistent severe myocardial dysfunction in patients after acute myocardial infarction at follow-up. J Am Coll Cardiol 2010;56:1056-62.
 This work is licensed under a
This work is licensed under a