Stefan Mot1, Adela Serban1,2, Dana Pop2,3
1 „N. Stăncioiu” Heart Institute, Cluj-Napoca, Romania
2 „Iuliu Hatieganu” University of Medicine and Pharmacy, Cluj-Napoca, Romania
3 Rehabilitation Hospital, Cluj-Napoca, Romania
Abstract: Recent progresses in techniques and knowledge of percutaneous interventions had changed the paradigm of myocardial revascularization in LMCA disease from a surgical procedure 20 years ago to a percutaneous approach for al-most all patients nowadays. There are still pro’s and con’s for each situation and it is clearly the aim of the Heart Team to establish an adequate medical indication with respect to the clinical data, the particularities of the patient, the local surgical or PCI expertise and the preference of the patient and family. This review is trying to present the actual status of evidence – based data in the field of LMCA disease PCI.
Keywords: percutaneous coronary interventions, left main.
The left main coronary artery (LMCA) stenosis is associated with a severe prognosis because of several anatomical and functional particularities of this artery: it is a large, often tapered vessel, arising directly from the aorta, which nourishes a large amount of possi-ble endangered myocardium that can lead to increa-sed risk of major cardiac events1. The vast majority of causes of this narrowing is atherosclerosis, involving in more than 80% of cases the bifurcation of the left main artery, in a „T” shaped angulation of the emer-ging vessels: the left anterior descending (LAD) and circumflex (CX) arteries; in 10% of cases there is also a third vessel – the intermediate ramus- making a so called “trifurcation” and also in 15% of patients becau-se the right coronary artery (RCA) is small, the LMCA is dominant supplying almost the whole left ventricle2. Treatment for that disease is rarely only medical, because of its poor outcome. Coronary artery bypass grafting (CABG) has been for a long time the stan-dard revascularization technique, demonstrating a better survival rate than optimal medical treatment3. Recently published data, comparing revascularization with percutaneous coronary interventions (PCI) ver-sus CABG for LMCA disease had shown comparable results in terms of survival rate, stroke or myocardial infarction4.
A successful interventional treatment of LMCA disea-se implies 2 cardinal rules:
- Careful patient selection
- Proper angioplasty technique including the use of intravascular imaging and physiological guidance This review will emphasize how to do a careful selection of the patients for each strategy of treatment, according to the particular individual clinical aspects, and also the current data supporting different types of PCI techniques and adjunctive imagistic and physiolo-gic intracoronary evaluation modalities.
I. PATIENT SELECTION: PCI VS. CABG IN LMCA DISEASE
Randomized trials: Six randomized trials had com-pared percutaneous revascularization with surgery: LEMANS- 20085; SYNTAX LM- 20106; BOUDRIOT-20117; PRECOMBAT- 20118; EXCEL- 20172 and NO-BLE-20179. Only the last 2 had used second generati-on stents, which are currently available in worldwide cath-labs. The EXCEL trial demonstrated that, in case of low or intermediateanatomical group (Syntax score lower than 32), there is an equipoise of number of deaths, strokes and myocardial infarctions (MIs) at 3 years follow up between the surgical and the inter-ventional groups. However, in long term, there is an excess of need of repeat revascularizations procedu-res in the PCI group. Still, at 30 days PCI had fewer number of deaths, strokes, or MIs and also fewer major arrhythmias, infections, reoperations, bleeding, and transfusions compared with CABG. The investiga-tors of EXCEL stated that PCI should be the preferred strategy of revascularization in carefully selected pa-tients, after discussion in Heart Team10. The NOBLE trial showed a slight superiority of the evolution of patients treated with CABG compared to PCI, mainly driven by the excess of myocardial infarctions and re-peat revascularizations. It is noteworthy that definiti-on of periprocedural MI was different in the two trials – EXCEL has taken into account only those which are clinically significant (10x the upper limit of CK-MB), while NOBLE counted also those which do not in-tervene in the clinical outcome of a patient and also is important to note that in the NOBLE trial a lower quality of DES was used leading to a 3% incidence of stent thrombosis9,11.
Meta-analyses of CABG vs. PCI: A recent me-ta-analysis of the six randomized trials has shown a reduced number of deaths, strokes and myocardial in-farctions, also a reduced number of deaths in the PCI group when the Syntax score is low and increasing with the rise of anatomical complexity12. In another meta-analysis, published in 2018, involving all 11 trials performed until now, comparing PCI with CABG for LMCA disease, Head et al. demonstrated a similar rate of death at 5 years follow up – 10.5%, regardless the presence of diabetes mellitus or high anatomical com-plexity -Syntax score >3313 (Figure 1).
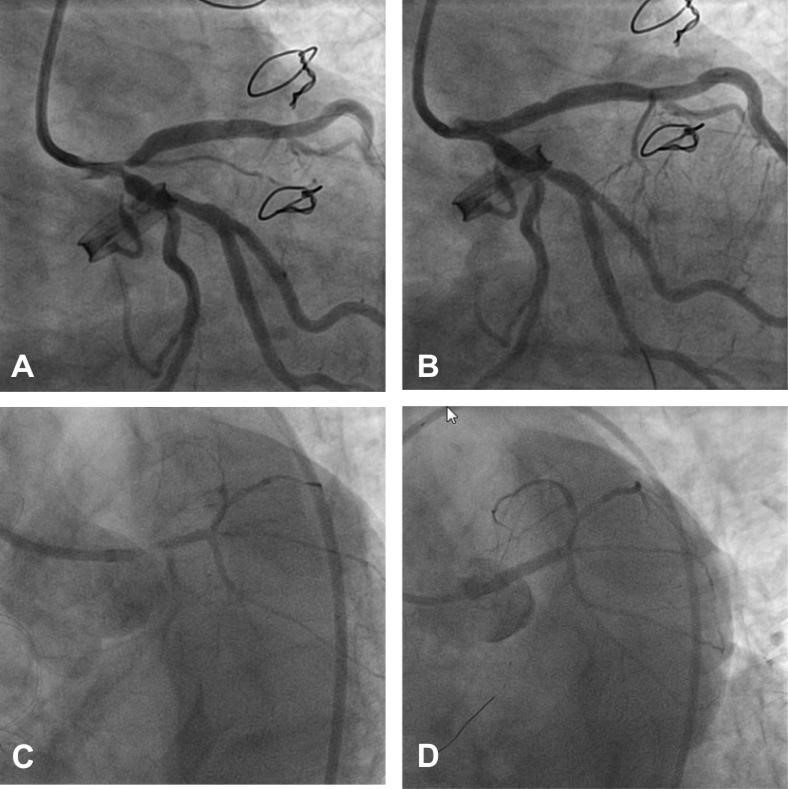
Figure 1. 5 years equipoise of mortality with PCI vs CABG, irrespective to the Syntax score complexity: Syntax score 32: before PCI (A) and after PCI (B); Syntax score 15: before PCI (C) and after PCI (D).
Registries of Left Main Revascularization: FU WAI14, IRIS MAIN15 and DELTA 216 compared pati-ents who were revascularized either with PCI or with CABG between 2004-2015. The results are very si-milar to those observed in the EXCEL trial, with the same number of deaths, strokes and myocardial in-farctions and with an excess number of repeated revascularization procedures in the PCI arm in a median of 3 years follow up.
Meta-analysis of medical treatment compared to PCI: A statistical comparison between the out-come of patients medically treated with those who underwent PCI showed a similar result with surgery, with a reduction of mortality in the PCI group at 5 years with 80%17. With such a significant difference, it is very unlikely that someone could recommend only medical treatment for LMCA disease!
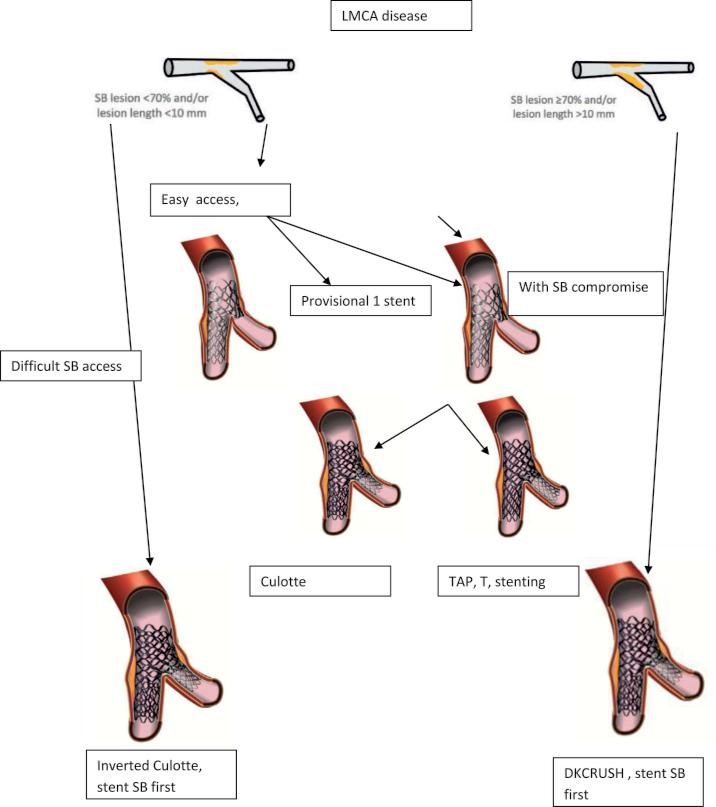
Figure 2. Algorithm for strategy choices of LMCA PCI (adapted from EBC consensus document).
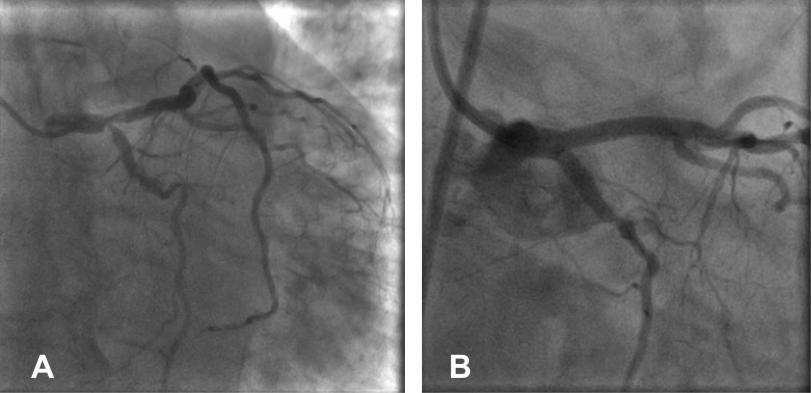
Figure 3. Distal LMCA lesion (Medina 1-1-1) treated with 2 stents with a „dkcrush” technique – before (Figure 3a) and after stenting (Figure 3b).
Thus, PCI is recommended for patients with low and intermediate scores, or to those with high surgical risk and CABG when there is a high anatomical and clinical complexity.
Choosing the indication and risk stratification: After the publication in early 2018 of Head meta-analysis, the newly appeared ESC Guidelines for Myo-cardial Revascularization, stipulated a Class I indication with level of evidence B for PCI in LMCA disease with low Syntax score and II a with the same level of evi-dence for intermediate risk. Since there is no differen-ce in mortality at 5 years, a clinical score was added to the anatomical Syntax score, helping the physician in predicting mortality at 4 years: the Syntax 2 score which integrates 7 variables: age, sex, chronic obstruc-tive pulmonary disease, peripheral vessel disease, left ventricular ejection fraction, creatinine clearance, pre-sence of LMCA disease18. However, the Syntax score 2 was not extensively investigated for LMCA disease. Remarcably the patients with diabetes mellitus (DM) treated with PCI for LMCA disease have similar pro-gnosis as those treated with CABG; on contrary for the 3 vessel coronary artery disease diabetic patients, the classical situation is still valid – surgery is a better option in term of survival13,18. In conclusion for the diabetic patient with left main disease interventional therapy is as good as surgical one!
II. IMPROVEMENTS IN THE TECHNIQUE AND INTRAVASCULAR IMAGING AND PHYSIOLOGICAL GUIDANCE
PCI technique-related issues: PCI for LMCA di-sease should be performed by experienced operators, with at least15 procedures/year for at least 3 consecu-tive years19. The ostial and mid shaft located LMCA lesions are usually straight forward procedures, with a very good long term success. The distal localization is present in 80% of cases and is a bifurcation or trifurca-tion lesion. The current recommendation of the Euro-pean Bifurcation Club is the use of a single stent with the provisional second bail out stenting of the side branch in case of necessity. All single stent procedures should include the Proximal Optimization Techniques (POT), i.e. inflation of large non-compliant balloons inside the stented LMCA20. In certain cases (Figure 2) long CX lesions, high risk of CX compromise or di-fficult access, a double stent strategy should be used from the very beginning. There are several bifurcati-on/2 stents techniques and it is clear that any operator should choose the one which is most convenient for him and suitable for the patient that particular situati-on. There are data coming from two Chinese studies that show that the „double kissing crush” technique is superior to the „cullotte” technique in the treatment of LMCA stenosis and should be the elective proce-dure in such cases21. For any 2 stents procedure, a final POT and a kissing balloon in the LMCA/LAD/CX should be performed.
Stent selection: There was no difference in ischemic end points seen in three prospective registries involv-ing various second-generation DES for LMCA disease. Stent thrombosis was observed in only 0.7% of pati-ents and it is similar to that from the EXCEL Trial, so there should be no recommendation for a specific type of 2nd or 3rd generation of DES, if sizing and te-chniques of implantation are appropriate22. There are ongoing trials studying dedicated bifurcation stents (POLBOS, TRYTON) or biodegradable polymer DES (MAIN COMPARE).
Imaging adjunctive guidance: It is highly impor-tant to have alternative intravascular imaging tools when dealing with LMCA disease PCI, because ob-servational studies had shown a better survival with the use of IVUS in elective cases23. It is important that before intervention the vessel size and distribution of the plaque within the LMCA and its branches to be carefully observed. The measurement of minimal lumen area (MLA) can defer an intervention, if is >6 mm2 24 or recommend it, if is <4.5 mm2, for ostial or shaft LMCA25. After stent implantation, IVUS is a valu-able tool for the evaluation of complications (dissecti-ons, stent distortion), for assessing the apposition of the stent to the vessel wall and also in ensuring the adequate expansion of the stent at different levels of the LMCA: ostial CX- 5 mm2, ostial LAD- 6 mm2, the polygon of confl uence (the convergence zone of the LMCA, LAD, and CX – 7 mm2 and the shaft of the LMCA) – 8 mm2 26. Optical coherence tomography (OCT) is an alternative for IVUS, with a certain limit in defining the ostium of the LM due to the need of deep intubation of the guiding catheter for an adequa-te contrast injection27.
Physiologic adjunctive guidance: FFR or iFRis useful in the preoperative assessment, because, in bor-derline lesions, in almost 30-40% of cases a mismatch between the angiographically defined severity and the functional severity of the myocardial ischemia defined by a FFR <0.75 is observed, due the dimensions of the LMCA28. Post implantation of the stent, FFR can be used for defining the severity of the jailed ostial LAD or CX lesions or for the assessment or other distal non LMCA lesions.
CONCLUSIONS
For most of the patients with left main disease, the survival is similar with interventional or surgical treat-ment.
Clinical decision making on percutaneous revascu-larization for left main coronary artery disease should account for the presence of comorbidities, the extent of the anatomical disease, physiological component, likelihood for complete revascularization, and patient preference.
Physiological assessment should be performed to assess the need for revascularization in bifurcation lesions. Intravascular imaging guidance can be use be-fore the procedure to better understand bifurcation anatomy and to optimize stent implantation; however, clinical outcomes trials are required to recommend imaging as essential part of LMCA PCI.
Bifurcation PCI should be tailored to the patient-specific anatomy and the technique selected based on the experience of the operator. Long lesions in side branch probably benefit from more complex (or 2 stent) techniques.
A collaborative effort combining individual patient datasets from randomized clinical trials has the poten-tial to better identify which patients can benefit from which specific technique.
Conflict of interest: none declared.
References
1. Almudarra SS, Gale CP, Baxter PD, Fleming SJ, Brogan RA, Ludman PF, de Belder MA, Curzen NP; National Institute for Cardiovascular Outcomes Research (NICOR). Comparative outcomes after unpro-tected left main stem percutaneous coronary intervention. JACC Cardiovasc Interv 2014;7:717–730.
2. Stone GW, Sabik JF, Serruys PW, Simonton CA, Ge´ne´reux P, Pus-kas J, Kandzari DE, Morice M-C, Lembo N, Brown WM, Taggart DP, Banning A, Merkely B, Horkay F, Boonstra PW, van Boven AJ, Ungi I, Boga´ts G, Mansour S, Noiseux N, Sabate´ M, Pomar J, Hickey M, Gershlick A, Buszman P, Bochenek A, Schampaert E, Page´ P, Dressler O, Kosmidou I, Mehran R, Pocock SJ, Kappetein AP; EX-CEL Trial Investigators. Everolimus-eluting stents or bypass surgery for left main coronary artery disease. N Engl J Med 2016;375:2223– 2235.
3. Yusuf S, Zucker D, Passamani E, Peduzzi P, Takaro T, Fisher LD, Kennedy JW, Davis K, Killip T, Norris R, Morris C, Mathur V, Var-nauskas E, Chalmers TC. Effect of coronary artery bypass graft sur-gery on survival: overview of 10-year results from randomised trials by the Coronary Artery Bypass Graft Surgery Trialists Collabora-tion. Lancet 1994;344:563–570.
4. Morice M-C, Serruys PW, Kappetein AP, Feldman TE, Stahle E, Co-lombo A, Mack MJ, Holmes DR, Torracca L, van Es G-A, Leadley K, Dawkins KD, Mohr F. Outcomes in patients with de novo left main disease treated with either percutaneous coronary interven-tion using paclitaxel-eluting stents or coronary artery bypass graft treatment in the synergy between percutaneous coronary interven-tion with TAXUS and Cardiac Surgery (SYNTAX) Trial. Circulation 2010;121:2645–2653.
5. Buszman PE, Buszman PP, Banasiewicz-Szkro´bka I, Milewski KP, Z_ urakowski A, Orlik B, Konkolewska M, Trela B, Janas A, Martin JL, Kiesz RS, Bochenek A. Left main stenting in comparison with surgical revascularization: 10-year outcomes of the (Left Main Coronary Ar-tery Stenting) LE MANS Trial. JACC Cardiovasc Interv 2016;9:318– 327
6. Morice M-C, Serruys PW, Kappetein AP, Feldman TE, Stahle E, Co-lombo A, Mack MJ, Holmes DR, Choi JW, Ruzyllo W, Religa G, Huang J, Roy K, Dawkins KD, Mohr F. Five-year outcomes in pa-tients with left main disease treated with either percutaneous coro-nary intervention or coronary artery bypass grafting in the synergy between percutaneous coronary intervention with taxus and cardiac surgery trial. Circulation 2014;129:2388–2394
7. Boudriot E, Thiele H, Walther T, Liebetrau C, Boeckstegers P, Pohl T, Reichart B, Mudra H, Beier F, Gansera B, Neumann F-J, Gick M, Zietak T, Desch S, Schuler G, Mohr F-W. Randomized comparison of percutaneous coronary intervention with sirolimus-eluting stents versus coronary artery bypass grafting in unprotected left main stem stenosis. J Am Coll Cardiol 2011;57:538–545.
8. Park S-J, Kim Y-H, Park D-W, Yun S-C, Ahn J-M, Song HG, Lee J-Y, Kim W-J, Kang S-J, Lee S-W, Lee CW, Park S-W, Chung C-H, Lee J-W, Lim D-S, Rha S-W, Lee S-G, Gwon H-C, Kim H-S, Chae I-H, Jang Y, Jeong M-H, Tahk S-J, Seung KB. Randomized trial of stents versus bypass surgery for left main coronary artery disease. N Engl J Med 2011;364:1718–1727
9. Ma¨kikallio T, Holm NR, Lindsay M, Spence MS, Erglis A, Menown IBA, Trovik T, Eskola M, Romppanen H, Kellerth T, Ravkilde J, Jen-sen LO, Kalinauskas G, Linder RBA, Pentikainen M, Hervold A, Banning A, Zaman A, Cotton J, Eriksen E, Margus S, Sørensen HT, Nielsen PH, Niemela¨ M, Kervinen K, Lassen JF, Maeng M, Oldroyd K, Berg G, Walsh SJ, Hanratty CG, Kumsars I, Stradins P, Steigen TK, Fro¨bert O, Graham ANJ, Endresen PC, Corbascio M, Kajander O, Trivedi U, Hartikainen J, Anttila V, Hildick-Smith D, Thuesen L, Christiansen EH; NOBLE Study Investigators. Percutaneous coro-nary angioplasty versus coronary artery bypass grafting in treat-ment of unprotected left main stenosis (NOBLE): a prospective, randomised, open-label, non-inferiority trial. Lancet 2016;388:2743– 2752
10. Baron SJ, Chinnakondepalli K, Magnuson EA, Kandzari DE, Puskas JD, Ben-Yehuda O, Es G-A, van Taggart DP, Morice M-C, Lembo NJ, Brown WM, Banning A, Simonton CA, Kappetein AP, Sabik JF, Ser-ruys PW, Stone GW, Cohen DJ; EXCEL Investigators. Quality of life after everolimus-eluting stents or bypass surge
11. Capodanno D, Bass TA. Revascularization of unprotected left main coronary artery disease. Circ Cardiovasc Interv 2016;9:e004782.
12. Palmerini T, Serruys P, Kappetein AP, Genereux P, Riva D Della, Reggiani LB, Christiansen E, Holm NR, Thuesen L, Makikallio T, Morice MC, Ahn J-M, Park S-J, Thiele H, Boudriot E, Sabatino M, Romanello M, Biondi-Zoccai G, Cavalcante R, Sabik JF, Stone GW. Clinical outcomes with percutaneous coronary revascularization vs coronary artery bypass grafting surgery in patients with unprotected left main coronary artery disease: a meta-analysis of 6 randomized trials and 4,686 patients. Am Heart J 2017;190:54–63.
13. Head SJ, Milojevic M, Daemen J, Ahn J-M, Boersma E, Christiansen EH, Domanski MJ, Farkouh ME, Flather M, Fuster V, Hlatky MA, Holm NR, Hueb WA, Kamalesh M, Kim Y-H, Ma¨kikallio T, Mohr FW, Papageorgiou G, Park S-J, Rodriguez AE, Sabik JF, Stables RH, Stone GW, Serruys PW, Kappetein AP. Mortality after coronary ar-tery bypass grafting versus percutaneous coronary intervention with stenting for coronary artery disease: a pooled analysis of individual patient data. Lancet 2018;391:939–948.
14. Zheng Z, Xu B, Zhang H, Guan C, Xian Y, Zhao Y, Fan H, Yang Y, Wang W, Gao R, Hu S. Coronary artery bypass graft surgery and percutaneous coronary interventions in patients with unpro-tected left main coronary artery disease. JACC Cardiovasc Interv 2016;9:1102–1111.
15. Lee PH, Ahn J-M, Chang M, Baek S, Yoon S-H, Kang S-J, Lee S-W, Kim Y-H, Lee CW, Park S-W, Park D-W, Park S-J. Left main coro-nary artery disease: secular trends in patient characteristics, treat-ments, and outcomes. J Am Coll Cardiol 2016;68:1233–1246.
16. Chieffo A, Tanaka A, Giustino G, Briede I, Sawaya FJ, Daemen J, Kawamoto H, Meliga E, D’Ascenzo F, Cerrato E, Stefanini GG, Cap-odanno D, Mangiameli A, Templin C, Erglis A, Morice MC, Mehran R, Van Mieghem NM, Nakamura S, De Benedictis M, Pavani M, Var-bella F, Pisaniello M, Sharma SK, Tamburino C, Tchetche D, Colom-bo A; DELTA 2 Investigators. The DELTA 2 registry. JACC Cardio-vasc Interv 2017;10:2401–2410
17. Shah R, Morsy MS, Weiman DS, Vetrovec GW. Meta-analysis com-paring coronary artery bypass grafting to drug-eluting stents and to medical therapy alone for left main coronary artery disease. Am J Cardiol 2017;120:63–68
18. Farooq V, van Klaveren D, Steyerberg EW, Meliga E, Vergouwe Y, Chieffo A, Kappetein AP, Colombo A, Holmes DR, Mack M, Feld-man T, Morice M-C, Sta°hle E, Onuma Y, Morel M, Garcia-Garcia HM, van Es GA, Dawkins KD, Mohr FW, Serruys PW. Anatomical and clinical characteristics to guide decision making between cor-onary artery bypass surgery and percutaneous coronary interven-tion for individual patients: development and validation of SYNTAX score II. Lancet 2013;381:639–650.
19. Xu B, Redfors B, Yang Y, Qiao S, Wu Y, Chen J, Liu H, Chen J, Xu L, Zhao Y, Guan C, Gao R, Ge´ne´reux P. Impact of operator experience and volume on outcomes after left main coronary ar-tery percutaneous coronary intervention. JACC Cardiovasc Interv 2016;9:2086–2093.
20. Lassen JF, Burzotta F, Banning AP, Lefe`vre T, Darremont O, Hil-dick-Smith D, Chieffo A, Pan M, Holm NR, Louvard Y, Stankovic G. Percutaneous coronary intervention for the Left Main stem and other bifurcation lesions. The 12(th) consensus document from the European Bifurcation Club. EuroIntervention 2018;13:1540–1553
21. Chen S-L, Xu B, Han Y-L, Sheiban I, Zhang J-J, Ye F, Kwan TW, Paiboon C, Zhou Y-J, Lv S-Z, Dangas GD, Xu Y-W, Wen S-Y, Hong L, Zhang R-Y, Wang H-C, Jiang T-M, Wang Y, Sansoto T, Chen F, Yuan Z-Y, Li W-M, Leon MB. Clinical outcome after DK crush ver-sus culotte stenting of distal left main bifurcation lesions: the 3-year follow-up results of the DKCRUSH-III Study. JACC Cardiovasc In-terv 2015;8:1335–1342.
22. Lee PH, Kwon O, Ahn J-M, Lee CH, Kang D-Y, Lee J-B, Kang S-J, Lee S-W, Kim Y-H, Lee CW, Park S-W, Park D-W, Park S-J. Safe-ty and effectiveness of second generation drug-eluting stents in pa-tients with left main coronary artery disease. J Am Coll Cardiol 2018;71:832–841.
23. Park S-J, Kim Y-H, Park D-W, Lee S-W, Kim W-J, Suh J, Yun S-C, Lee CW, Hong M-K, Lee J-H, Park S-W; MAIN-COMPARE Inves-tigators. Impact of intravascular ultrasound guidance on long-term mortality in stenting for unprotected left main coronary artery ste-nosis. Circ Cardiovasc Interv 2009;2:167–177
24. de la Torre Hernandez JM, Herna´ndez Hernandez F, Alfonso F, Ru-moroso JR, Lopez-Palop R, Sadaba M, Carrillo P, Rondan J, Lozano I, Ruiz Nodar JM, Baz JA, Fernandez Nofrerias E, Pajin F, Garcia Camarero T, Gutierrez H; LITRO Study Group (Spanish Working Group on Interventional Cardiology). Prospective application of pre-defined intravascular ultrasound criteria for assessment of interme-diate left main coronary artery lesions results from the multicenter LITRO study. J Am Coll Cardiol 2011;58:351–358
25. Park S-J, Ahn J-M, Kang S-J, Yoon S-H, Koo B-K, Lee J-Y, Kim W-J, Park D-W, Lee S-W, Kim Y-H, Lee CW, Park S-W. Intravascular ultrasound-derived minimal lumen area criteria for functionally sig-nifi cant left main coronary artery stenosis. JACC Cardiovasc Interv 2014;7:868–874
26. Kang S-J, Ahn J-M, Song H, Kim W-J, Lee J-Y, Park D-W, Yun S-C, Lee S-W, Kim Y-H, Lee CW, Mintz GS, Park S-W, Park S-J. Com-prehensive intravascular ultrasound assessment of stent area and its impact on restenosis and adverse cardiac events in 403 patients with unprotected left main disease. Circ Cardiovasc Interv 2011;4:562– 569.
27. Burzotta F, Dato I, Trani C, Pirozzolo G, De Maria GL, Porto I, Nic-coli G, Leone AM, Schiavoni G, Crea F. Frequency domain optical coherence tomography to assess non-ostial left main coronary ar-tery. EuroIntervention 2015;10:e1–e8.
28. Hamilos M, Muller O, Cuisset T, Ntalianis A, Chlouverakis G, Sar-no G, Nelis O, Bartunek J, Vanderheyden M, Wyffels E, Barbato E, Heyndrickx GR, Wijns W, De Bruyne B. Long-term clinical outcome after fractional fl ow reserve-guided treatment in patients with angio-graphically equivocal left main coronary artery stenosis. Circulation 2009;120:1505–1512.
29. Puri R, Kapadia SR, Nicholls SJ, Harvey JE, Kataoka Y, Tuzcu EM. Op-timizing outcomes during left main percutaneous coronary interven-tion with intravascular ultrasound and fractional fl ow reserve. JACC Cardiovasc Interv 2012;5:697–707.
 This work is licensed under a
This work is licensed under a