Catalina Lionte1,3, Cristina Bologa1,3, Ovidiu Petris1,3, Victorita Sorodoc1,3, Alexandra Stoica1,3, Cristina Tuchilus2,3, Elisabeta Jaba4, Adorata Elena Coman1,3, Luminita Vata1,3, Raluca Haliga1,3, Oana Sirbu1,3, Laurentiu Sorodoc1,3
1 2nd Medical Clinic, „Sf. Spiridon” Emergency Clinical County Hospital, Iasi, Romania
2 Central Laboratory, „Sf. Spiridon” Emergency Clinical County Hospital, Iasi, Romania
3 „Grigore T. Popa” University of Medicine and Pharmacy, Iasi, Romania
4 Department of Statistics, FEAA, „Al. I. Cuza” University, Iasi, Romania
Abstract: Acute poisonings represent a challenge for the hospital practitioners, the burden of morbidity and mortality being significant worldwide. The prognostic utility of combined analysis using troponin I (TnI), electrocardiogram (ECG), and transthoracic echocardiography (TTE) parameters in acute poisoning, upon admission in a medical or intensive care unit (ICU) ward, was not evaluated. This prospective observational cohort studied 222 acutely poisoned adults with an in-hospital mortality rate of 4.5%. Multivariate logistic regression showed, as predictors for in-hospital mortality, TnI measured 6 hours from admission [odds ratio (OR) 1.752; CI 95%: 1.201-2.558; p 0.004], the QTc interval (OR 1.882; CI 95%: 1.022-3.466; p 0.043), and deceleration time (DT) of the E wave (OR 3.653; CI 95%:1.460-9.137; p 0.006). The receiver operating characteristic (ROC) analysis confi rmed that 6h-troponin (AUC, 0.889; CI, 0.789-0.990; p < 0.001), and DT (AUC, 0.801; CI, 0.644-0.958; p 0.001), have the capacity to indicate a risk for in-hospital mortality. Among the parameters infl uencing in-hospital mortality of acutely poisoned patients, myocardial injury assessed upon admission based on the dynamic of cardiac troponins, ECG and TTE can be used to predict the outcome and mortality in this setting. Keywords: poisoning, myocardial injury, in-hospital mortality.
INTRODUCTION
Acute poisonings have a high morbidity and morta-lity and represent an important challenge for hospital practitioners1,2. Myocardial injury frequently occurs af-ter exposure to different poisons, such as pharmaceu-tical agents with a recognized cardiotoxicity3,4, carbon monoxide (CO)5 and other toxic gases, pesticides6, drugs of abuse7,8, or vegetal toxins9,10, and it was pro-ved to be a predictor of mortality in several toxin ex-posures.3,5,11 There are studies which investigated the potential role of biomarkers12,13, transthoracic echo-cardiography (TTE)14, or both15, in some toxin expo-sures, especially those related with a high cardiovas-cular morbidity. Electrocardiogram (ECG) parameters have a predictive role for the outcome and mortality in patients suspected of acute poisoning.16 Our previo-us experience showed the benefi t of using some clini-cal scores, lactate, B-type natriuretic peptide, and MB isoenzyme of creatine kinase to early predict the com-plications, poor short-term outcomes, and mortality in systemic poison exposures17, and the usefulness of E-wave deceleration time (DT) and B-type natriuretic peptide to predict mortality in patients acutely into-xicated with undifferentiated poisons18. However, the combined analysis of troponin I with ECG and TTE parameters upon admission of an acutely poisoned pa-tient in a medical or Intensive Care Unit (ICU) ward, with respect to the outcomes and in-hospital morta-lity, was not performed.
The aim of this study was to analyze if myocardial injury, assessed using troponin I (TnI) measured upon admission and 6 hours after presentation, ECG, as well as the parameters of cardiac function using TTE in a cohort with acute poisoning hospitalized in a medical or ICU ward can be useful as an early predictor for a poor outcome and in-hospital mortality in acutely poi-soned patients with different xenobiotics. Thus, the practitioners could optimize the strategies to identify the poisoned patients with acute myocardial injury and adjust their management to improve the outcome of these patients.
MATERIALS AND METHODS
We performed a prospective observational study in a cohort of patients acutely poisoned with different xe-nobiotics, over a period of 18 months (October 2016 – March 2018). We enrolled consecutive patients ol-der than 18 years, which were addressed to the Emer-gency Department (ED) within 12 hours from poison exposure and admitted in a medical or ICU ward with a diagnosis of acute poisoning, after obtaining an in-formed consent. The study was partially funded by an internal research grant of the university, approved by the review board of the hospital and university.
Patients had either an accidental acute exposure, or a self-poisoning with pharmaceutical agents (prescrip-tion drugs and over-the-counter [OTC] medicines), illicit drugs, nonpharmaceutical agents (i.e. pesticides, rodenticides, chemicals, toxic alcohols), vegetal to-xins, toxic gases, or a combination of multiple poisons. Patients without a signed informed consent, younger than 18 years of age, with an associated disease that can influence biomarkers, ECG or TTE pattern (i.e. diabetes, acute myocardial infarction or heart failure, chronic renal disease, severe liver disease), patients with an acute pathology associated to poisoning (i.e. trauma, burns, anaphylaxis etc.), or patients with in-complete data were excluded from our study.
Poisoning severity score (PSS) was determined in all patients using the grading system described by Pers-son et al.19 The venous blood was collected immedia-tely after admission for conventional laboratory tests and troponin I (TnI) analysis, 6 hours after the admissi-on for TnI (6h-troponin), also during the hospital stay at the discretion of the attending physician, to assess acute myocardial injury, according to the European Society of Cardiology guidelines20. Cardiovascular bi-omarkers were determined from the blood sample with PATHFAST® Cardiac Biomarker Analyser (LSI Medience Corporation, Japan), and with ARCHITECT c16000 clinical chemistry analyser (Abbott Labora-tories, USA). A standard 12-lead ECG was recorded upon ED presentation using a CardioM Medica ECO-Net 12 channels electrocardiograph and repeated during hospitalization when needed. The QTc was cal-culated using the Bazett formula21 and was considered prolonged if greater than 440 milliseconds (ms).
We performed immediately after admission a stan-dard TTE in all poisoned patients, using a Fukuda Denshi Full Digital Ultrasound System UF-850XTD (Fukuda Denshi Co., Ltd., Japan). The parameters’ normal values were considered upon guidelines’ re-commendations22,23.
We observed as an outcome measure the status at hospital discharge. A poor outcome was defi ned as multiple complications or in-hospital death. Patients with a myocardial injury detected during hospitalization were programmed for a follow-up thirty days post-discharge, but unfortunately not all patients were compliant with this recommendation.
Statistical analysis
The categorical variables were expressed as numbers and percentages and compared using the Chi-squa-re test. The continuous variables were expressed as medians with interquartile ranges (IQR) and compa-red with the Mann-Whitney test. The variables were compared in univariate analysis (survivors vs decea-sed patients). All significant variables in the univariate analyses for in-hospital mortality were subjected to a multivariate logistic regression analysis. Risk was ex-pressed as odds-ratios (OR) with confidence inter-vals (CI). Goodness-of-fit for multivariate models was confirmed using the Hosmer and Lemeshow test. The receiver operating characteristic (ROC) methodology was used to analyze the discriminatory capacity of predictive variables. ROC analyses were expressed as curve plots and calculated area under the curve (AUC) with 95% CI and the associated p value representing the likelihood of the null hypothesis (AUC = 0.5). P values <0.05 were considered statistically significant. Statistical analyses were performed using SPSS softwa-re for Windows (V.22.0; SPSS, Chicago, IL, USA).
RESULTS
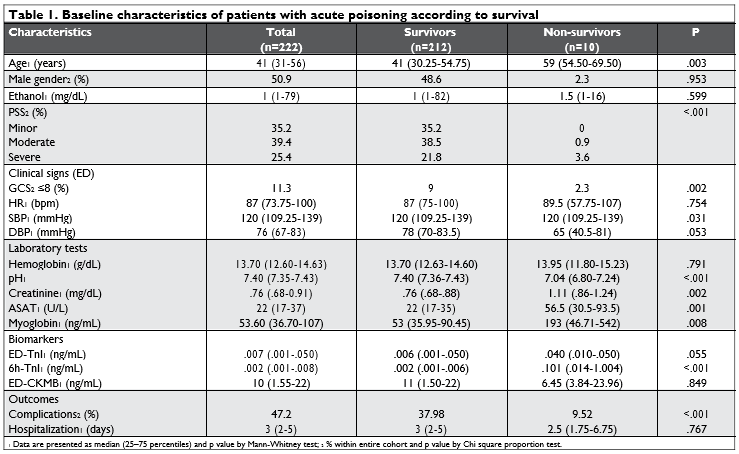
We analyzed 222 patients, with a median age of 43 years (range 18-91 years), 50.9% men. Time to ED arrival was 4.2 ± 1.8 hours (range 30 minutes-12 hours). The selected clinical characteristics (demographics, PSS, GCS, poison types, vital signs, etc.) with respect to mortality are included in Table 1, and Figure 1.
43 patients in our cohort were exposed to com-binations of poisons (15.5%), 40 were exposed to non-pharmaceutical agents (14.4%), 33 patients were poisoned with sedative-hypnotics (11.9%), 31 cases were exposed to pesticides (11.2%), 16 patients to antidepressant/ antipsychotic medication (5.8%).
There were 15 patients exposed to toxic gases, ma-inly carbon monoxide (5.4%), and 11 patients with cardiovascular drugs poisoning (4%). The rest of the cases were poisoning with OTC medication, or other prescription drugs (Figure 1), and only 4 patients had vegetal toxins exposure (1.4%). There were no signifi-cant differences in the outcomes based on the poison involved. Ethanol co-ingestion had no influence on the outcome or death.
Although there was a significant statistical differen-ce in the age, PSS, GCS score of survivors versus non-survivors, these variables did not predict in-hospital mortality after multivariate logistic regression.
169 patients of the entire cohort (76.2%) developed complications, while 35 patients had multiple compli-cations, involving at least two major organs or systems, and cardiovascular complications were recorded in 15.76 % patients. Patients with a poor outcome didn’t have a significantly prolonged hospitalization (Table 1). Deaths were recorded in 10 patients (4.5%) in our cohort, as follows: 4 patients (1.8%) intoxicated with combinations of poisons, 3 patients exposed to toxic alcohols and chemicals (1.4%), one pesticide exposure, one toxic gas exposure, and one patient poisoned with antidepressants. The direct cause of death was represented by multiple complications (dysrhythmi-as, toxic-induced myocardial injury, refractory shock, acute respiratory distress syndrome, and multiple or-gan failure).
There was no significant statistical difference in TnI level within age and gender groups, while the mean initial levels of TnI were higher in non-survivor group (Table 1) but didn’t reach the statistical significance (p 0.55). Assessment of 6h-TnI showed a signifi cantly higher value in the fatalities group (Table 1).
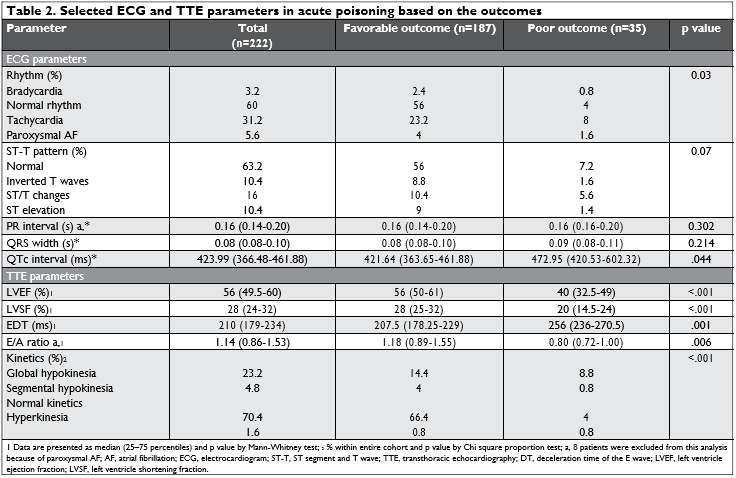
When analyzing ECG, 40% subjects had an abnormal rhythm, while ST – T changes were seen in 36.8% pa-tients and were predictive for a poor outcome (Table 2). There were no significant differences in PR inter-val, QRS complex width within the outcome groups, however the QTc interval was significantly prolonged in patients with the poor outcome (Table 2). There were no significant differences in the ECG parameters among poison groups.
At the time of the TTE, 8 subjects (3.6%) were in atrial fibrillation (Table 2). Alteration in both diastolic and systolic LV function, along with presence of LV regional or global wall abnormalities had a signifi cant impact on the outcome (Table 2).
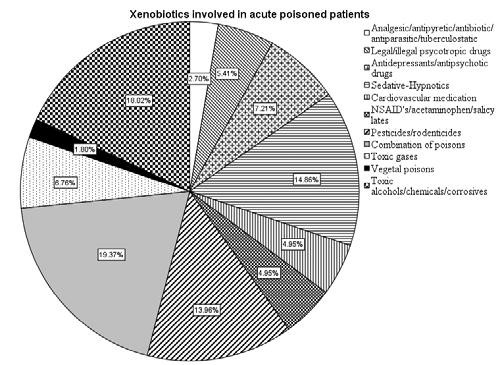
Figure 1. Xenobiotics involved in acute poisoning in cohort studied.
Logistic regression analysis
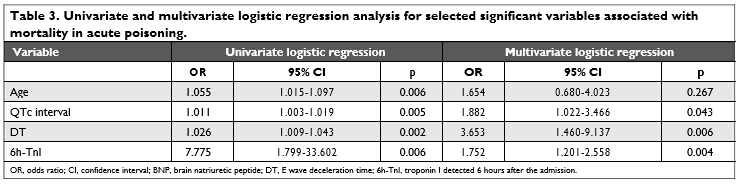
After univariate logistic regression analysis, age, the QTc interval, DT and 6h-TnI correlated with in-hos-pital mortality (Table 3). The multivariate logistic re-gression analysis including the same predictor varia-bles showed that only the QTc interval (OR 1.882; CI 95%: 1.022-3.466; p 0.043), DT (OR 3.653; CI 95%:1.460-9.137; p 0.006) and 6h-TnI (OR 1.752; CI 95%: 1.201-2.558; p 0.004) are predictive for morta-lity in acute poisoning with different xenobiotics. The ROC analysis demonstrated two predictive variables to have a good discriminatory power for mortality (Fi-gure 2).
DISCUSSION
This is the first study, to our knowledge, which pro-spectively and concomitantly correlates the TnI levels upon arrival and 6 hours after admission in a medical or ICU ward with ECG parameters and TTE indices in a heterogeneous cohort of acutely poisoned patients admitted to a medical or ICU ward within 12 hours
of poison exposure. Despite a relatively small number of fatalities (10 patients, 4.5%), we observed a strong relationship between TnI dynamic, and alteration in LV function evaluated using TTE with the risk of a poor outcome and death.
ECG changes were analyzed in different poison ex-posures3,5,13,24,25. Some studies demonstrated a corre-lation between the prolonged QT interval with cardi-ovascular events in patients with drug self-poisoning26, and with mortality, in herbicide poisoning11. A QTc interval greater than 500 ms was predictive for cardi-otoxicity in antipsychotic overdose27 and, along with QT interval dispersion, was proved to be an indepen-dent predictor of adverse cardiovascular events in a heterogeneous cohort of 34 patients with suspected poisoning involving different types of drugs, alcohols, and herbal/OTC medication16, also for cardiovascular complications in acute poisoning with cardiotoxic me-dication or poisons3. However, in methanol poisoning, abnormalities on the ECG suggestive for cardiotoxi-city failed to predict mortality25. Our results based on a larger cohort of poisoned patients, with acute expo-sure to heterogeneous xenobiotics, showed that the prolonged QTc interval >472 ms is correlated with a poor outcome and increases by 88% the odds of in-hospital mortality. This observation is important, be-cause in our cohort, the proportion of agents proved to determine QTc prolongation and subsequent death (i.e. cardiovascular drugs, antidepressants, antipsycho-tics, pesticides) was 26.2%, the rest being poisons that were not associated until now with QTc interval pro-longation-induced mortality. Also, it is consistent with our previous results on patients acutely poisoned with a systemic toxin17.
TnI is a biomarker with increased levels in pesticide poisoning13,28, and a negative TnI on admission exclu-des fatality with an extremely high predictive value in undifferentiated patients with acute drug overdose12. Our results showed that in acute poisoning with heterogeneous toxins, initial elevated TnI, but mainly elevation of 6-h TnI as a consequence of acute myo-cardial injury, is a biomarker predictive for a poor outcome and shows a 74% increased risk for in-ho-spital mortality in this setting. This is an interesting observation, mainly because we tried to include in our study patients without the comorbidities which could be associated with an increased troponin level29.
The possible mechanisms involved in acute poi-soning complicated with myocardial injury might be the imbalance between the oxygen supply (decreased in CO exposure, after coronary vasospasm or toxin induced dysrhythmias or hypotension) and increased myocardial oxygen demands (in febrile patients such as neuroleptic poisoning, hypertension occurring in stimulants acute poisoning etc.), or as a consequence of direct myocardial cell death after inhibition of oxi-dative phosphorylation12,30,31.
Echocardiography showed a better accuracy, as opposed to ECG changes, in detecting CO-induced cardiac damage, where changes in diastolic function, preceding systolic function abnormalities32, or various patterns of LV systolic dysfunction were observed32-34. Our previous experience with TTE in acute poisoned non-diabetic patients proved that assessment of dias-tolic function correlated with BNP level are useful to predict mortality18.
The results obtained in this cohort of acutely poi-soned patients showed that the assessment, using TTE upon admission in a medical or ICU ward, of cardiac function parameters, especially the diastolic function of the LV, accurately predicted the risk for a poor outcome and death in this setting, showing 2.65 times increased odds of mortality. We hypothesize that a prolonged DT may reflect the poison-induced subcli-nical heart damage, or the setting of acute myocar-dial injury, being recognized that diastolic dysfuncti-on is a feature that precedes systolic dysfunction32,33. Although several changes in systolic function were observed in the analyzed cohort, they failed to signi-ficantly correlate with in-hospital mortality, possibly because of a relatively low prevalence of recognized cardiotoxins in our cohort.
To the best of our knowledge, this is the largest study to prospectively demonstrate the utility of tro-ponin, combined with ECG and TTE parameters as markers of acute myocardial injury to predict, upon admission in a medical or ICU ward, the risk of a poor outcome and in-hospital death for acutely poisoned patients with different xenobiotics.
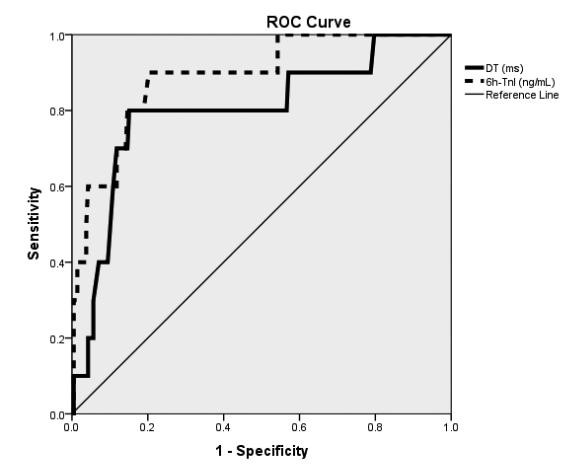
Figure 2. Receiver Operating Characteristic Curves validates the dis-criminatory power of the parameters predicting mortality. Areas under the curves: DT (E wave deceleration time): 0.801 (95% confidence interval 0.644-0.958, p 0.001); 6h-TnI (troponin detected 6 hours after admission): 0.889 (95 % confi dence interval 0.789-0.990, p<0.001).
Limitations
The main limitation of the study may be that too few patients died during hospitalization to deliver reliable statistical data about in-hospital mortality. A larger sample was not available for this analysis given the constraints applied from the exclusion criteria, to avoid bias from co-morbidities in the cardiovascular biomarkers, ECG and echocardiography analysis. We could not calibrate the influence of toxin serum con-centration, and we could not monitor all patients at least 30 days after the acute poisoning. Future pro-spective studies are warranted to confirm and further explore the implications of toxin-induced acute myo-cardial injury in every patient admitted with an acute poisoning in a medical or ICU ward.
CONCLUSIONS
In acutely poisoned adult patients, assessment of myo-cardial injury using initial and 6h-TnI, the QTc interval on initial ECG and the parameters of LV diastolic func-tion obtained using TTE upon admission in a medical or ICU ward accurately predicted the outcomes and mortality. As TnI, ECG, and TTE are routinely used and not expensive, are less invasive, and are widely available, they can be successfully applied in everyday practice as part of the initial evaluation of acutely poi-soned patients with different xenobiotics, to assess their outcomes. They may help hospital practitioners to improve the management of these poisonings and to early address the worst outcome and mortality.
Funding: This study was partially funded by the “Gr. T. Popa” University of Medicine and Pharmacy Iasi, Romania (grant No. 30884/30.12.2014).
Conflict of interest: none declared.
References
1. Dart RC, Bronstein AC, Spyker DA, Cantilena LR, Seifert SA, Heard SE, Krenzelok EP. Poisoning in the United States: 2012 Emergency Medicine Report of the National Poison Data System. Ann Emerg Med 2015; 65: 416-22.
2. Krakowiak A, Kotwica M, Śliwkiewicz K, Piekarska-Wijatkowska A. Epidemiology of acute poisonings during 2003–2007 in Toxicology Unit, Department of Occupational Medicine and Toxicology, Nofer Institute of Occupational Medicine, Łódź, Poland. IJOMEH 2011; 24: 199-207.
3. Hassanian-Moghaddam H, Amiri H, Zamani N, Rahimi M, Shadnia S, Taherkhani M. QT Dispersion and Prognostication of the Outcome in Acute Cardiotoxicities: A Comparison with SAPS II and APACHE II Scoring Systems. Cardiovasc Toxicol 2014; 14: 129-33.
4. Berling I, Isbister GK. Prolonged QT Risk Assessment in Antipsy-chotic Overdose Using the QT Nomogram. Ann Emerg Med 2015; 66: 154-64.
5. Kao HK, Lien TC, Kou YR, Wang JH. Assessment of myocardial in-jury in the emergency department independently predicts the short-term poor outcome in patients with severe carbon monoxide poisoning receiving mechanical ventilation and hyperbaric oxygen ther-apy. Pulm Pharmacol Ther 2009; 22: 473-7.
6. Roth A, Zellinger I, Arad M, Atsmon J. Organophosphates and the Heart. Chest 1993; 103: 576-82.
7. Lusetti M, Licata M, Silingardi E, Bonetti LR, Palmiere C. Therapeu-tic and recreational methadone cardiotoxicity. J Forensic Leg Med 2016; 39: 80-4.
8. Schwartz BG, Rezkalla S, Kloner RA. Cardiovascular Effects of Co-caine. Circulation 2010; 122: 2558-69.
9. Tovar RT, Petzel RM. Herbal Toxicity. Dis Mon 2009; 55: 592-641.
10. Unverir P, Soner BC, Dedeoglu E, Karcioglu O, Boztok K, Tuncok Y. Renal and hepatic injury with elevated cardiac enzymes in Amanita phalloides poisoning: a case report. Hum Exp Toxicol 2007; 26: 757-61.
11. Kim YH, Lee JH, Hong CK, Cho KW, Park YH, Kim YW, Hwang SY. Heart rate–corrected QT interval predicts mortality in glyphosate-surfactant herbicide–poisoned patients. Am J Emerg Med 2014; 32: 203-7.
12. Manini AF, Stimmel B, Hoffman RS, Vlahov D. Utility of Cardiac Troponin to Predict Drug Overdose Mortality. Cardiovasc Toxicol 2016; 16: 355-60.
13. Cha YS, Kim H, Go J, Kim TH, Kim OH, Cha KC, Lee KH, Hwang SO. Features of myocardial injury in severe organophosphate poi-soning. Clin Toxicol 2014; 52: 873-9.
14. Jung Y, Lee J, Min Y, Park J, Jeon W, Park E, Shin J, Oh S, Choi SC. Carbon Monoxide-Induced Cardiomyopathy. Circ J 2014; 78: 1437-44.
15. Liu S, Shen Q, Lv C, Zhang P, Yu H, Yang L, Wu L. Analysis of com-bined detection of N terminal pro–B-type natriuretic peptide and left ventricular ejection fraction in heart function in patients with acute CO poisoning. Am J Emerg Med 2014; 32: 1212-4.
16. Manini AF, Nelson LS, Skolnick AH, Slater W, Hoffman RS. Electro-cardiographic Predictors of Adverse Cardiovascular Events in Sus-pected Poisoning. J Med. Toxicol 2010; 6: 106-15.
17. Lionte C, Sorodoc V, Tuchilus C, Cimpoiesu D, Jaba E. Biomarkers, lactate, and clinical scores as outcome predictors in systemic poi-sons exposures Hum Exp Toxicol. 2017; 36: 651-62.
18. Lionte C, Sorodoc V, Bologa C, Tuchilus C, Jaba E. Usefulness of Transthoracic Echocardiography Parameters and Brain Natriuretic Peptide as Mortality Predictors in Hospitalized Acutely Poisoned Patients: A Prospective Observational Study. Basic Clin Pharmacol Toxicol 2017; 120: 498-504.
19. Persson HE, Sjöberg GK, Haines JA, Pronczuk de Garbino J. Poison-ing Severity Score: Grading of acute poisoning. J Toxicol – Clin Toxi-col 1998; 36: 205-13.
20. Thygesen K, Alpert JS, Jaffe AS, Chaitman BR, Bax JJ, Morrow DA, White HD: the Executive Group on behalf of the Joint European So-ciety of Cardiology (ESC)/American College of Cardiology (ACC)/ American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarc-tion. Fourth universal defi nition of myocardial infarction. Circulation. 2018; 138: e1–e34. DOI: 10.1161/CIR.0000000000000617.
21. Chan A, Isbister GK, Kirkpatrick CMJ, Dufful SB. Drug induced QT prolongation and torsade de pointes: evaluation of a QT nomogram. QJM 2007; 100: 609-15.
22. Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, Flachskampf FA, Foster E, Goldstein SA, Kuznetsova T, Lancellotti P, Muraru D, Picard MH, Rietzschel ER, Rudski L, Spencer KT, Tsang W, Voigt JU. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascu-lar Imaging. J Am Soc Echocardiogr 2015; 28:1-39.
23. Lancellotti P, Price S, Edvardsen T, Cosyns B, Neskovic AN, Dulghe-ru R, Flachskampf FA, Hassager C, Pasquet A, Gargani L, Galderisi M, Cardim N, Haugaa KH, Ancion A, Zamorano JL, Donal E, Bueno H, Habib G. The use of echocardiography in acute cardiovascular care: Recommendations of the European Association of Cardiovascular Imaging and the Acute Cardiovascular Care Association. Eur Heart J – Cardiovasc Imaging 2015; 16: 119-46.
24. Akdur O, Durukan P, Ozkan S, Avsarogullari L, Vardar A, Kavalci C, Ikizceli I. Poisoning severity score, Glasgow coma scale, corrected QT interval in acute organophosphate poisoning. Hum Exp Toxicol 2010; 29: 419-25.
25. Sanaei-Zadeh H, Emamhadp M, Farajidana H, Zamanp N, Amirfar-hangp A. Electrocardiographic manifestations in acute methanol poi-soning cannot predict mortality. Arh Hig Rada Toksikol 2013; 64: 265-71.
26. Maignan M, Pommier P, Clot S, Saviuc P, Debaty G, Briot R, Car-pentier F, Danel V. Deliberate Drug Poisoning with Slight Symptoms on Admission: Are there Predictive Factors for Intensive Care Unit Referral? A three-year Retrospective Study. Basic Clin Pharmacol Toxicol 2014; 114: 281-7.
27. Khalaf MAM, Abdel Rahman TM, Abbas MF. Values of Using QTc and N-Terminal Fragment of B-Type Natriuretic Peptide as Markers for Early Detection of Acute Antipsychotic Drugs-Induced Cardiotoxicity. Cardiovasc Toxicol 2011; 11:10-7.
28. Lee DK, Cho NH, Kim OH, Go J, Kim TH, Cha KC, Kim H, Lee KH, Hwang SO, Cha YS. Evaluation of Cardiac Function Using Transtho-racic Echocardiography in Patients with Myocardial Injury Secondary to Methomyl Poisoning. Cardiovasc Toxicol 2015; 15: 269-75.
29. Petris AO, Tatu-Chitoiu G, Coman IM, Tint D, Christodorescu R, Chioncel V, Darabantiu D, Cimpoesu D, Antohi L, Sorodoc L, Pe-trescu L, Pop C, Mebazaa A, Chioncel O. Biomarkers in emergen-cy cardiology: cardio-pulmonary resuscitation, acute coronary syn-dromes, pulmonary thromboembolism, acute aortic syndrome and acute heart failure. Romanian Journal of Cardiology 2017; 27: 333-48.
30. Lionte C, Sorodoc L, Petriş O, Sorodoc V. Electrocardiographic changes in acute organophosphate poisoning. Rev Med Chir Soc Med Nat Iasi. 2007; 111: 906-11.
31. Lionte C. An unusual cause of hypotension and abnormal electrocar-diogram (ECG) — scombroid poisoning. Central European Journal of Medicine 2010; 5: 292-7.
32. Çiftçi Ö, Günday M, Çaliskan M, Güllü H, Dogan R, Güven A, Müder-risoglu H. Mild carbon monoxide poisoning impairs left ventricular diastolic function. Indian J Crit Care Med 2013; 17: 148-53.
33. Davutoglu V, Gunay N, Kocoglu H, Gunay NE, Yildirim C, Cavdar M, Tarakcioglu M. Serum Levels of NT-ProBNP as an Early Cardiac Marker of Carbon Monoxide Poisoning. Inhal Toxicol 2006; 18:155-8.
34. Park JS, Seo KW, Choi BJ, Choi SY, Yoon MH, Hwang GS, Tahk SJ, Choi SC, Min YG, Shin JH. Various Echocardiographic Patterns of Left Ventricular Systolic Dysfunction Induced by Carbon Monoxide Intoxication. Cardiovasc Toxicol 2016; 16:361-9.
 This work is licensed under a
This work is licensed under a