Download PDF
https://doi.org/10.47803/rjc.2020.30.4.620
Cosmin Cojocaru1, Mohamed Dardari1, Dan-Andrei Radu1,2, Stefan Bogdan1,2, Corneliu Iorgulescu1,2, Radu Vatasescu1,2
1 Laboratory of Clinical Electrophysiology and Pacing, Department of Cardiology, Clinical Emergency Hospital, Bucharest, Romania
2 „Carol Davila” University of Medicine and Pharmacy, Bucharest, Romania
Abstract: Aims – Frequent premature ventricular complexes (PVCs) may induce/aggravate LV systolic dysfunction (LVD) by tachy(dyssynchrono)cardiomyopathy (tCMP) in patients with/without previous structural heart disease. High arrhythmic burden (i.e. >26%) is the main predictor of tCMP development in patients with previously normal LV function. However, its predictive power is reduced once the arrhythmic burden is below 26%, with considerable overlap between patients at risk for tCMP and those who will maintain normal LV function. We sought to evaluate the predictive power of a composite index that includes PVC burden, PVC duration and PVC coupling interval. Methods – 61 patients referred for radiofrequency ablation (RFA), with frequent PVCs refractory to at least one antiarrhythmic drug (AAD), symptomatic and/ or with LV systolic dysfunction (LVEF < 50%) were retrospectively studied. Patients with structural lesions on transthoracic echocardiography (TTE) and/or cardiac magnetic resonance imaging (c-MRI), with sustained ventricular tachycardia/supra-ventricular tachycardia or severe valvular disease were excluded. A composite parameter dependent on PVC burden, PVC duration and PVC coupling interval was defined. Results – Mean PVC burden was 25.80% ± 11.64 (35% ± 8.16 in tCMP subgroup). Chronic PVC suppression was achieved in 89.6% of patients with a mean of 1.44 ± 0.7 procedures with 86.4% of patients requiring one procedure. Septal right ventricular outflow tract (RVOT) was the most frequent PVC origin (36.1%). Mean left ventricular ejection fraction (LVEF) in the tCMP group (7 patients) was 38% ± 5.26 which increased 1 month after RF ablation to 54.6% ± 3.64 (87.35% of recovered LVEF), at 3 months to 56% ± 2.23 and at 6 months 57% ± 2.73. LVEF recovery was also present in non-tCMP subgroup, yet statistically insignificant. There was no procedure-related mortality. Retrograde ventriculo-atrial (VA) conduction, male gender, non-sustained VT (NSVT), a higher BMI and a higher PVC burden were associated with tCMP development. ROC curve analysis appears to demonstrate higher sensitivity of tCMP prediction by the composite index in comparison to PVC burden in patients with 16.93-25.93% PVCs (i.e. below the formerly described tCMP PVC% cut-off). Conclusions – In patients with a PVC burden lower than the previously described cut-offs (i.e. with ~17-25% PVCs) PVC mediated systolic dysfunction seems to be predicted with higher sensitivity by a composite index accounting for PVC burden, PVC duration and PVC coupling interval.
Keywords: Premature ventricular complexes, cardiomyopathy, ventricular dysfunction, catheter ablation, arrhythmic burden, heart failure.
WHAT’S NEW
Considerable overlap between patients with premature ventricular complexes (PVCs) that are at risk for tachycardiomyopathy and those who will maintain normal LV function below the threshold of 26% PVCs. In patients with PVC burden lower than the previously described thresholds, PVC mediated systolic dysfunction seems to be predicted with higher sensitivity by simultaneously accounting for PVC burden, PVC duration and PVC coupling interval.
INTRODUCTION
Premature ventricular complexes (PVCs) are frequently encountered in both structurally normal and diseased hearts and high arrhythmic burden is known to induce or aggravate or induce left ventricular dysfunction (LVD). Even though it is regarded as the cardinal predictor of tachycardiomyopathy (tCMP), PVC burden is however an imperfect predictor as there are both patients with high arrhythmic burden with no LVD development and severe LVD can be encountered with relatively low burdens of PVCs (i.e. there is important variability of the critical burden for LVD in individual patients). Consequently, multiple trials have evaluated further tCMP risk factors in addition to PVC percentage (such as broad QRS PVCs, long coupling interval, epicardial origin, lack of circadian variability of PVCs, retrograde conduction, male gender, time from diagnosis, asymptomatic PVCs). We decided to evaluate a composite index that includes PVC QRS duration and PVC coupling in addition to PVC burden.
METHODS
Symptomatic and/or tCMP patients with frequent (> 10%) idiopathic PVCs refractory to at least one anti-arrhythmic drug referred for radiofrequency ablation (RFA) were retrospectively included. A PVC tCMP subgroup was defined by LVEF < 50%. Patients with structural heart disease (SHD) demonstrated by transthoracic echocardiography (TTE) were excluded. C-MRI was used for SHD exclusion in 60.7% of patients. Patient demographics, clinical data, previous antiarrhythmic treatments, baseline & PVC electrical characteristics, TTE & Holter EKG data, PVC anatomical origin and intraprocedural fluoroscopy and mapping data, at initial referral and by follow-up at 1, 3 and 6 months post-RFA. RFA was performed by manual ablation or aided by remote magnetic navigation system (MNS, Stereotaxis Inc., Niobe II). Activation mapping +/- electro-anatomical mapping (CARTO3, Biosense Webster, Diamond Bar, CA, USA) were used to locate PVC origin. Acute procedural success was defined as the elimination of the targeted PVCs and lack of recurrence 30 minutes after the last RF application. Chronic procedural success was defined by at least 80% reduction in PVC burden at 6 months evaluation. A composite index was defined as the natural logarithm (ln) of the burden of PVC multiplied by the coupling interval and by PVC duration – Index = ln (PVC_burden x coupling_interval x PVC_duration). Statistical analysis was performed using IBM SPSS Statistics 20.0 (IBM Corporation, Armonk, NY, USA). Discrete variables were compared using Chi-square analysis. Continuous variables were expressed as mean ± standard deviation (SD) and were compared using 2-group Student T test/paired student T test. Receiver-operator curve analysis was performed to compare sensitivity and specificity for PVC burden and the composite index. A p value < 0.05 was considered statistically significant.
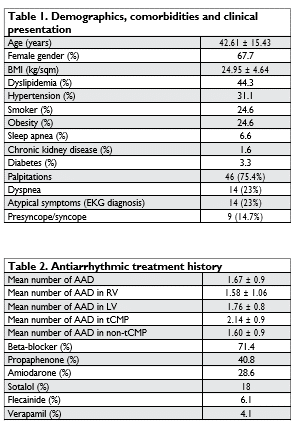
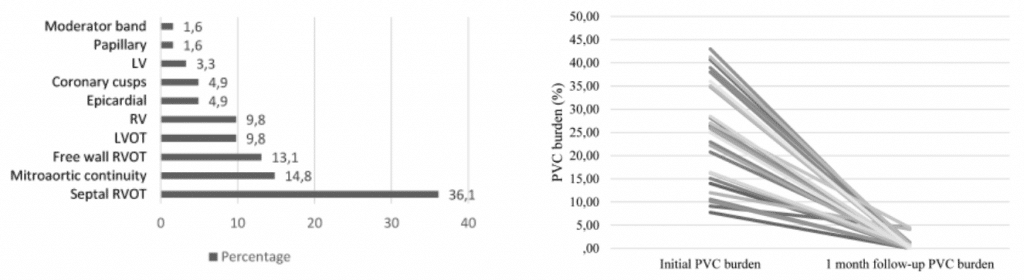
Figure 1. PVCs origin sites.
Figure 2. PVC burden evolution at 1 month follow-up post-radiofrequency ablation.
RESULTS
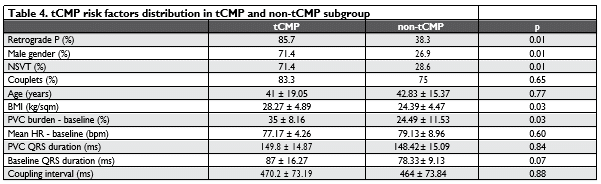
Baseline characteristics of the patient populations. 61 patients with idiopathic PVCs were included with a mean age of 42.61 ± 15.43 years, 67.7% female gender. Beta-blockers were most frequently used by physicians as AADs and most patients had tried >1 AAD before ablation referral. In patients with LV originating PVCs and in those with tCMP respectively, a greater number of AADs was used as compared with those with RV PVC origin and those without tCMP, yet statistically insignificant. Palpitations were the most frequent symptom (Tables 1, 2).
Procedural results. Chronic procedural success was obtained in 89.6% of patients with 1.44 ± 0.7 pro-cedures. Septal RVOT was most frequently targeted (36.1%) and required 1 procedure in 86.4% of cases. Rarest origins targeted (1 case each) were the posteromedial papillary muscle and the moderator band but required multiple procedures (5 and 3 respectively). There was no procedure related mortality.
Post-procedural evolution. In patients with chronic procedural success, RF ablation lead to a statistically significant reduction of PVC burden (< 0.7% PVCs) during the follow-up interval. The mean average heart rate of patients with acute procedural success was subsequently reduced throughout the follow-up interval (1 month – 77.05 ± 7.5 bpm, statistically different from baseline average HR – p = 0.03; 3 months 64 ± 6.36, not statistically different compared to 1 month average HR – p = 0.1; 6 months – 74.30 ± 7.90, statistically different from 3 month average HR – p = 0.001) in comparison to the initial value (80.76 ± 8.33), with lack of statistical significance at 3 months. In tCMP patients, systolic function recovery (as expressed by LVEF) was most important (i.e. 87.35% of entire recovery) during the first month post-ablation by reaching 54.6 ± 3.64% from 38 ± 5.26% (p = 0.009) and continued over the entire monitoring period at 3 months (56 ± 2.23%, p = 0.003) and 6 months (57.85 ± 2.73%, p = 0.004). Baseline LVEF in non-tCMP patients was 56.93 ± 3.87%; LVEF recovery was encountered (1 month – 58.07 ± 2.33%, p = 0.11; 3 months – 58.44 65%, p = 0.09, 6 months 57.85 ± 2.66%, p = 0.09), yet statistically insignificant.
Retrospective analysis of tCMP risk factors. Retrograde VA conduction, male gender, NSVT were significantly more frequent in tCMP when compared to non-tCMP subgroup; BMI and PVC burden were statistically higher in tCMP patients. However, there was no statistical difference in PVC QRS duration, baseline QRS duration, average heart rate (HR) or age and no particular PVC origin predicted tCMP. Receiver-operator characteristic curve analysis demonstrated higher sensitivity of tCMP susceptibility based on the composite index (AUC 0.800) in comparison to PVC burden (AUC 0.781) over a certain interval of specificity attributed to patients with 16.95-25.93% PVC burden.
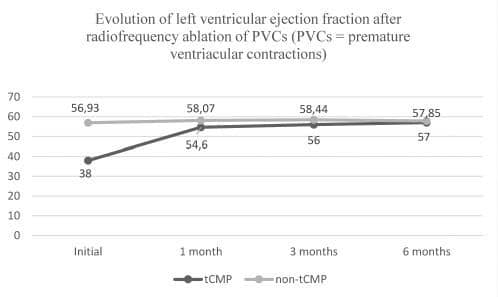
Figure 3. Evolution of left ventricular ejection fraction recovery after radiofrequency ablation in tCMP and non-TCMP subgroups.
DISCUSSIONS
Procedural results and post-ablation evolution. Similarly to data derived from previous clinical trials1-4, chronic success by RFA was obtained in almost 90% of cases and RVOT was the most frequent origin (which usually required one procedure). Mitro-aortic continuity was the most frequent left-sided origin. Complete LVEF recovery after RFA is to be expected in pure tCMP5 (as defined by LVEF <50% with complete reversibility post-RFA) and was mostly noted throughout the first month (some trials even showing LVEF normalization during the first week post-RFA6) and sustained over the 6 months monitoring period. Further follow-up data was not included in the current analysis, but trials show that LVEF recovery is generally limited to the first 6 months post-RFA7,8. Though statistically insignificant, LVEF recovery was also observed in the non-tCMP group (which may be caused by arbitrary definition of LVD solely by < 50% and not by the extent of systolic performance recovery).
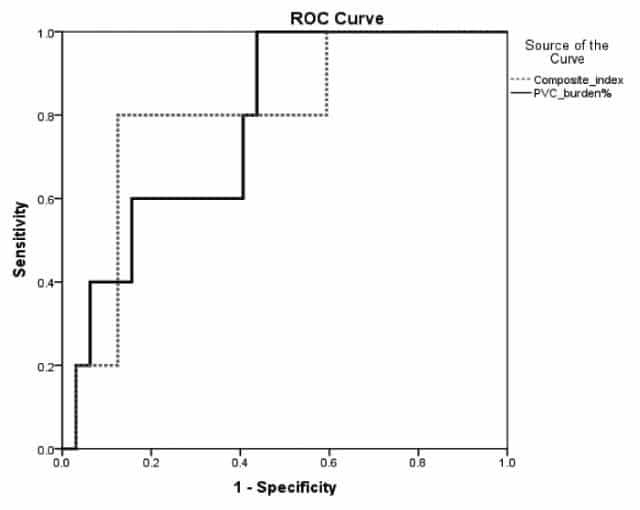
Figure 4. Receiver-operator characteristic curve indicating combination of sensitivity and specificity for tCMP development based on PVC burden and composite index. PVC = premature ventricular complex.
Retrospective analysis of tCMP risk factors Several risk factors for tCMP development previously confirmed in larger trials1,9 were significantly differently distributed or statistically different in tCMP & non-tCMP subgroups (i.e. male gender, NSVT, retro-grade VA conduction; BMI, PVC burden).
Male gender. Male gender has been previously described as an independent predictor of tCMP1; even if population-based trials show that PVCs seem to be more symptomatic in females10 (which may lead to earlier therapy and avoidance of LVD development in time), the neuro-hormonal implications of PVC-tCMP development have not yet been fully understood.
Average heart rate. Two major components are considered to be involved in tCMP5 – tachycardia (i.e. high average heart rates) and dyssynchronous contraction (i.e. larger QRSs) during PVCs. Even though there were no differences between average HR between tCMP and non-tCMP and average HR did not predict tCMP in logistic regression, our data shows significant reduction in average HR 1 month after RFA (referring to tachycardia mediated systolic dysfunction).
Retrograde ventriculoatrial conduction. Retrograde VA conduction is regarded as an independent predictor of tCMP, which was consistent with our data. Long-term atrial retrograde activation causes an abnormal ventriculo-atrial contraction which may induce transient haemodynamic changes which in time can contribute to tCMP development11.
PVC QRS duration. Previous studies show that broader PVCs (>150 msec – i.e. through more pronounced ventricular dyssynchrony) more likely lead to tCMP development even with lower arrhythmic burdens12. However, PVC duration was similar between tCMP and non-tCMP subgroups and did not predict tCMP in logistic regression in our study.
Coupling interval & PVC origin. Long CI of PVCs is considered to be a predictor of tCMP deve-lopment13. LV dyssynchrony seems to be more pronounced at longer CI (and interestingly not in different PVC origins in recent data) which may participate in progressive systolic dysfunction14. Furthermore, the greater preload of longer CI may exaggerate mechanical stretch on the myocardial wall and seems to increase activity in local sensory neurites15 in comparison to short CI. However, our data showed no statistical difference between PVC QRS duration and CI between tCMP and non-tCMP patients.
Arrhythmic burden. Even if current available data shows that PVC-induced cardiomyopathy may be predicted by PVC burdens higher than ~26% (similar to our burden cut-off evaluation by ROC-curve analysis – 25.93%, 80% sensitivity, specificity 62.2%)2,9,11,16,17 clinical and electrophysiologic characteristics, and the predictors of TICMP in patients with idiopathic ventricular arrhythmias. There is great variability of critical PVC burden for LVD development in individual patients. Moreover, recent data shows that subtle LV systolic dysfunction (i.e. decrease in longitudinal strain) may be seen even with 8% PVCs burden18.
Composite index. ROC curve analysis of the composite index including previously discussed tCMP factors (PVC QRS duration, longer CI and high arrhythmic burden) demonstrated higher sensitivity (i.e. detection of LVD-susceptible cases) in patients between 16.95 – 25.93% PVCs (i.e. below the formerly described thresholds of arrhythmic burden for tCMP development) when compared to PVC burden alone.
LIMITATIONS
A limited number of retrospectively included patients were included – however similar to previous clinical trials with a ratio of 1:10 tCMP cases to normal LVEF), which may influence statistical analysis. As in all previous PVC tCMP clinical trials, biased inclusion of non-ultrasound-apparent structurally diseased hearts is possible; in this regard, cardiac MRI evaluation for LGE was performed in more than half of the patients included.
CONCLUSIONS
In patients with ~17-25% PVCs (i.e. below PVC burden-based cut-off of tCMP prediction) patients at risk of tCMP development may be better identified (in comparison to PVC burden alone) by accounting for PVC burden, PVC QRS duration and coupling interval simultaneously.
Conflict of interest: none declared.
References
1. Latchamsetty R, Yokokawa M, Morady F, Kim HM, Mathew S, Tilz R, et al. Multicenter outcomes for catheter ablation of idiopath-ic premature ventricular complexes. JACC Clin Electrophysiol. 2015;1(3):116–23.
2. Hasdemir C, Ulucan C, Yavuzgil O, Yuksel A, Kartal Y, Simsek E, et al. Tachycardia-induced cardiomyopathy in patients with idiopath-ic ventricular arrhythmias: the incidence, clinical and electrophysi-ologic characteristics, and the predictors. J Cardiovasc Electrophysi-ol [Internet]. 2011;22(6):663–8. Available from: http://onlinelibrary. wiley.com/store/10.1111/j.1540-8167.2010.01986.x/asset/j.1540-8167.2010.01986.x.pdf?v=1&t=if5idl3u&s=7b215e6f2b9e1d3e9e383f 318232249b392a1b7f
3. Zhong L, Lee YH, Huang XM, Asirvatham SJ, Shen WK, Friedman PA, et al. Relative efficacy of catheter ablation vs antiarrhythmic drugs in treating premature ventricular contractions: A single-center retrospective study. Hear Rhythm. 2014;11(2):187–93.
4. Wijnmaalen AP, Delgado V, Schalij MJ, van Huls van Taxis CFB, Hol-man ER, Bax JJ, et al. Benefi cial effects of catheter ablation on left ventricular and right ventricular function in patients with frequent premature ventricular contractions and preserved ejection fraction. Heart. 2010;96(16):1275–80.
5. Martin CA, Lambiase PD. Pathophysiology, diagnosis and treatment of tachycardiomyopathy. Heart [Internet]. 2017;103(19):1543– 52. Available from: http://heart.bmj.com/lookup/doi/10.1136/ heartjnl-2016-310391
6. HASDEMIR C, KARTAL Y, SIMSEK E, YAVUZGIL O, AYDIN M, CAN LH. Time Course of Recovery of Left Ventricular Systolic Dysfunction in Patients with Premature Ventricular Contraction-In-duced Cardiomyopathy. Pacing Clin Electrophysiol [Internet]. 2013 May [cited 2016 Aug 24];36(5):612–7. Available from: http://doi.wi-ley.com/10.1111/pace.12087
7. Penela D, Van Huls Vans Taxis C, Aguinaga L, Fern??ndez-Armenta J, Mont L, Castel MA, et al. Neurohormonal, structural, and function-al recovery pattern after premature ventricular complex ablation is independent of structural heart disease status in patients with de-pressed left ventricular ejection fraction: A prospective multicenter study. J Am Coll Cardiol. 2013;62(13):1195–202.
8. Yokokawa M, Good E, Crawford T, Chugh A, Pelosi F, Latcham-setty R, et al. Recovery from left ventricular dysfunction after abla-tion of frequent premature ventricular complexes. Hear Rhythm. 2013;10(2):172–5.
9. DEL CARPIO MUNOZ F, SYED FF, NOHERIA A, CHA Y-M, FRIEDMAN PA, HAMMILL SC, et al. Characteristics of Premature Ventricular Complexes as Correlates of Reduced Left Ventricular Systolic Function: Study of the Burden, Duration, Coupling Interval, Morphology and Site of Origin of PVCs. J Cardiovasc Electrophysiol [Internet]. Blackwell Publishing Inc; 2011 Jul 1;22(7):791–8. Available from: http://dx.doi.org/10.1111/j.1540-8167.2011.02021.x
10. Sirichand S, Killu AM, Padmanabhan D, Hodge DO, Chamberlain AM, Brady PA, et al. Incidence of idiopathic ventricular arrhyth-mias: A population-based study. Circ Arrhythmia Electrophysiol. 2017;10(2).
11. Ban J-E, Park H-C, Park J-S, Nagamoto Y, Choi J-I, Lim H-E, et al. Electrocardiographic and electrophysiological characteristics of pre-mature ventricular complexes associated with left ventricular dys
function in patients without structural heart disease. Europace [In-ternet]. 2013;15(5):735–41. Available from: http://www.ncbi.nlm.nih. gov/pubmed/23194696
12. Yokokawa M, Kim HM, Good E, Crawford T, Chugh A, Pelosi F, et al. Impact of QRS duration of frequent premature ventricular complexes on the development of cardiomyopathy. Hear Rhythm. 2012;9(9):1460–4.
13. Sadron Blaye-Felice M, Hamon D, Sacher F, Pascale P, Rollin A, Du-parc A, et al. Premature ventricular contraction-induced cardiomy-opathy: Related clinical and electrophysiologic parameters. Hear Rhythm. 2016;13(1):103–10.
14. Potfay J, Kaszala K, Tan AY, Sima AP, Gorcsan J, Ellenbogen KA, et al. Abnormal Left Ventricular Mechanics of Ventricular Ectopic Beats: Insights Into Origin and Coupling Interval in Premature Ventricular Contraction-Induced Cardiomyopathy. Circ Arrhythm Electrophysi-ol [Internet]. 2015 Oct [cited 2016 Sep 20];8(5):1194–200. Available from: http://www.ncbi.nlm.nih.gov/pubmed/26297787
15. Hamon D, Rajendran PS, Chui RW, Ajijola OA, Irie T, Talebi R, et al. Premature Ventricular Contraction Coupling Interval Variability De-stabilizes Cardiac Neuronal and Electrophysiological Control. Circ Arrhythmia Electrophysiol. 2017;10(4).
16. Latchamsetty R, Bogun F. Premature Ventricular Complex-induced Cardiomyopathy. Rev Esp Cardiol. 2016;69(4):365–9.
17. Baman TS, Lange DC, Ilg KJ, Gupta SK, Liu T-Y, Alguire C, et al. Re-lationship between burden of premature ventricular complexes and left ventricular function. Hear Rhythm [Internet]. Elsevier; 2010 Jul [cited 2016 Sep 22];7(7):865–9. Available from: http://linkinghub.el-sevier.com/retrieve/pii/S1547527110003280
18. Arnar DO, Mairesse GH, Boriani G, Calkins H, Chin A, Coats A, et al. Management of asymptomatic arrhythmias. Europace [Inter-net]. 2019; Available from: http://www.ncbi.nlm.nih.gov/pubmed/ 30882141.
 This work is licensed under a
This work is licensed under a