Ana-Maria Vintila1,2, Irina Iordachescu1, Mihaela Horumba1
1 Department of Internal Medicine and Cardiology, Coltea Clinical Hospital, Bucharest, Romania
2 Department of Internal Medicine, „Carol Davila” University of Medicine and Pharmacy, Bucharest, Romania
Abstract: Objective – The purpose of our study was to evaluate LDL-cholesterol goal attainment in patients at very high-cardiovascular risk due to concurrent arterial hypertension, type 2 diabetes mellitus and ASCVD, in light of the recently updated dyslipidemia guidelines. Methods – Data from patients enrolled between January 2016 and December 2017 was collected in order to assess LDL cholesterol target attainment (≤70 mg/dL and <55 mg/dL) corresponding to 2016 and 2019 European Dyslipidemia Guidelines. Results – A total of 993 patients were included in the analysis. Only 31% of patients achieved LDL-c goals of ≤70 mg/dL, without gender differences, a percentage which further dropped to 15% after establi-shing the target below 55 mg/dL. Patients with concurrent atrial fibrillation (34.9% vs. 25.1%, p=0.006), heart failure (37.1% vs. 27.2%, p=0.047) and chronic kidney disease (36.3% vs. 28.2%, p=0.028) had better, though far from optimal lipid control per the 2016 guidelines. Two in three patients had controlled diabetes with HbA1c values below 7%. Conclusion – Our study shows that LDL-c targets were not met by very-high risk patients even with the lower 2016 threshold, with the new recommendations making lipid goals look more daunting.
Keywords: arterial hypertension; diabetes; dyslipidemia; LDL-cholesterol goals; very-high cardiovascular risk.
INTRODUCTION
Cardiovascular disease (CVD) is the leading cause of mortality with an estimated 30% of deaths worldwide1. From an economic standpoint, CVD places a heavy burden which could potentially be limited by populati-on-wide interventions, but should also be addressed in a patient-oriented approach, especially in patients who are at high or very-high cardiovascular risk1,2.
The prevalence of arterial hypertension and type 2 diabetes mellitus, keystone factors of CVD, is high and likely to increase further due to „globalization” of dietary habits and urbanization1,3. These conditions potentiate one another in producing atherosclerotic cardiovascular disease (ASCVD) which may lead to stroke, myocardial infarction, chronic kidney disease and ultimately death.
Low-density lipoprotein cholesterol has been attes-ted as a determinant of atherosclerotic cardiovascular disease. Recent studies have shown little risk associa-ted with a drastic LDL-cholesterol decrease4. Accor-ding to the 2019 ESC guidelines for the management of dyslipidemia, diabetic patients at very-high cardio-vascular risk should aim for an LDL-c reduction ≥50% from baseline or an LDL-c goal <55 mg/dL5 irrespecti-ve of primary or secondary prevention; this new goal aims for tighter lipid control than previously recom-mended in the 2016 version (≤70 mg/dL)6. However, real world data has shown time and again that lipid control is achieved in relatively few patients7,8.
MATERIAL AND METHODS
We performed a retrospective, unicentric, cohort study on consecutive patients admitted to the Depart-ment of Internal Medicine and Cardiology between January 2016 and December 2017. All patients were over 18 years of age and signed an informed consent; all had arterial hypertension, diabetes mellitus and AS-CVD diagnosed prior to enrollment. Data regarding demographics (gender, age) was collected along with laboratory assay results including lipid profile (serum cholesterol, triglycerides, LDL-cholesterol, HDL-cho-lesterol), glycated hemoglobin and renal function (se-rum urea, creatinine, uric acid). All patients were un-dergoing statin treatment, though data was not acqui-red as to the specific type or dose.
LDL-c goal attainment categorical variables were created in accordance with the ESC Guideline for the management of dyslipidemias as all patients were considered to be at very-high cardiovascular risk due to association of arterial hypertension, type 2 diabetes mellitus, age (≥40 years for men, ≥50 years for women) and diagnosed ASCVD (in the form of stable angina, prior myocardial infarction or coronary revas-cularization). Thus, treatment targets were LDL-cho-lesterol ≤70 mg/dL and <55 mg/dl, respectively, accor-ding to the 2016 and 2019 editions of the guideline.
Statistical analysis was performed using IBM® SPSS for Windows version 20. Descriptive statistics – means SD and proportions – were used to define patient demographics and lipid profile goal attainment. Computations included the 2 test to compare proporti-ons and analysis of variance to compare differences between continuous variables. A p-value below 0.05 was considered statistically significant.
RESULTS
We enrolled a total of 993 patients with a slight pre-dominance of the female gender (59.9%) and a mean age of 69.2 ± 9.7 years. Women were slightly older than men (70.4 ± 9.6 years vs. 67.3 ± 9.6, p<0.001). Two in three patients had controlled diabetes, with glycated hemoglobin values below the 7% target (Ta-ble 1).
In accordance with the 2016 ESC dyslipidemia tar-gets (LDL-cholesterol ≤70 mg/dL), only about a third of patients had LDL-c levels within the desired range (31.6%, mean LDL-c: 91.7 ± 38.3 mg/dL). Taken furt-her, with the 2019 ESC dyslipidemia targets applied (patients at very-high cardiovascular risk should aim for an LDL-c goal <55 mg/dL), the number of patients dropped by half (15.8%).
Patients who attained lipid goals were slightly older when considering LDL-c target ≤70 mg/dL (70.3 ± 9.3 vs. 68.0 ± 9.9, p=0.004) but not <55 mg/dL (p=0.064). There was no difference between LDL-c values of male or female patients (89.9 ± 38.6 mg/dL vs. 92.8 ± 38.7 mg/dL, p=0.341) and, thus, no gender specific di-fferences between LDL-c target achievement in terms of 2016 goals, though there seems to be a trend when evaluating by 2019 recommendations (2016: 30.9% vs. 32.1%, p=0.410; 2019: 18.5% vs. 14.1%, p=0.078).
The most prevalent comorbidity was heart failure (82.5%), followed by chronic kidney disease and atri-al fibrillation in up to a third of patients (31.5% and 30.5%). As expected, patients with heart failure were older (71.8 ± 9.0 vs. 62.8 ± 8.6, p<0.001), as were those with atrial fibrillation (73.2 ± 8.7 vs. 67.4 ± 9.6, p<0.001) or chronic kidney disease (73.9 ± 8.4 vs. 66.9 ± 9.6, p<0.001). In the HF and AF groups, there was no gender difference (84.1% vs. 80.2%, p=0.116 and 31.4% vs. 29.1%, p=0.244 respectively), though more women had CKD than men (36.1% vs. 24.5%, p<0.001).
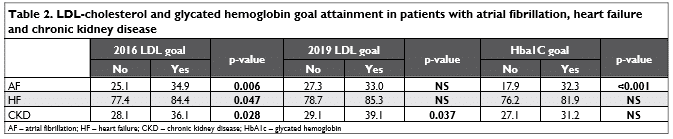
It is apparent that the subgroup of patients with atrial fibrillation had better control of lipid profi le pa-rameters (81.1 ± 30.5 mg/dL vs. 95.9 ± 40.7 mg/dL, p<0.001). In other words, more AF patients reached the 2016 LDL-c goal (34.9% vs. 25.1%, p=0.006); how-ever, when considering the 2019 goals, as the percen-tages drop to 18.5% and 14.8%, there is also a loss of statistical signifi cance (p=0.140).
Furthermore, lipid profile discrepancies among the subgroups of patients with and without heart failure or chronic kidney disease were noted (see Table 2); as such, patients with heart failure had better LDL-c goal attainment when compared to the 2016 but not the newer guidelines (37.1% vs. 27.2%, p=0.047 and 17.6% vs. 12.0%, p=0.125), while CKD patients maintained the differences irrespective of LDL-c goal (36.3% vs. 28.2%, p=0.028 and 18.9% vs. 13.0%, p=0.037).
DISCUSSION
Our study is the fi rst to assess LDL-c goal attainment in a Romanian population through the lens of the ne-wly published dyslipidemia guidelines and shows that while results were unsatisfactory before, even in very-high risk patients the new threshold only makes the task more daunting.
Out of all the very-high risk patients enrolled, only a third managed to reach LDL-c values below 70 mg/dL, a figure which dropped to under 1 in 5 patients when considering the 55 mg/dL target. Our findings are in accordance with literature data showing that despi-te publication of guidelines with clear treatment goals and availability of lipid-lowering therapies (LLTs), only few patients actually reach the desired level of control in terms of cholesterol and triglycerides9,10. The EU-ROASPIRE IV study evaluated cholesterol goal achie-vement in European patients and included a subgroup of Romanian patients; little under half had LDL-c valu-es below 100 mg/dL and only a fifth managed to reach the LDL-c goal (≤70 mg/dL) despite lipid-lowering the-rapy (LLTs) with high-intensity statin11.
In a large German cohort, only 19.5% of patient with preexisting cardiovascular disease were able to reach the desired LDL-c goal ≤70 mg/dL, with only a marginally better target achievement in diabetic pati-ents (33.5%) despite moderate- to high-intensity statin use10.
Studies have shown that patients are more likely to attain lipid goals with increasing age12,13, as did the patients in our cohort. However, it has also been re-ported that gender differences are relevant in terms of lipid goal achievement with diabetic men having lower LDL-c values under treatment.14,15 In our study popu-lation, no gender specific differences were registered in terms of LDL-c values or LDL goal achievement ir-respective of target (≤70 mg/dL or <55 mg/dL). Furt-hermore, there were no signifi cant gender differences in triglyceride levels, despite total cholesterol being higher in women, and the LDL to HDL ratio higher in men (see Table 1, Figure 1).
Failure to attain cholesterol goals draws attention to the physician, on the one hand, who may be reluc-tant to up-titrate LLT regiments due to safety con-cerns and the patient, on the other, who may not be adherent to lifestyle and medication recommendati-ons. It is somewhat alarming that only 1% of mode-rate-intensity statin patients undergo up-titration of treatment regimens and up to a quarter of patients on high-intensity statin discontinue treatment10. With the new targets in place we may expect an increase in the number of patients with recommendation for high-intensity statin and, potentially, an increase in the number of patients who discontinue treatment.
Several studies have tried to explain patient or physician reluctance to up-titrate statin dose through safety concerns.16 However, it has been shown that there is no “J”-curve associated with low LDL-c valu-es and muscle symptoms seem to occur with only a slight predominance, if any, in placebo-controlled ran-domized trials4,5. The newer guidelines recommend a stepwise approach to treatment: from maximal statin up-titration to addition of Ezetimibe and ultimately, PCSK9 inhibitors5. A comparison of LDL-c goal at-tainment spanning over a 6-year period in Europe and the Middle East has shown that due to the advent of high-intensity statin and ezetimibe an improvement in target achievement has been possible, at least in term of very-high risk patients7.
As polypharmacy is a known cause of treatment dis-continuation, it is somehow surprising that in our co-hort patients with various comorbidities such as atri-al fibrillation, heart failure or chronic kidney disease, which in themselves require specific drugs, were more likely to attain lipid goals. It is our opinion that patients who develop such conditions undergo more frequent follow-ups which in turn lead to better adherence to treatment.
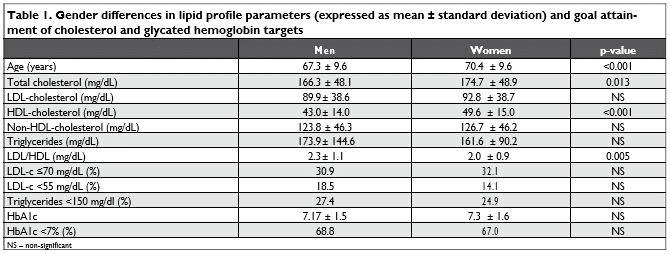
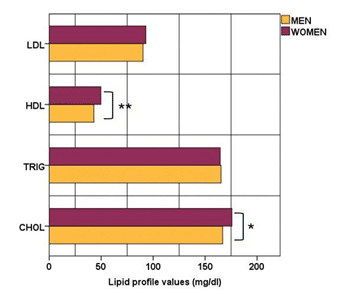
Figure 1. Mean values of lipid fractions shows no gender difference be-tween mean LDL-cholesterol values, though slightly higher HDL-cholester-ol in women and lower total cholesterol in men.
*statistically significant at a <0.05 level ; **statistically significant at a <0.001 level
STUDY LIMITATIONS
Data regarding treatment regimens was not available and, as is the case of cross-sectional studies, patient follow-up could not be performed in order to assess the effect of LLT up-titration, nor provide informati-on on treatment discontinuation. Finally, there was a lack of data on associated comorbidities, fi nancial and health insurance status, which could potentially limit patients’ adherence to treatment.
CONCLUSIONS
The gap between guideline recommendations and real world data has been made evident by a large number of studies to date, even considering previous LDL-c targets of ≤70 mg/dL. With the recently updated gui-delines that lower the treatment threshold in very-hi-gh risk patients to a further <55 mg/dL, we expect to see even lower goal attainment, as is the case with our cohort of diabetic, hypertensive and ASCVD patients. Hence, primary care physicians and specialists must redouble their efforts to control risk factor in patients at very-high cardiovascular risk.
Conflict of interest: none declared.
List of abbreviations used
AF – atrial fibrillation
ASCVD – atherosclerotic cardiovascular disease CKD – chronic kidney disease
CVD – cardiovascular disease HbA1c – glycated hemoglobin
HDL-c – high-density lipoprotein cholesterol HF – heart failure
LDL-c – low-density lipoprotein cholesterol LLTs – lipid-lowering therapies
References
1. Deaton C, Froelicher ES, Wu LH, Ho C, Shishani K, Jaarsma T. The global burden of cardiovascular disease. Eur J Cardiovasc Nur 2011; 10(2_suppl): S5-S13.
2. Smith DG. Epidemiology of dyslipidemia and economic burden on the healthcare system. Am J Manag Care 2007; 13: S68-71.
3. Hu FB. Globalization of food patterns and cardiovascular disease risk. Am Heart Assoc 2008; 118:1913–1914.
4. Giugliano RP, Pedersen TR, Park J-G, De Ferrari GM, Gaciong ZA, Ceska R, Toth K, Gouni-Berthold I, Lopez-Miranda J, Schiele F. Clini-cal efficacy and safety of achieving very low LDL-cholesterol con-centrations with the PCSK9 inhibitor evolocumab: a prespecifi ed secondary analysis of the FOURIER trial. Lancet 2017; 390(10106): 1962-71.
5. Mach F, Baigent C, Catapano AL, Koskina KC, Casula M, Badimon L, Chapman MJ, De Backer GG, Delgado V, Ference BA. 2019 ESC/EAS guidelines for the management of dyslipidaemias: Lipid modification to reduce cardiovascular risk. Atherosclerosis 2019; 290:140-205.
6. Catapano AL, Graham I, De Backer G, Wiklund O, Chapman MJ, Drexel H, Hoes AW, Jennings CS, Landmesser U, Pedersen TR. 2016 ESC/EAS guidelines for the management of dyslipidaemias. Eur Heart J 2016; 37(39): 2999-3058.
7. Gitt AK, Lautsch D, Horack M, Brudi P, Liu L, Ferrières J. Improvement of LDL-cholesterol goal attainment in high-risk patients in Europe and Middle East between 2008-09 and 2013-14: results of DYSIS and DYSIS II CHD. J Am Coll Cardiol 2017; 69(11 Supplement): 1702.
8. Kotseva K, Wood D, De Backer G, De Bacquer D, Pyörälä K, Reiner Ž, Keil U, Group ES. EUROASPIRE III. Management of cardiovascu lar risk factors in asymptomatic high-risk patients in general practice: cross-sectional survey in 12 European countries. Eur J Cardiovasc Prev Rehabil 2010; 17(5): 530-40.
9. Kuiper JG, Sanchez RJ, Houben E, Heintjes EM, Penning-van Beest FJ, Khan I, van Riemsdijk M, Herings RM. Use of Lipid-modifying Therapy and LDL-C Goal attainment in a high-cardiovascular-risk popula-tion in the Netherlands. Clin Ther 2017; 39(4): 819-27. e1.
10. Fox KM, Tai M-H, Kostev K, Hatz M, Qian Y, Laufs U. Treatment patterns and low-density lipoprotein cholesterol (LDL-C) goal at-tainment among patients receiving high-or moderate-intensity statins. Clin Res Cardiol 2018; 107(5): 380-8.
11. Reiner Ž, De Backer G, Fras Z, Kotseva K, Tokgözoglu L, Wood D, De Bacquer D, Investigators E. Lipid lowering drug therapy in pa-tients with coronary heart disease from 24 European countries–fi nd-ings from the EUROASPIRE IV survey. Atherosclerosis 2016; 246: 243-50.
12. Chi MD, Vansomphone SS, Liu I, Cheetham C, Green KR, Scott RD, Reynolds K. Adherence to statins and LDL-cholesterol goal attain-ment. Am J Manag Care 2014; 20(4): e105-12.
13. Ho L-T, Yin W-H, Chuang S-Y, Tseng W-K, Wu Y-W, Hsieh I-C, Lin T-H, Li Y-H, Huang L-C, Wang K-Y. Determinants for achieving the LDL-C target of lipid control for secondary prevention of cardiovas-cular events in Taiwan. PloS One 2015; 10(3): e0116513.
14. Parris ES, Lawrence DB, Mohn LA, Long LB. Adherence to statin therapy and LDL cholesterol goal attainment by patients with diabe-tes and dyslipidemia. Diabetes Care 2005; 28(3): 595-9.
15. Russo G, Pintaudi B, Giorda C, Lucisano G, Nicolucci A, Cristofaro MR, Suraci C, Mulas MF, Napoli A, Rossi MC. Age-and gender-relat-ed differences in LDL-cholesterol management in outpatients with type 2 diabetes mellitus. Int J Endocrinol 2015; 2015.
16. Rizzo M, Banach M, Montalto G, Mikhailidis DP. Lipid-lowering ther-apies and achievement of LDL-cholesterol targets. Arch Med Sci 2012; 8(4): 598.
 This work is licensed under a
This work is licensed under a