Ana Maria Balahura1,2, Anamaria Mihailescu3, Emma Weiss1,2, Cristina Japie2, Elisabeta Badila1,2, Daniela Bartos1,2
1 Clinical Department 5, „Carol Davila” University of Medicine and Pharmacy, Bucharest, Romania
2 Department of Internal Medicine, Emergency Clinical Hospital, Bucharest, Romania
3 „Prof. Dr. C.C. Iliescu” Emergency Institute for Cardiovascular Diseases, Bucharest, Romania
Abstract: Objective – Hypertension (HTN) pandemic is well recognized and with its low control rates can lead to HTN crisis and patients visiting excessively the Emergency Department (ED). The aim of the current study is to describe the frequency and pattern of hypertensive crises presenting at the ED of a tertiary care emergency hospital in Romania. Design and method – We retrospectively analysed all the charts of patients presenting at the ED during 1 month. We studied patients presenting for HTN defined as blood pressure (BP) ≥ 140/90 mmHg. We defined HTN emergency (EMG) as BP ≥ 180/120 mmHg with acute HTN mediated target organ damage (HMOD) and HTN urgency as BP ≥ 180/120 mmHg without HMOD (URG). In all other cases, BP ≥ 140/90 mm Hg was referred to as elevated BP (EBP). Results – 5898 pa-tients presented at the ED in 1 month, 293 pts were evaluated for HTN (4.96% from all presentations). 48.2% were true HTN crises. EMG (only12.2%) were older, with 91.8% known HTN, a higher number of comorbidities – higher prevalence of atrial fi brillation (p<0.005), chronic coronary syndromes (p<0.005), previous stroke (p 0.009) and dyslipidaemia (p<0.005). The most frequent acute HMOD were stroke (33.4%) and acute coronary syndrome (27.7%). Intravenous furosemide and enalaprilat were the most frequently used antihypertensive drugs. Conclusions – Hypertensive disease remains a frequent cause of ED presentations with only half of cases representing true urgencies or emergencies, overburdening the emergency health care system. Patients with true EMG represent a vulnerable category as they are older and have higher number of comorbidities.
Keywords: hypertensive crisis, hypertensive emergency, hypertensive urgency.
INTRODUCTION
Arterial hypertension (HTN) remains one of the ma-jor health problems around the world with an estima-ted global prevalence of 1.3 billion, between 30-45% of adult population suffering from HTN1. Romania is a country with a high prevalence of HTN with 45.1% of the adult population being hypertensive. Unfortuna-tely, the high prevalence is paralleled by a low control rate with only 30.8% of patients reaching the currently recommended blood pressure (BP) targets2,3.
Acute HTN crises are a direct consequence of po-orly treated or controlled HTN and are a frequent reason patients visit medical care facilities, overburde-ning the medical health care system4. A hypertensive crisis is a general term referring to situations with an acute increase in BP and can include HTN emergen-cies, defi ned as an acute severe increase in BP associ-ated with acute HTN mediated target organ damage (AHMOD), and HTN urgencies, defined as an increase in BP usually over 180/110 mmHg without AHMOD1,5.
The latest published consensus paper on hyper-tensive emergencies has renamed HTN urgency as uncontrolled HTN advocating that when AHMOD is absent, its long term prognosis is similar to stable patients that have uncontrolled HTN14-6. In light of this new definition, only a few patients should visit the ED and the vast majority should be treated in the pri-mary care settings. However, HTN pandemic is well recognized and with its low control rates can lead to acute or chronic increase in BP and patients visiting excessively the Emergency Department (ED). Moreo-ver, data are scarce on the proper management of an HTN emergency and clear protocols are still lacking4. Therefore, it is important to describe the prevalence and pattern of HTN crises that are managed in the ED in the real world settings4.
To the best of our knowledge, currently, there aren’t any data published describing the frequency, types and management practices of HTN crisis pre-senting at the EDs in Romania. Therefore, the aim of the current study is to describe the frequency and pattern of hypertensive crises presenting at the ED of a tertiary care emergency hospital in Romania. Mo-reover, we aimed at characterising the profile of the patient presenting for a HTN crisis, its risk factors, clinical presentations, as well as their medical manage-ment in the ED.
METHODS
Study design
This was a retrospective descriptive study evaluating patients older than 18 years old presenting with eleva-ted BP to the ED of a tertiary care emergency hospital from Bucharest, Romania, during one month – March 2018.
Study population, variables and measurements We retrieved complete demographic, clinical, paracli-nical and treatment data from the ED charts of pa-tients presenting for symptomatic or asymptomatic hypertension defined as BP ≥ 140/90 mmHg.
A history of physician-diagnosed diabetes mellitus (DM), chronic kidney disease (CKD), chronic coro-nary syndrome (CCS), dyslipidemia, obesity, atrial fibrillation and stroke was noted from the patient’s medical record file. Clinical symptoms were recorded from the physician’s initial assessment sheet. Electro-cardiograms were available for all patients and were used to diagnose atrial fibrillation.
Blood pressure readings, done with an automatic standardized BP measuring device, at different time in-tervals, were recorded from vital sheets.
We defined a hypertension emergency (EMG) as BP 180/120 mmHg with acute HMOD and HTN urgen-cy as BP ≥180/120 mmHg without HMOD (URG). In all other cases BP ≥140/90 mmHg was referred to as elevated BP (EBP).
Patient management was assessed by recording the list of medication from the treatment sheet attached inside the medical record file which includes type of drug, dose, the route and the time of administration.
Mean length of stay in the ED was recorded by calculating the time interval between the patient’s ad-mission time and discharge/admittance time from ED. Acute HMOD such as acute coronary syndromes, stroke, aortic dissection, HTN encephalopathy, malig-nant HTN and heart failure / pulmonary edema were recorded using the discharge summary notes filled by the ED consultant.
Statistical Analysis
The categorical variables were presented as counts and percentages, while continuous variables were presented as mean values ± standard deviation. The frequency of clinical and paraclinical characteristics in the groups was compared using two-by-two contin-gency table and analysed with chi-square 2 with Yates correction test. Continuous variables were compared using Student’s T-test or the Mann-Whitney U test, as appropriate to the distribution of the data. Two-sided p-values < 0.05 were considered significant.
Statistical analysis was performed with the Statis-tical Package for the Social Sciences (SPSS) 23.0 for Windows.
This study has been approved by the Ethics com-mittee of the Clinical Emergency Hospital Bucharest.
RESULTS
Demographic characteristics and risk factors From 5898 patients presented at the ED in one month, 293 presented for symptomatic or asymptomatic elevated BP (4.96% from all presentations). 48.2% were true HTN crises (2.39% from all ED presentations) while the reminder presented for EBP (2.57% of all ED presentations). Only 12.2% were EMG (0.61% from all ED presentations, 25.5% from HTN crisis) (Figure 1).
The baseline characteristics, risk factors and co-morbidities are depicted in Table 1.
The mean age of patients presenting for a true emergency (and non EBP) was 67.5±12.3 years, pa-tients in the EMG group being signifi cantly older than URG (p 0.02). In the EMG group, there were more patients previously diagnosed with HTN (p < 0.005) and they had a higher average number of comorbidities (0.01). In the EMG group significantly more patients had atrial fibrillation (AF) (p<0.005), chronic coronary syndromes (p<0.005), a previous stroke (p 0.009) and dyslipidaemia (p<0.005). There were no differences in sex distribution between EMG and URG.
Two thirds of patients were previously diagnosed with HTN. From the 205 previously known hyper-tensive patients, 83.4% were treated with an average of 2.1±0.9 antihypertensive drugs at home; however, patients in the EMG group had a signifi cantly lower rate of treatment compared to the URG group (45.4% versus 96%, p 0.002). Treated patients in the URG and EMG had a similar average number of antihypertensive drugs recommended at home. Angiotensin converting enzyme inhibitors (ACEIs) or angiotensin receptor blockers (ARBs) were the most frequent used anti-hypertensive drug classes in chronic therapy (44.0%), followed by beta blockers (34.8%) and indapamide (22.5%). The only difference between EMG and URG was the lower rate of ACEI/ARB usage in the EMG (Table 2).
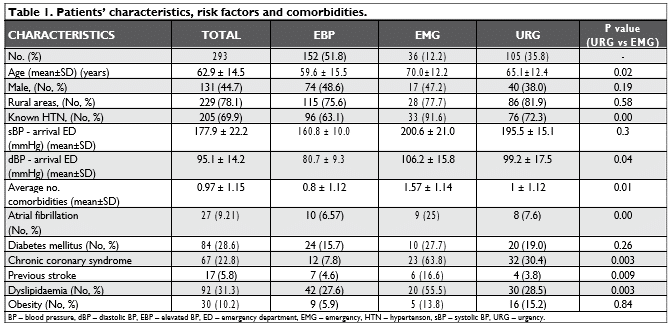
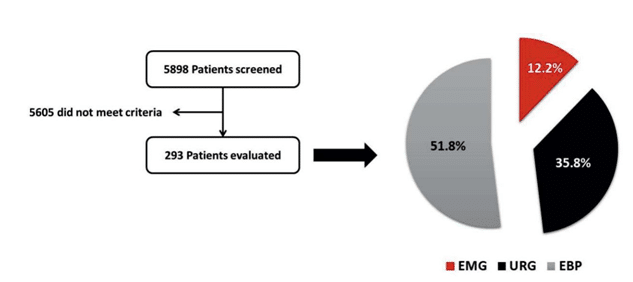
Figure 1. The study flow chart and distribution of patients presenting with hypertension. EBP – elevated blood pressure, EMG – emergency, URG – urgency.
Clinical presentation
The presenting symptoms and their frequency in HTN crises are listed in Table 2 and Figure 2. The most frequent presenting symptoms in the overall studied population were headache (26.9%) and dizziness (19.7%). However, in the EMG group, chest pain and dyspnoea were the most frequent symptoms and were signifi cantly more prevalent than in the URG group. Headache was a more frequent symptom in the URG group.
In the EMG, the most frequent AHMOD were stroke (ischemic plus haemorrhagic) (33.4%) and ACS (acute coronary syndrome, 27.7%) followed by heart failure (16.6%). HTN encephalopathy, aortic dissecti-on and malignant HTN were rarer (Figure 2).
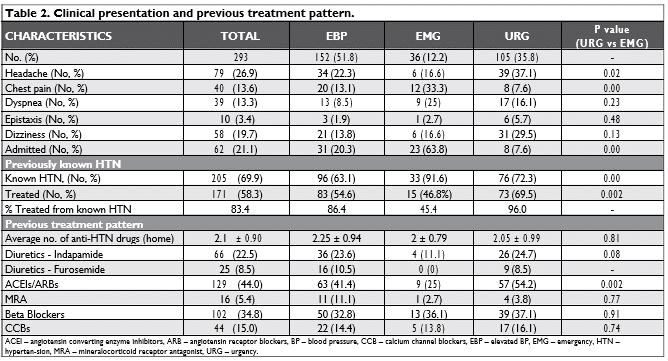
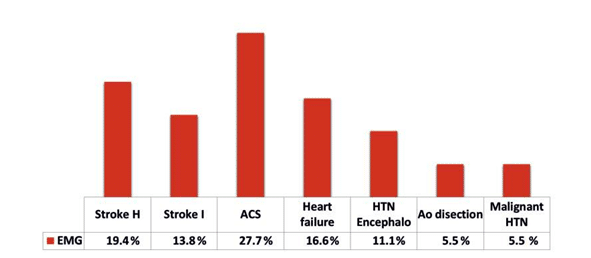
Figure 2. Frequency of acute hypertensive mediated organ damage in patients presenting with hypertensive emergencies. ACS – acute coronary syndromes, Encephalo – Encephalopathy, EMG – emergency, HTN – hypertension, H – haemorrhagic, I – ischemic.
ED management
The management patterns in the ED are summarized in the Figures 3-5. The average time spent in the ED was 218.7±26.5 min, without significant difference between EMG and URG. EBP patients spent less time in the ER. Most patients were discharged, only 21.1% were admitted. As expected, patients in the EMG had a significantly higher admittance rate (63.8% versus 7.6% URG, p < 0.005).
The mean systolic BP (sBP) upon arrival was 177.9±22.2 mmHg in the overall population, with no significant difference between URG and EMG. Howe-ver, upon leaving the ED, sBP remained higher in the EMG (153.1±22.1 versus 142.9±13.1 URG, p 0.02) even though sBP was significantly lowered compared with the initial value. Diastolic BP upon arrival was sig-nifi cantly higher in the EMG than URG group.
Treatment was administered in 100% of EMG pa-tients as opposed to only 79% of URG patients. Di-uretics (intravenous (iv) furosemide) were the most frequently used antihypertensive drug (139 (47.4 %)) in the ED with a surprisingly higher usage in the URG versus EMG (76 (72.3%) vs 20 (55.5%), p 0.06). ACEIs were the second most used drugs (64 (21.8%)) while nitroglycerine came in on the third place (13 (4.3%)). Nitroglycerine was more frequently used in the EMG group (19.4% versus 2.8% URG, p <0.005). Calcium channel blockers (2%), urapidil (0.003%) and clonidine (0.003%) were rarely used.
DISCUSSIONS
The present study provides an estimate of the preva-lence of hypertensive crises in an emergency depart-ment of a tertiary emergency hospital from Romania. These accounts for 2.39% from all ED presentations. However, EBP accounts for another 2.57% of ED pre-sentations overburdening the emergency care system. To the best of our knowledge, these findings have ne-ver been reported before in Romania and show that hypertensive crises represent an important and com-mon event in emergency medicine and require appro-priate resources for their diagnosis and treatment. Moreover, the fact that almost half of the presentation for elevated BP are in fact non-crisis situation points at an inappropriate management of HTN in the primary health care system.
Although EMG represents only 12.2% of all ED presentations for increased BP and one fourth of all hypertensive crises, they are by definition characteri-zed by end-organ damage such that the medical staff devotes a lot of time and resources to these patients. Our findings are in partial agreement with previous reported data on HTN crisis. In a large multicentre Italian study on hospital admissions for HTN crises in the ED, over a one year period, the prevalence of HTN crises was 0.46% from all clinico-surgical urgen-cies with 25.3% of them being EMG7. In another study done in a university emergency hospital from Brazil, the prevalence of HTN crisis was 0.5% from all clini-co-surgical emergencies, with 39.6% EMG8. Another study from an university hospital from Pakistan show-ed a prevalence of 1.8% HTN crisis from all emer-gency cases presenting at the ED9. These data show a significantly lower proportion of HTN crisis than the one reported in our study. This may be due to the different defi nitions used in these studies, a higher threshold of BP >220/120 mmHg being the cut-off for defining HTN crises in the ones reporting a lower prevalence. However, the proportion of EMG, which in all studies was defined as hypertension associated with acute HMOD, was the same (one fourth of all HTN crisis) suggesting that in fact our hospital is dea-ling with a higher proportion of HTN emergencies and urgencies than other centers around the world. The different health care system organisation and the high prevalence of hypertension and poor HTN control in Romania can account for these differences2. Nonethe-less, this should draw attention to the overburdening of the EDs and the emergency health care in Romania by HTN crises as well as non-crisis elevations in BP.
Other reports on this topic could enable us to com-pare the data from various areas of our country and add an epidemiological point of view on HTN crisis, which, unfortunately, cannot be estimated from the present study.
Patients with true EMG are older and have more previous history of HTN, dyslipidaemia, CCS, pre-vious stroke and AF suggesting a higher burden and a longer duration of disease, with significantly more chronic HMOD, factors probably contributing to the acute presentation with more severe HTN and acute HMOD. Almas et al. reported similar rates of comor-bidities as in our study for EMG as well as for URG patients even though they had a predominant male and younger population9. Another risk factor is older age which was associated with increasing risk of hyperten-sive emergency in some studies8,10. Moreover, poor BP control is associated with worse outcome in terms of target organ damage and there are studies showing that less effective BP control is an independent risk factor for ED presentation due to an HTN crisis11. Some studies have reported a percentage between 12.7 and 33 of patients with hypertensive crises who were unaware of their hypertensive status similar to our patients, which were previously unknown hyper-tensive more in the URG 27.7% then 8.4% in the EMG (p < 0.005)12,13. Unfortunately, we did not have any tool to assess previous control or proper adherence to antihypertensive therapy. Nonetheless, these fin-dings suggest that there is a need for increased aware-ness among the general population, hypertensive sub-jects and treating physicians to address this important issue.
Systolic BP upon arrival was not significantly diffe-rent while diastolic BP (dBP) was significantly higher in the EMG than the URG group. Even though some studies have reported significantly different sBP when presenting at the ED, Zampaglione et al have reported a significant difference only with the dBP, which has been reported to be greater in patients with EMG than URG, indicating greater peripheral vascular resistance in these cases and greater severity13. This supports the current concept that not the level of BP but the acute HMOD dictates the difference in outcome4. Mo-reover, both diastolic and systolic BP are associated with cardiovascular outcome in hypertensive patients and both measurements should be taken into account when evaluating a HTN patient14.
Acutely elevated BP can manifest as several clini-cal scenarios. In our study, headache and dizziness were the most frequent symptoms followed by chest pain and dyspnoea, as found in other studies. Only chest pain was significantly more frequent in the EMG group, as a sign of acute HMOD10,15. This implies that symptoms alone are not able to distinguish between emergencies and urgencies and highlight the need for a thorough evaluation prior to making a management decision.
EMG is defined by the presence of acute HMOD. In the large multicentre study by Pinna et al, the preva-lence of AHMOD was 30.9% acute pulmonary edema, 22% stroke, 17.9% myocardial infarction, 4.9% hyper-tensive encephalopathy7. In another study, the cere-brovascular and cardiovascular complications were the main HMOD with 58% stroke and 38% ACS plus heart failure10. Our study findings are in concordance with the data published thus far as we found that the majority had cardiovascular or cerebrovascular invol-vement. The clinical pattern of presentation of hyper-tensive crises at the ED are of great interest for the clinician as well as for the characterisation of disease course and estimating prognosis.
Treatment was administered in 100% of EMG pati-ents as opposed to only 79% of URG patients. Indeed, recent data suggests that referring patients for URG at the ED did not seem to improve cardiovascular outco-mes or BP control at 6 months hence the new recom-mendation of the current European position paper on management of HTN emergencies that URG should be renamed “uncontrolled BP” an treated as a non-crisis situation4,6.
Furosemide iv was the most frequently used anti-hypertensive drug, iv ACEIs were the second most used while nitroglycerine came in on the third pla-ce. Nitroglycerine was more frequently used in the EMG group in agreement with the high percentage of ACS and chest pain in this group. Calcium chan-nel blockers, urapidil and clonidine were rarely used. The European position paper on the management of HTN emergencies recommends that treatment in pa-tients with a hypertensive EMG be driven by the type of HMOD, and, although differences in preference and experience exist with regard to the use of intraveno-us BP-lowering medication, most EMG can be treated with either labetalol or nicardipine. The drugs recom-mended in this position paper are iv beta blockers,
CCB, iv nitrates, iv ACEI and clonidine. However, the discrepancy in the therapeutic management in our ED and the previously mentioned recommendations is mainly due to the unavailability of most of the iv antihypertensive drugs (except for furosemide, enalapri-lat, nitroglycerine and urapidil) in many parts of Roma-nia1,4. Therefore, this peculiar pattern of management is specifi c to our ED and is due to the local health care system problems. Nonetheless, the low usage of nitroglycerine and clonidine should alarm the clinici-ans treating HTN crisis that the treatment pattern can be optimized even in the settings of our health care system particularities.
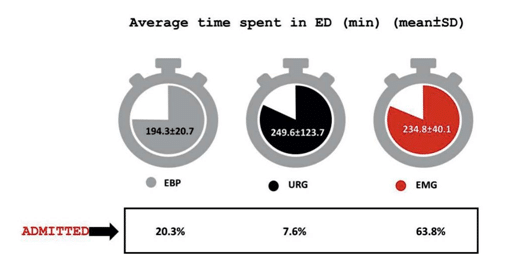
Figure 3. Graphic representation of time spent in the emergency department and admittance rate. EBP – elevated blood pressure, ED – emergency de-partment, EMG – emergency, URG – urgency.
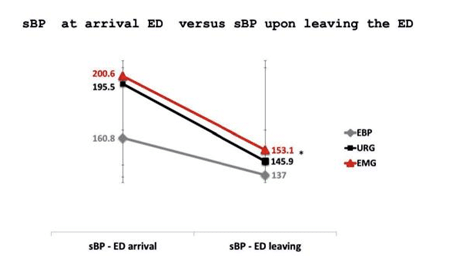
Figure 4. Changes in blood pressure between arriving and leaving the emergency department. BP – blood pressure, EBP – elevated BP, ED – emergency department, EMG – emergency, HTN – hypertension, sBP – systolic BP, URG – urgency. *p<0.05.
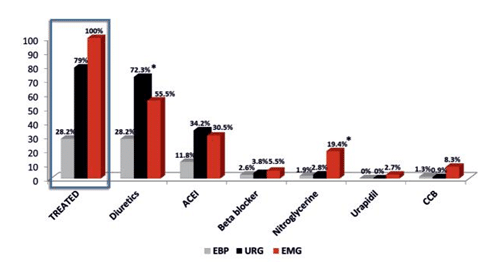
Figure 5. Frequency of antihypertensive drugs usage in the emergency department. ACEI – angiotensin converting enzyme inhibitors, BP – blood pressure, CCB – calcium channel blockers, EBP – elevated BP, EMG – emergency, URG – urgency. * p<0.05.
STUDY LIMITATIONS
Our study is a single-center report and its retrospecti-ve nature limits the data available for analysis. Moreo-ver, BP measurements were taken from the patients files and repeated measurements to confirm elevated BP were not available for all patients. Nonetheless, ED charts are medical and legal documents ensuring the correctness of the data and the final diagnosis written on the file was cross-checked to ensure that the pati-ents ware correctly classified.
Unfortunately, available treatment was occasio-nally restricted due to resource limitations; hence, the observed treatment strategies may be due not to physician preference, but rather medication availabi-lity. However, to the best of our knowledge, this is the first study reporting the frequency and pattern of HTN crisis presenting at the ED of a representative tertiary care emergency hospital from Bucharest, Ro-mania.
Even though it has limited external validity because the sample size is not representative for the entire population of Romania, this paper’s finding represent a valuable information for health care providers and health insurance agencies to establish a correct mana-gement strategy.
CONCLUSION
Hypertensive disease remains a frequent cause of ED presentations with only half of cases representing true urgencies or emergencies, overburdening the emer-gency health care system in Romania. Patients with true hypertensive EMG represent a vulnerable cate-gory as they are older, with a higher number of co-morbidities making them more likely to be admitted. Ischemic or haemorrhagic stroke and acute coronary syndromes are the most frequent types of end-organ damage in hypertensive emergencies. Treatment pat-tern at the ED is not aligned to the current European recommendation, iv furosemide and ACEIs being the most frequently used antihypertensive drugs.
Founding source: This work was possible due to the MODERNIZE project (Modernization of infra-structure in the center of research – development in minimally invasive interventional medical techniques in internal medicine and gastroenterology), funded by the National Authority of Scientific Research and Innovation, in the name of the Ministry of European Funds, through the Operational Program Increase of Economic Competitiveness, Priority axis 2 = Opera-tion 2.2.1 (POSCCE-A2-0.2.2.1- 2013-1), co-financed by the European Regional Development Fund.
Conflict of interest: none declared.
References
1. Williams, B., et al., 2018 ESC/ESH Guidelines for the management of arterial hypertension. European Heart Journal, 2018. 39(33): p. 3021-3104.
2. Dorobantu, M., et al., Perspectives on hypertension’s prevalence, treatment and control in a high cardiovascular risk East European country: data from the SEPHAR III survey. J Hypertens, 2018. 36(3): p. 690-700.
3. Dorobantu, M., et al., Hypertension prevalence and control in Ro-mania at a seven-year interval. Comparison of SEPHAR I and II sur-veys. J Hypertens, 2014. 32(1): p. 39-47.
4. van den Born, B.H., et al., ESC Council on hypertension position document on the management of hypertensive emergencies. Eur Heart J Cardiovasc Pharmacother, 2019. 5(1): p. 37-46.
5. Whelton, P.K., et al., 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/ APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detec-tion, Evaluation, and Management of High Blood Pressure in Adults. Journal of the American College of Cardiology, 2018. 71(19): p. e127.
6. Patel, K.K., et al., Characteristics and Outcomes of Patients Present-ing With Hypertensive Urgency in the Office Setting. JAMA Intern Med, 2016. 176(7): p. 981-8.
7. Pinna, G., et al., Hospital admissions for hypertensive crisis in the emergency departments: a large multicenter Italian study. PloS one, 2014. 9(4): p. e93542-e93542.
8. Martin V, H.É., Garcia E, Luizon MR. , Hypertensive Crisis Profile : Prevalence and Clinical Presentation. Arquivos Brasileiros de Car-diologia, 2004. 83(2): p. 131-136.
9. Almas, A., et al., Hypertensive Crisis, Burden, Management, and Outcome at a Tertiary Care Center in Karachi. International journal of chronic diseases, 2014. 2014: p. 413071-413071.
10. Vilela-Martin, J.F., et al., Hypertensive crisis: clinical–epidemiological profile. Hypertension Research, 2011. 34(3): p. 367-371.
11. Tisdale, J.E., M.B. Huang, and S. Borzak, Risk factors for hyperten-sive crisis: importance of out-patient blood pressure control. Family Practice, 2004. 21(4): p. 420-424.
12. Arhami Dolatabadi, A., et al., Prevalence of undiagnosed hyperten-sion in the emergency department. Trauma monthly, 2014. 19(1): p. e7328-e7328.
13. Zampaglione, B., et al., Hypertensive Urgencies and Emergencies. Hypertension, 1996. 27(1): p. 144-147.
14. Flint, A.C., et al., Effect of Systolic and Diastolic Blood Pressure on Cardiovascular Outcomes. New England Journal of Medicine, 2019. 381(3): p. 243-251.
15. Al-Bannay, R. and A.A. Husain, Hypertensive crisis. Clinical presenta-tion, comorbidities, and target organ involvement. Saudi Med J, 2010. 31(8): p. 916-20.
 This work is licensed under a
This work is licensed under a