Download PDF
https://doi.org/10.47803/rjc.2020.30.1.73
Horia Stefan Rosianu1, Razvan Olimpiu Mada1, Simona Oprita2, Adrian Stef3, Manuel Chira2, Catalin Aurelian Trifan2
1 Department of Cardiology, „Niculae Stancioiu” Heart Institute, Cluj-Napoca, Romania
2 Department of Cardiac Surgery, „Niculae Stancioiu” Heart Institute, Cluj-Napoca, Romania
3 Department of Anesthesiology, „ Niculae Stancioiu” Heart Institute, Cluj-Napoca, Romania
Abstract: Cardiac resynchronization therapy is a common option in adult patients with heart failure and conduction abnormalities. Specific selection criteria for pediatric population are lacking. We report the case of a 14-year-old boy with signifi cant pulmonary regurgitation subsequent to corrected tetralogy of Fallot and single chamber permanent pacing which presented with heart failure symptoms. Careful management was planned by a Heart Team including pediatric cardiologist, cardiac surgeon, interventional cardiologist and anesthesiologist. After undergoing cardiac surgery with complete correction of the pulmonary regurgitation and upgrade to a triple chamber pacing, the patient was discharged in good clinical status. Keywords: cardiac resynchronization therapy, heart failure, pediatrics.
Rezumat: Terapia de resincronizare cardiacă este o opţiune frecventă la pacienţii adulţi cu insufi cienţă cardiacă şi tul-burări de conducere. Criteriile specifice de selecţie pentru populaţia pediatrică lipsesc. Raportăm cazul unui băiat în vârstă de 14 ani cu insuficienţă pulmonară semnifi cativă secundară unei tetralogii Fallot corectate şi cardiostimulare permanentă monocamerală, care prezenta simptome de insuficienţă cardiacă. Managementul pacientului a fost planificat cu grijă de o echipă formată dintr-un cardiolog pediatru, chirurg cardiac, cardiolog intervenţionist şi anestezist. După ce a fost supus unei intervenţii chirurgicale cardiace cu corectarea completă a regurgitării pulmonare şi trecerea la stimulare tricamerală, pacientul a fost externat în stare clinică bună.
Cuvinte cheie: terapie de resincronizare cardiacă, insuficienţă cardiacă, pediatrie.
INTRODUCTION
Cardiac resynchronization therapy (CRT) has proven its effectiveness in appropriately selected candidates and became a standard of care in adult heart failure (HF) patients with conduction abnormalities. Current guidelines have specific recommendations regarding the selection of the CRT candidates, considering the clinical status, medical therapy, ECG and left ventricu-lar ejection fraction (LVEF)1.
Whether pediatric population might benefit from this invasive therapy or which are the selection crite-ria is not clear. All the big CRT studies have enrolled only adult patients2. In children, data come only from case reports or small case series. It is probably due to the lower incidence of heart failure in this age group, commonly limited to those with congenital heart di-sease3-6.
CASE REPORT
We report the case of a 14-year-old boy with corrected tetralogy of Fallot and permanent cardiac pacing (single chamber pacemaker, VVIR) due to postoperati-ve complete atrioventricular (AV) block which was re-ferred for exertional dyspnea and growth retardation. The patient underwent cardiac surgery with complete correction (ventricular septal defect correction with pericardial patch, infundibular resection and transan-nular patch) during early childhood (7-months-old). Due to subsequent complete AV block he received a single chamber rate adaptive pacemaker with epi-cardial lead placed on the right ventricular (RV) free wall (Figure 1A). Six years later the pacemaker was replaced with a similar device due to battery deple-tion. At that moment echocardiography revealed sig-nifi cant pulmonary regurgitation without right heart dilatation, and paradoxical movement of the septum due to RV pacing. After five years, the pacemaker re-ached ERI (elective replacement indicator) and a new device was implanted. Echocardiographic evaluation showed dilatation of the right chambers of the heart. Surgical correction of the pulmonary regurgitation was proposed but the patient delayed therapy. Three years later, he was referred to our center for the re-asons mentioned above. ECG showed sinus rhythm with AV dissociation and paced QRS complexes (QRS width=200ms with left bundle branch block (LBBB) morphology, Figure 1B). Compared to the previous echo examination, the right chambers were more di-lated, the mechanical dyssynchrony worse (Figure 2A) and the left ventricular (LV) stroke volume reduced. Considering the clinical status and the progressive dilatation of the right heart, the patient underwent cardiac surgery with implantation of a biological pros-thesis (Carpentier-Edwards Perimount Magna Ease) in pulmonary position (Figure 3A). During the same pro-cedure 2 additional epicardial leads were placed: one on the right atrium and the other on the LV. Those, alongside with the RV lead were connected to a triple chamber cardiac pacemaker (Figure 3A). The device was programmed DDD biventricular mode with LV anticipation (Fig 3B). The postoperative echocardiography illustrated synchronous contraction of both septum and LV postero-lateral wall (Figure 2B) with improved stroke volume. After a few days the patient was discharged in good clinical condition.
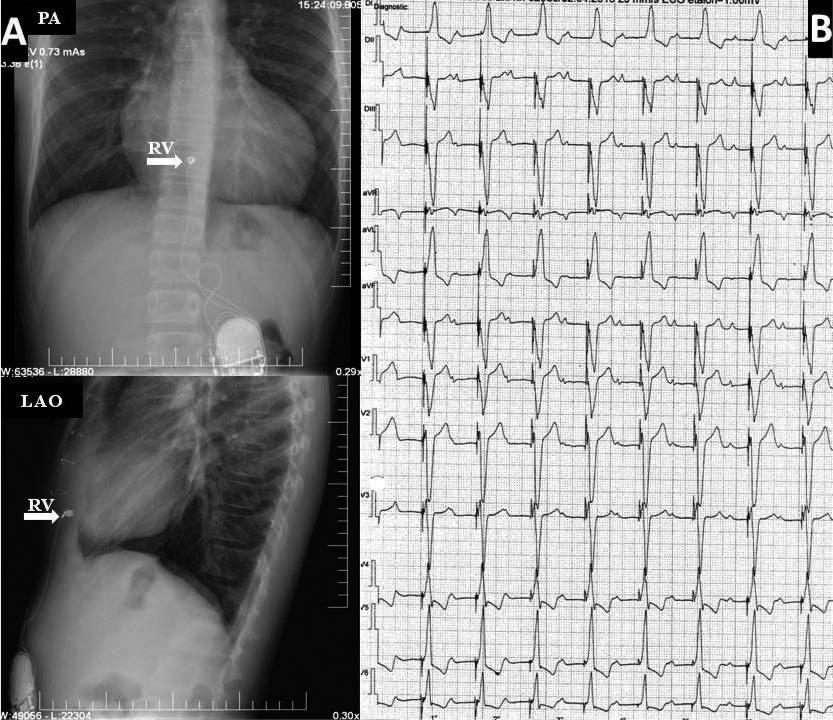
Figure 1. Single chamber cardiac pacing with epicardial lead on the right ventricle in tetralogy of Fallot with severe pulmonary regurgitation. Left panel (A): Chest X-ray. Right panel (B): Electrocardiogram. RV= right ventricular lead; PA=postero-anterior view; LAO=left anterior oblique.
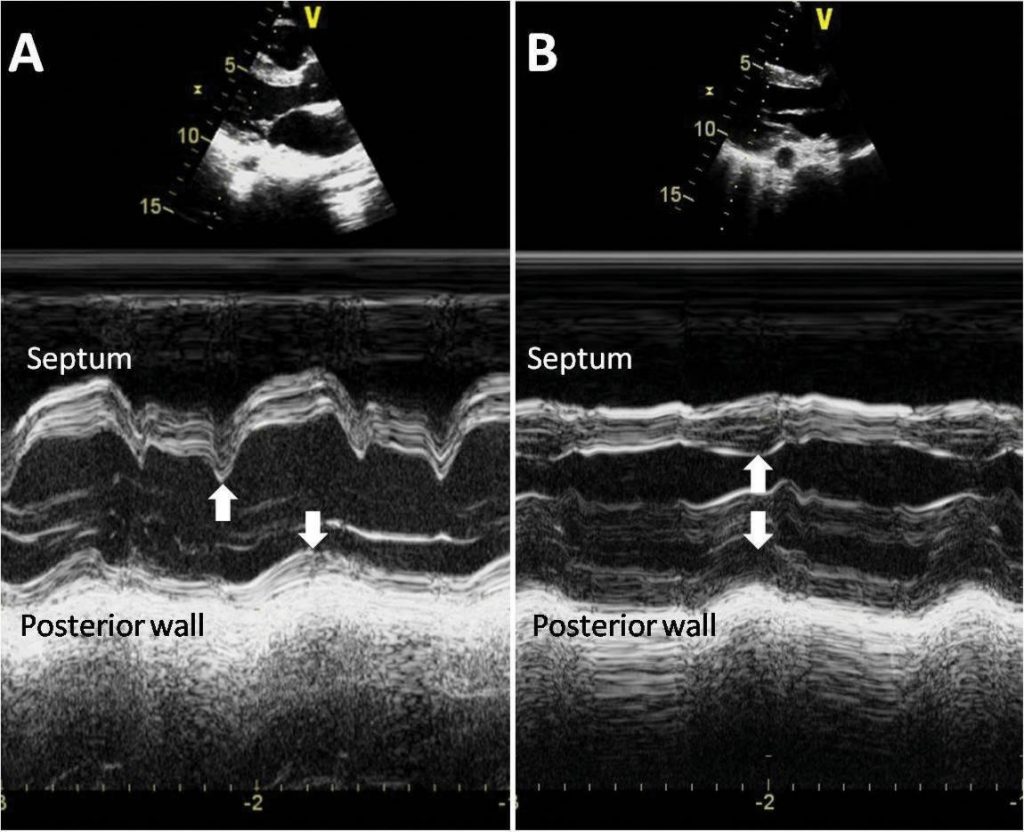
Figure 2. M-mode echocardiography in parasternal long axis view (PLAX) showing dyssynchronous/synchronous contraction of the interventricular sep-tum and posterior wall (white arrows). Left panel (A): before therapy. Right panel (B): after therapy.
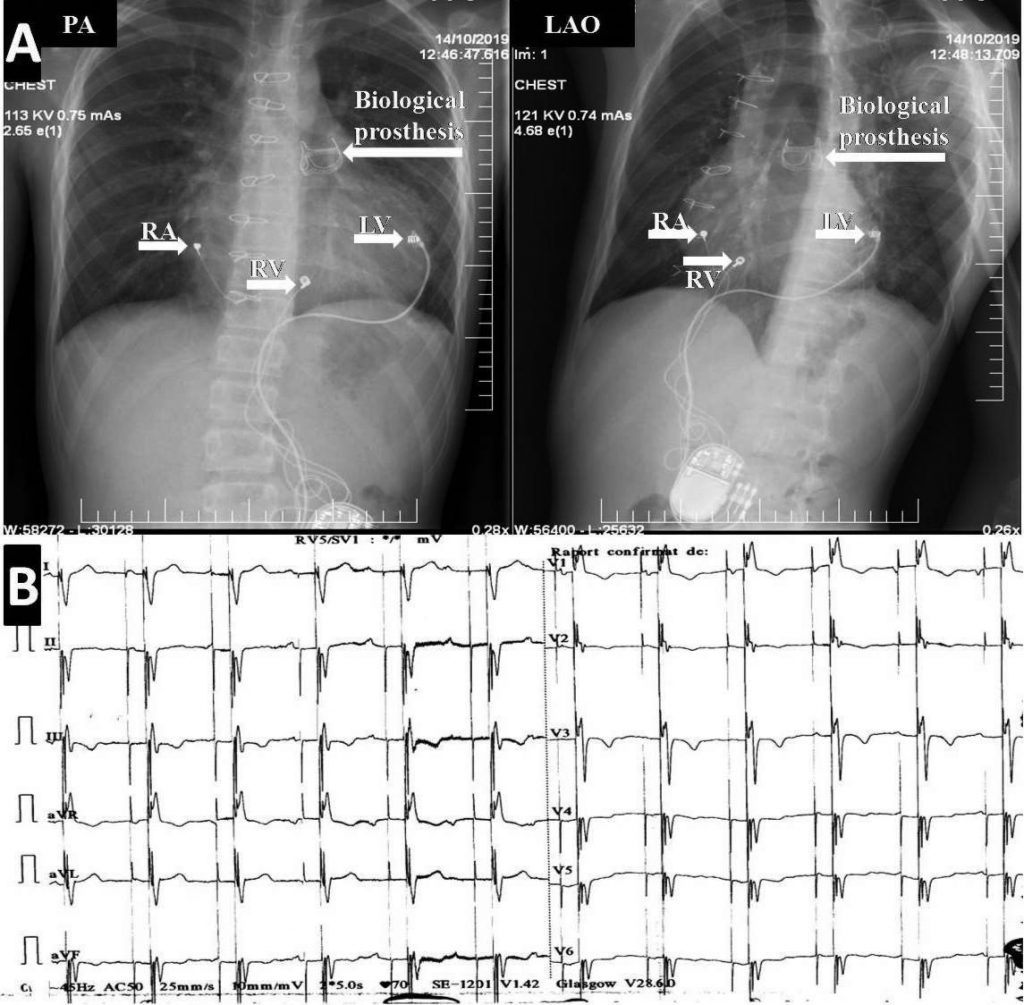
Figure 3. Cardiac resynchronization therapy with epicardial leads and Contegra graft in pulmonary position in repaired tetralogy of Fallot. Upper panel (A): Chest X-ray. Lower panel (B): Electrocardiogram. RA= right atrial lead; RV= right ventricular lead; LV= left ventricular lead; PA=postero-anterior view; LAO=left anterior oblique.
DISCUSSION
The patient presented is particular due to its complex cardiac condition that led to HF at a young age. Sig-nificant pulmonary regurgitation subsequent to com-plete correction of the tetralogy of Fallot (with tran-sannular patch) and the deleterious RV pacing were responsible for the development of the pathological condition. During surgery both conditions were cor-rected leading to improved cardiac function. Decision to perform upgrade from RV pacing to CRT in a pace-maker dependent pediatric patient was based on the ECG findings (QRS=200ms with LBBB morphology) associated to severe septal „bounce” on echocardiography. The echo exam was repeated after surgery while pacing either RV or both ventricles. The sep-tal “bounce” was found only during RV pacing. This finding suggests that responsible for the mechanical dyssynchrony was mainly the non-physiological car-diac pacing. However, we cannot underestimate the role of pulmonary regurgitation in the development of HF, especially in the context of dilated right heart cavities.
Cardiac pacing in pediatric population is usually con-fined to complete congenital or acquired AV block. The later develops after the surgical repair of a con-genital heart disease. Tetralogy of Fallot is most com-monly involved7. Its correction is a two-step procedu-re consisting of closure of the ventricular septal defect with a pericardial patch, infundibular resection and, usually, transanular patch. The later results in pulmo-nary regurgitation with increased RV preload, leading eventually to dilatation of the right heart chambers and HF. Once the RV dilates, it is recommended to treat pulmonary regurgitation either surgically (with a biological prosthesis) or interventional (transcatheter valve implantation) in order to avoid RV failure8.
Pediatric patients with complete AV block do usu-ally undergo single chamber pacemaker implantation with epicardial lead attached to the RV wall9. Kim et al have shown that up to 10% of patients developed HF after 10 years of RV pacing due to the atrioven-tricular and interventricular dyssynchrony10. There is a growing body of literature suggesting that develop-ment of pacemaker induced cardiomyopathy is highly dependent on the lead position. LV apical/midwall pacing appears to preserve better the cardiac function compared to RV pacing9.
CRT is increasingly used for adult patients with HF and reduced ejection fraction who have conduction abnormalities. Restoration of both atrioventricular and interventricular synchrony usually results in im-proved cardiac performance and functional capacity1,2. However, up to one third of patients who undergo CRT according to current guideline criteria are non-responders to the therapy. New parameters for pa-tient selection and CRT optimization are still under research11,12.
Specific criteria for pediatric population are lacking. There are not too many children meeting the CRT criteria from adults. First of all, NYHA functional class was designed for adults. It is not clear if it’s suitable for children considering the particular metabolism and physical activity that varies even between age groups. Secondly, QRS duration is changing with age. As a con-sequence, it is not unusual to have mechanical dyssyn-chrony even when QRS <120ms. Thirdly, adults do usually have LBBB QRS morphology, while in pediatric population right bundle branch block morphology is prevalent. This is due to the fact that children with HF have frequently a congenital heart disease. Moreo-ver, in this specific subgroup, evaluation of the LVEF is more difficult due to the complex anatomy2-6.
Conflict of interest: none declared.
References
1. Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland GF, Coats AJS, Falk V, González-Juanatey JR, Harjola VP, Jankowska EA, Jes-sup M, Linde C, Nihoyannopoulos P, Parissis JT, Pieske B, Riley JP, Rosano GMC, Ruilope LM, Ruschitzka F, Rutten FH, Van der Meer P, Filippatos G, McMurray JJV, Aboyans V, Achenbach S, Agewall S, Al-Attar N, Atherton JJ, Bauersachs J, Camm AJ, Carerj S, Ceconi C, Coca A, Elliott P, Erol Ç, Ezekowitz J, Fernández-Golfín C, Fitzsi-mons D, Guazzi M, Guenoun M, Hasenfuss G, Hindricks G, Hoes AW, Iung B, Jaarsma T, Kirchhof P, Knuuti J, Kolh P, Konstantinides S, Lainscak M, Lancellotti P, Lip GYH, Maisano F, Mueller C, Petrie MC, Piepoli MF, Priori SG, Torbicki A, Tsutsui H, Van Veldhuisen DJ, Windecker S, Yancy C and Zamorano JL. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Devel-oped with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail. 2016;18(8):891-975.
2. Linde C, Ellenbogen K, McAlister FA. Cardiac resynchronization therapy (CRT): Clinical trials, guidelines, and target populations. Hear Rhythm. 2012;9(8 SUPPL.):S3.
3. Batra A, Balaji S. Cardiac Resynchronization Therapy in Children. Curr Cardiol Rev. 2009;5(1):40-44.
4. Motonaga KS, Dubin AM. Cardiac resynchronization therapy for pe-diatric patients with heart failure and congenital heart disease: a re-appraisal of results. Circulation. 2014;129(18):1879-1891.
5. Uebing A, Gibson DG, Babu-Narayan SV, Diller GP, Dimopoulos K, Goktekin O, Spence MS, Andersen K, Henein MY, Gatzoulis MA and Li W. Right ventricular mechanics and QRS duration in patients with repaired tetralogy of Fallot: Implications of infundibular disease. Cir-culation. 2007;116(14):1532-1539.
6. HILL A, SILKA M, BAR-COHEN Y. Cardiac Resynchronization Therapy in Pediatrics. J Innov Card Rhythm Manag. 2018;9(8):3256-3264.
7. Singh HR, Batra AS, Balaji S. Pacing in children. Ann Pediatr Cardiol. 2013;6(1):46-51.
8. Villafañe J, Feinstein JA, Jenkins KJ, Vincent RN, Walsh EP, Dubin AM, Geva T, Towbin JA, Cohen MS, Fraser C, Dearani J, Rosenthal D, Kaufman B and Graham TP. Hot Topics in Tetralogy of Fallot. 2013.
9. Janoušek J, Van Geldorp IE, Krupičková S, Rosenthal E, Nugent K, Tomaske M, Früh A, Elders J, Hiippala A, Kerst G, Gebauer RA, Kubuš P, Frias P, Gabbarini F, Clur SA, Nagel B, Ganame J, Papagi-annis J, Marek J, Tisma-Dupanovic S, Tsao S, Nürnberg JH, Wren C, Friedberg M, De Guillebon M, Volaufova J, Prinzen FW and Delhaas T. Permanent cardiac pacing in children: Choosing the optimal pacing site: A multicenter study. Circulation. 2013;127(5):613-623.
10. Kim JJ, Friedman RA, Eidem BW, Cannon BC, Arora G, Smith EOB, Fenrich AL and Kertesz NJ. Ventricular function and long-term pac-ing in children with congenital complete atrioventricular block. J Cardiovasc Electrophysiol. 2007;18(4):373-377.
11. Mada RO, Lysyansky P, Duchenne J, Beyer R, Mada C, Muresan L, Rosianu H, Serban A, Winter S, Fehske W, Stankovic I and Voigt JU. New Automatic Tools to Identify Responders to Cardiac Resyn-chronization Therapy. J Am Soc Echocardiogr. 2016;29(10).
12. Dauw J, Martens P, Mullens W. CRT Optimization: What Is New? What Is Necessary? Curr Treat Options Cardiovasc Med. 2019;21(9).
 This work is licensed under a
This work is licensed under a