Download PDF
https://doi.org/10.47803/rjc.2020.30.2.236
Dan F. Filip1, Gabriela Kozma1, Calin F. Pop1
1 Laboratory of Angiography and Cardiac Catheterization, „Dr. Constantin Opris” Emergency County Hospital, Baia Mare, Romania
Abstract: Objectives – The aim of this study was to describe our experience with endovascular treatment in critical limb ischaemia and to bring new follow-up data about these patients with initial successfully revascularization. Methods – A retrospective study of 181 patients with critical limb ischaemia, with successful endovascular treatment in our institution was performed. We followed death, reintervention and amputation rates during a mean period of 55.1 ± 8.2 months. Results – The mean age of the patients was 65.2±11.6 years. Of these patients, 66.3% were males, 38.1% diabetics, 51.4% active smokers, 21% with chronic kidney disease, 32.6% with other clinical forms of peripheral artery diseases. The final treatment was stenting in 31.5% of cases and balloon angioplasty alone in the rest of the cases. Treated arteries were in the femoral-popliteal segment – 55.6%, aorto-iliac segment – 31.4% and infrapopliteal segment – 13%. 27.6% of the patients underwent procedures on more than one arterial segment. During follow up 11 deaths occurred (6.1%), 27 patients (14.9%) underwent reinterventions for revascularization (endovascular or surgical) and 31 patients (17.1%) suffered further amputations. Conclusions – Despite a certain rate of death, amputation and reintervention, our results suggest that endovascular approach in critical limb ischaemia can be an efficient and feasible treatment option if its results are optimal at the time of implementation.
Rezumat: Obiective – Scopul prezentului studiu a fost să descrie experienţa autorilor în ceea ce priveşte terapia en-dovasculară în ischemia critică a membrului inferior şi de a duce noi date de follow-up despre aceşti pacienţi revascularizaţi efi cient iniţial. Metodă – Am efectuat un studiu retrospectiv pe 181 de pacienţi cu ischemie critică de membru inferior re-vascularizaţi eficient în instituţia noastră. Am urmărit ratele de deces, reintervenţie şi amputaţie pe o perioadă medie de 55,1± 8,2 luni. Rezultate – Vârsta medie a pacienţilor a fost 65,2±11,6 ani. Dintre aceştia, 66,3% sunt bărbaţi, 38,1% diabetici, 51,4% fumători activi, 21% cu boală cronică renală, 32,6% cu alte forme clinice de boli arteriale periferice. Tratamentul final a fost stentarea în 31,5% dintre cazuri şi doar angioplastia cu balon pentru celelalte cazuri. Arterele revascularizate aparţineau segmentului femuro-popliteal – 55,6%, segmentului aorto-iliac – 31,4% şi celui infrapopliteal – 13%. La 27,6% dintre pacienţi s-au efectuat proceduri pe mai mult de un segment arterial. Pe parcursul urmăririi s-au înregistrat 11 decese (6,1%), 27 de pacienţi (14,9%) au necesitat reintervenţii pentru revascularizare (endovasculară sau chirurgicală) şi 31 de pacienţi (17,1%) au suferit amputaţii ulterioare. Concluzii – În ciuda unor anumite rate de deces, amputaţie şi reintervenţie, rezultatele noastre sugerează că abordarea endovasculară poate fi o opţiune terapeutică eficientă şi fezabilă în ischemia critică a membrului inferior dacă rezultatul final este optim la momentul implementării iniţiale.
INTRODUCTION
Recent data in literature demonstrated a continuous increase in atherosclerotic burden which signifies an increased hazard of serious cardiovascular disorders1. Although peripheral arterial disease (PAD) affects 10 to 15% of the general population, it has often received less attention than other atherosclerotic diseases2. Critical limb ischaemia (CLI) is not a common form of PAD, accounts for just 1 to 3% of all patients with PAD1,3, but it is very important clinical condition, the most severe, with significant impact on amputation rates, quality of life, cardiovascular morbidity and mortality. Unfortunately, the randomised trials in this field are lacking and there are large discrepancies between the reported results of arterial reconstruction, which can influence the management of this patients.
OBJECTIVES
The aim of this study was to describe our experience with endovascular treatment in CLI and to bring new follow-up data about these patients with initial suc-cessfully revascularization.
METHODS
We performed a retrospective study on patients with CLI, admitted in our institution between February 2012 and February 2020, which have been invasively explored by angiography and then underwent successful endovascular treatment (balloon angioplasty alone or stenting). Initial characteristics of patients were obtained from hospital’s observation files and other medical documents attached there (medical letters, ultrasound bulletins, data from hospital’s computer system). Technical data about the invasive diagnosis and endovascular management were obtained from Cath Lab’s files and by reviewing the angiographic films. An arterial revascularization has been considered successful if the residual stenosis was bellow 50%, the distal flow was improved, the symptomatology was improved and the patients were discharged without amputations or procedural complications that could jeopardize the limb’s integrity or patients life. We followed death, reintervention and amputation rates. Follow up was made collaborating with referring physicians, general practitioners, by phone call directly to patients or by reviewing the hospital’s computer system. Recording deaths, we also try to identify if the cause was related with the evolution of critical limb ischaemia or other events occurred. Reintervention was considered every arterial revascularization made for new symptoms of CLI. We considered both endo-vascular and surgical reintervention, in index limb and in contralateral limb, same arterial segment that was revascularized first time and other arterial segments that needed subsequent revascularization. Amputation, irrespective of the limb, has been considered minor if it was performed bellow the ankle and major if performed above this level. In this study’s data base we included only patients with complete information, regarding both initial revascularization and follow up moment.
RESULTS
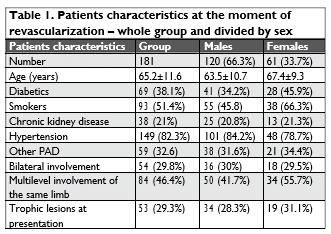
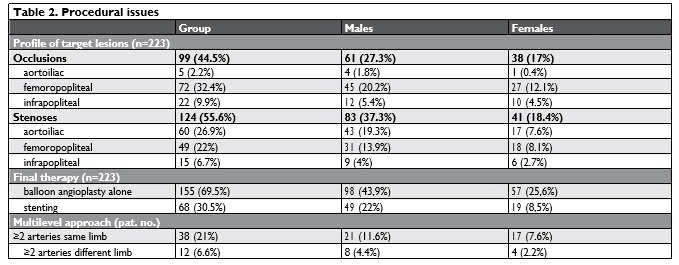
The study embedded 181 patients with CLI treated efficiently by endovascular approach, with mean follow up period: 53.4 ± 8.2 months. Patients initial characteristics are figured in Table 1. We also mention that at discharge all patients have received dual antiplatelet therapy (between one month and one year depending on the endovascular procedure), maximum tolera-ted statin dose and treatment of associated diseases according to specialized recommendations. In our institution we treated a number of 223 ar-teries, distributed as follows: 65 (29.1%) arteries in aortoiliac segment, 121 (54,2%) arteries in femoropopliteal segment and 37 (16.7%) infrapopliteal arteries. The lesions were type A, B and C (TASC II classifi – cation4), but simply they can be divided in stenoses (55.6%) and occlusions (44.4%). The final therapy was balloon angioplasty alone in 155 (69.5%) arteries and stenting in 68 (30.5%) arteries. Thirty-eight (21%) patients underwent procedures on 2 or more arteries in different segments of the same limb and 12 (6.6%) patients underwent procedures on 2 or more arteries on both inferior limbs. Procedural issues are detailed in Table 2. In the aortoiliac segment 63 of 65 lesions were stented and the remaining 2 underwent balloon angioplasty alone. In the femoropopliteal segment 109 lesions underwent balloon angioplasty alone and the remaining 13 were stented. The whole 37 infrapoplite-al arteries were treated with balloon angioplasty. The arterial approach used for the revasculariza-tion procedures was as follows: antegrade femoral – 106 (56.1%) punctures (usually used for revascularization of superficial femoral artery, popliteal artery and infrapopliteal segment), left brachial – 42 (22.2%) punctures and retrograde femoral – 28 (14.8%) punc-tures (usually used for revascularization of aortoiliac segment), femoral contralateral – 11 (5.8%) punctures and popliteal – 2 (1%) punctures.
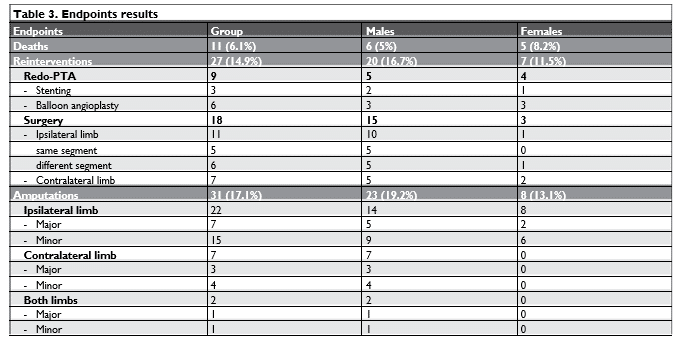
Results of the endpoints were: deaths – 11 patients (6.1%), reinterventions – 27 patients (14.9%), amputations – 31 patients (17.1%). Details are presented in Table 3.
Of the recorded 11 deaths only 2 (1.1%) were due to CLI. Both patients (1 male and 1 female), after optimal endovascular revascularization of a superficial fe-moral artery occlusion, refused segmental amputation of the necrotic forefoot, which led to septic shock and death in the end. The other deaths were due to cau-ses unrelated to CLI, like neoplasia, enteromesenteric infarction, sudden cardiac death, car crash.
Endovascular reinterventions were performed in the majority of cases for „de novo” lesions, but we had 1 procedure performed for an intra bare metal stent restenosis at the level of superficial femoral artery and 2 endovascular reinterventions performed after restenosis post balloon angioplasty alone in femoropoplite-al segments. Surgical revascularizations were performed for three categories of patients: “de novo” lesions, restenosis after initial endovascular revascularization and hybrid approach. In the first two categories, surgery was performed for TASC D lesions or for failed angioplasty attempt. In the hybrid approach scenario, we had 5 patients (2.8%) with multilevel involvement, in which after optimal endovascular revascularization of the aortoiliac segment, due to persistent ischemia surgery was performed for type D lesions in the femoropopliteal segment (usually long, very calcified superficial femoral artery occlusions) with subsequent good results.
Considering that 29.3% of patients presented with tissue loss, fortunately, of the 31 amputations recor-ded, 20 were minor (11%), usually a toe with trophic lesion at presentation and good delimitation of the necrosis after revascularization. Major amputations (6.1%) were performed due to extensive progression of the disease, when the lesions had no endovascular or surgical solution, or limb’s viability was lost due to late presentation.
DISCUSSIONS
As the 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Artery Diseases outlines, early recognition of CLI’s signs and referral to a vascular multi-disciplinary team are mandatory for limb salvage4. The same guideline clearly highlights that revascularization is indicated whenever feasible4. So, in our time we can consider that arterial revascularization is the corner-stone of treatment to prevent extremity loss1. Options for revascularization include endovascular, surgical and hybrid revascularization (as a combination of endovascular and surgical interventions). The BASIL trial (Bypass versus Angioplasty in Severe Ischaemia of the Leg) is, at the moment, the only randomized trial published that directly compared endovascular revascularization to open surgery in CLI patients5. At 2 years there was no significant difference between endovascular therapy and surgery regarding amputation-free survival5. BASIL-2 and BEST-CLI, other trials on the same topic, are still on going6,7. Due to significant technological advances in endovascular area and considering the more invasiveness, the risks of morbidity and mortality associated with surgery, nowadays, there is a significant trend toward „endovascular first” approach in the treatment of CLI8.
Faglia et al. performed a prospective study on 993 diabetic patients with CLI treated by successfully peripheral angioplasty (PTA) with a mean follow-up of 26 ± 15 months9. During follow-up 119 (12%) patients died, 17 (1.7%) major amputations were carried, clinical restenosis was observed in 87 (8.8%) patients and the 5 years primary patency was 88%9. Our data resembles with this study’s conclusions allowing us to consider that PTA as first choice revascularization technique is feasible, with low mortality, infrequent re-stenosis and potential of repetition when needed.
We reported a rate of limb salvage of 82,9% (amputation free) for our surveillance time. The study of Dosluoglu et al compared the outcome of endovascular revascularization, open surgery and hybrid revascularization on 654 patients, 770 limbs with symptomatic lower extremity occlusive disease (67% CLI)10. Limb salvage rates in patients with critical limb ischemia were similar in the endovascular (12- and 36-month; 86% ± 2% and 80% ± 3%), hybrid (94% ± 4% and 80% ± 7%), and open groups (80% ± 3% and 74% ± 4%) 10. Almost identical survival rates were reported in this cohort. The 12-, 36-, and 60-month survival in the open group was 80% ± 3%, 65% ± 4%, and 45% ± 4%, in endovascular group was 83% ± 2%, 63% ± 3%, and 43% ± 5%, and in the hybrid group was 80% ± 4%, 64% ± 5%, and 49% ± 7% (P= .963)10. During a mean follow up period of 53.4 ± 8.2 months we encountered a survival rate of 93.9%, much favourable in the male’s group.
A meta-analysis of infrapopliteal angioplasty for CLI, based on data retrieved from 30 articles, published for 1 and 36 months a survival rate of 98.3% ± 0.7% and 68.4% ± 5.5%, and limbs salvage rates of 93.4% ± 2.3% and 82.4% ± 3.4%, respectively11.
CONCLUSIONS
Despite a certain rate of death, amputation and re-intervention, our results suggest that endovascular approach in CLI can be an efficient and feasible treatment option if its results are optimal at the time of implementation. Multidisciplinary teams should have the treatment decision of CLI patients: endovascular, surgical or hybrid revascularization on individualized approach. Although it is well known that arterial revascularization is the most important item of CLI treatment, further studies are needed to clarify witch procedure is superior and to identify the factors that influence the management of these patients.
Conflict of interest: none declared.
References
1. Ahmet Yuksel, Yusuf Velioglu, Mustafa Cagdas Cayir, Gencehan Kumtepe, and Orcun Gurbuz: Current Status of Arterial Revascu-larization for the Treatment of Critical Limb Ischemia in Infrainguinal Atherosclerotic Disease. Int J Angiol. 2018 Sep; 27(3): 132–137.
2. Gerhard-Herman M D, Gornik H L, Barrett C et al. 2016 AHA/ ACC guideline on the management of patients with lower extremity peripheral artery disease: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. J Am Coll Cardiol. 2017;69(11): e71–e126.
3. Chung J, Modrall J G, Valentine R J. The need for improved risk strat-ifi cation in chronic critical limb ischemia. J Vasc Surg. 2014;60(06): 1677–1685.
4. Aboyans V, Ricco J-B, Bartelink M-L E L et al. 2017 ESC Guide-lines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS): Document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extrem-ity arteries. Endorsed by: the European Stroke Organization (ESO). The Task Force for the Diagnosis and Treatment of Peripheral Ar-terial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS). European Heart Journal, Volume 39, Issue 9, 01 March 2018, Pages 763–816, https:// doi.org/10.1093/eurheartj/ehx095
5. Bradbury AW, Adam DJ, Bell J, Forbes JF, Fowkes FG, Gillespie I, Ruckley CV, Raab GM; BASIL trial Participants. Bypass versus An-gioplasty in Severe Ischaemia of the Leg (BASIL) trial: An intention-to-treat analysis of amputation-free and overall survival in patients randomized to a bypass surgery-first or a balloon angioplasty-fi rst revascularization strategy. J Vasc Surg. 2010 May; 51 (5 Suppl): 5S-17S. doi: 10.1016/j.jvs.2010.01.073.
6. Popplewell MA, Davies H, Jarrett H, Bate G, Grant M, Patel S, Mehta S, Andronis L, Roberts T, Deeks J, Bradbury A; BASIL-2 Trial Inves-tigators. Bypass versus angioplasty in severe ischaemia of the leg – 2 (BASIL-2) trial: study protocol for a randomised controlled trial. Tri-als. 2016 Jan 6; 17:11. doi: 10.1186/s13063-015-1114-2.
7. Farber A, Rosenfield K, Menard M. The BEST-CLI trial: a multidisci-plinary effort to assess which therapy is best for patients with critical limb ischemia. Tech Vasc Interv Radiol. 2014 Sep; 17(3): 221-4. doi: 10.1053/j.tvir.2014.08.012.
8. Shishehbor MH, White CJ, Gray BH, Menard MT, Lookstein R, Rosenfi eld K, Jaff MR. Critical Limb Ischemia: An Expert Statement. J Am Coll Cardiol. 2016 Nov 1; 68(18):2002-2015.
9. Faglia E, Dalla Paola L, Clerici G, Clerissi J, Graziani L, Fusaro M, Gabrielli L, Losa S, Stella A, Gargiulo M, Mantero M, Caminiti M, Ninkovic S, Curci V, Morabito A. Peripheral angioplasty as the fi rst-choice revascularization procedure in diabetic patients with critical limb ischemia: prospective study of 993 consecutive patients hospi-talized and followed between 1999 and 2003. Eur J Vasc Endovasc Surg. 2005 Jun; 29(6):620-7. Epub 2005 Mar 28
10. Dosluoglu HH, Lall P, Cherr GS, Harris LM, Dryjski ML. Role of sim-ple and complex hybrid revascularization procedures for symptom-atic lower extremity occlusive disease. J Vasc Surg. 2010 Jun; 51(6): 1425-1435.e1. doi: 10.1016/j.jvs.2010.01.092.
11. Romiti M, Albers M, Brochado-Neto FC, Durazzo AE, Pereira CA, De Luccia N. Meta-analysis of infrapopliteal angioplasty for chronic critical limb ischemia. J Vasc Surg. 2008 May; 47(5): 975-981. doi: 10.1016/j.jvs.2008.01.005. Epub 2008 Apr 18.
 This work is licensed under a
This work is licensed under a